Uma paciente de 21 anos, previamente hígida, não tabagista, procurou o serviço de emergência com queixa de aumento recente e progressivo do volume da face, região cervical e tórax (Figura 1). Entretanto, negava dor, dispneia ou disfagia no momento da internação. Relatou quadro breve de odinofagia na semana anterior quando, durante um episódio de tosse, referiu forte dor retroesternal, de caráter dissecante, que aliviou em poucos minutos e, desde então, não apresentara quaisquer outros sintomas além do aumento de volume anteriormente descrito.
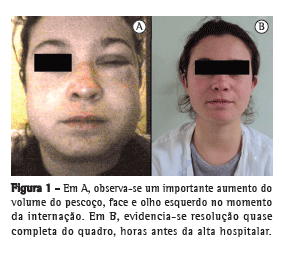
O exame físico evidenciou extenso enfisema subcutâneo, desde o apêndice xifoide até os músculos temporais, incluindo todo o pescoço e face. A percussão e a ausculta pulmonar não apresentavam alterações. À ausculta cardíaca, notou-se a presença do sinal de Hamman (estertores crepitantes ou bolhosos, associados ao batimento cardíaco) em qualidade crepitante. A oroscopia, assim como o restante do exame físico, mostrou-se normal.
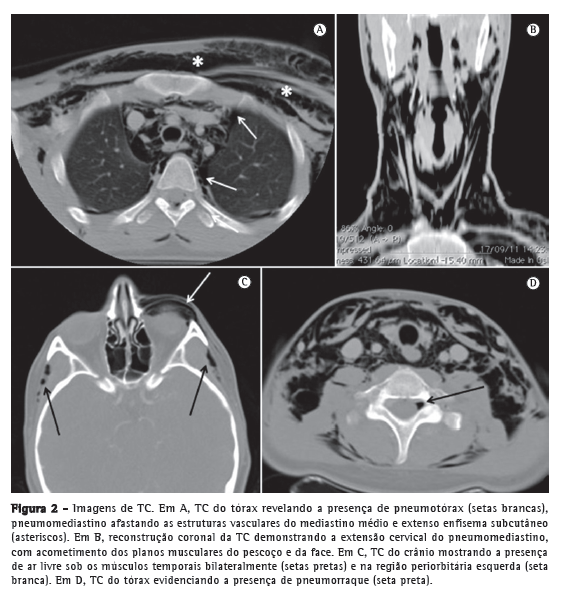
A TC de crânio, pescoço e tórax confirmou a presença de pneumomediastino, pneumotórax (Figura 2A), extenso enfisema de tecidos moles na região cervical (Figura 2B), incluindo face, tecidos periorbitários e músculos temporais (Figura 2C), além de documentar a presença de pneumorraque (Figura 2D).
A partir do segundo dia de internação, observou-se uma diminuição progressiva do enfisema subcutâneo. O tratamento instituído foi conservador, com repouso, dieta livre e analgesia, se necessário. Os exames laboratoriais de rotina, como hemograma e análise de urina, revelaram-se normais. Foram realizadas radiografias de tórax para o controle, observando-se uma redução diária dos achados acima descritos. A paciente permaneceu em observação por mais cinco dias, estando assintomática e com regressão quase completa do quadro clínico na alta hospitalar (Figura 1).
O pneumomediastino espontâneo ou síndrome de Hamman é definido pela presença de ar livre no mediastino, não sendo resultado de trauma, cirurgias ou outros procedimentos.(1) Constitui-se em uma entidade infrequente na prática médica,(1-6) tendo uma prevalência estimada entre 0,001% e 0,01%.(2) Em vista do seu curso quase sempre benigno, estima-se que uma série de diagnósticos seja perdida, porquanto muitos pacientes não procuram auxílio médico. Além disso, a detecção de uma causa não espontânea para o pneumomediastino, como cirurgias, traumas ou uso de ventilação mecânica, também diminui a sua prevalência.
Entre os fatores descritos como desencadeantes da doença, encontram-se exercícios físicos, trabalho de parto, cetoacidose diabética, inalação de drogas, tosse e vômitos.(3) O marco inicial da fisiopatologia da síndrome de Hamman é a ruptura alveolar, que resulta de uma alta pressão intra-alveolar, de uma baixa pressão perivascular, ou de ambas. Após o evento inicial, o ar penetra livremente no mediastino durante o ciclo respiratório, buscando equilibrar os gradientes pressóricos.(4) Esse mecanismo é conhecido como efeito ou fenômeno de Macklin, que descreveu detalhadamente esse cenário em 1939.(7)
Em dois terços dos casos, assim como no presente relato, pode haver progressão e acometimento da região cervical(5) e, menos frequentemente, dos tecidos faciais. O achado de pneumorraque, no entanto, é ainda mais raro, havendo apenas algumas descrições isoladas na literatura.(6) Acredita-se que, nessa situação, ocorra a passagem de ar pelos planos mediastinais posteriores, atingindo os neuroforames e o espaço epidural.(6) Se a passagem do ar para o mediastino e para os outros planos anatômicos anteriormente descritos não for suficiente para diminuir a pressão intra-alveolar, pode haver, como no presente caso e em 6-30% dos pacientes,(1) ruptura pleural com pneumotórax associado.(2) Outros locais passíveis de acometimento são o pericárdio e a cavidade peritoneal,(4) os quais, no presente caso, estavam preservados.
A maioria dos pacientes com síndrome de Hamman mostra-se sintomática em algum momento, sendo os sintomas mais frequentes a dispneia, a dor torácica e a tosse.(2) Em nosso caso, acreditamos que a tosse tenha sido o fator desencadeante, estando a paciente assintomática no restante do curso clínico da doença.
Algumas patologias vêm sendo associadas à síndrome de Hamman, como doenças intersticiais pulmonares, enfisema pulmonar, asma, bronquiectasias, malignidades intratorácicas e lesões císticas ou escavadas, assim como em pacientes após transplante pulmonar.(1,2) No caso descrito, a história clínica e a avaliação tomográfica da paciente conduziram-nos à exclusão de tais diagnósticos.
A radiografia do tórax costuma ser o primeiro exame realizado na triagem de pacientes com suspeita de pneumomediastino, seja ele espontâneo ou não. Para o pneumomediastino espontâneo, a sensibilidade do método mostra-se satisfatória, de aproximadamente 90%,(1) embora dependa sabidamente da extensão da afecção. No caso que apresentamos, a radiografia foi utilizada para o seguimento do caso, enquanto o diagnóstico foi determinado pela TC, considerada o padrão ouro na síndrome de Hamman.(3,5)
Embora se reconheça a importância dos estudos endoscópicos,(3) broncoscópicos e esofagográficos,(1) alguns autores recomendam suas realizações apenas na presença de disfagia, vômitos, traumas prévios, febre, leucocitose, derrame pleural, pneumoperitônio e doenças do aparelho digestivo,(4) achados ausentes no caso descrito. Além disso, tendo em vista a alta associação de enfisema cervical e odinofagia, esta última não é considerada como critério para a realização de exames invasivos.(4)
O tratamento da síndrome de Hamman ainda é controverso. A maioria dos estudos é limitada e sugere tratamento conservador, com repouso e analgesia, se necessário, apontando para a benignidade dessa condição.(2) No entanto, não existem consensos sobre o manejo desses pacientes.(4) Alguns centros têm recomendado restringir o uso de exames invasivos e de antimicrobianos, assim como evitar a restrição dietética, pois tais fatores aumentam o tempo médio de internação.(4) Além disso, a falta de familiaridade com essa entidade pode levar a estudos diagnósticos desnecessários e a tratamentos indevidos.(2)
As possíveis complicações variam de acordo com a etiologia ou o fator desencadeante. Em alguns casos, o atraso no diagnóstico e a não detecção de uma causa primária para o pneumomediastino podem levar, por exemplo, a ruptura esofágica, mediastinite ou pneumotórax hipertensivo.(1,4,5) A ocorrência de recidivas é rara, não sendo obrigatória a realização de seguimento a longo prazo.(2)
Giordano Rafael Tronco Alves
Acadêmico de Medicina,
Curso de Medicina da
Universidade Federal de Santa Maria, Santa Maria (RS) Brasil
Régis Vinícius de Andrade Silva
Médico Residente,
Serviço de Radiologia,
Hospital Universitário de Santa Maria, Curso de Medicina da
Universidade Federal de Santa Maria, Santa Maria (RS) Brasil
José Roberto Missel Corrêa
Médico Residente,
Serviço de Radiologia,
Hospital Universitário de Santa Maria, Curso de Medicina da
Universidade Federal de Santa Maria, Santa Maria (RS) Brasil
Cassiano Minussi Colpo
Médico Residente,
Serviço de Cirurgia,
Hospital Universitário de Santa Maria, Curso de Medicina da
Universidade Federal de Santa Maria, Santa Maria (RS) Brasil
Helen Minussi Cezimbra
Médica Residente,
Serviço de Infectologia,
Hospital Universitário de Santa Maria, Curso de Medicina da
Universidade Federal de Santa Maria, Santa Maria (RS) Brasil
Carlos Jesus Pereira Haygert
Professor Auxiliar da
Disciplina de Diagnóstico por Imagem, Universidade Federal de Santa Maria, Santa Maria (RS) BrasilReferências1. Iyer VN, Joshi AY, Ryu JH. Spontaneous pneumomediastinum: analysis of 62 consecutive adult patients. Mayo Clin Proc. 2009;84(5):417-21. PMid:19411438 PMCid:2676124.
2. Ho AS, Ahmed A, Huang JS, Menias CO, Bhalla S. Multidetector computed tomography of spontaneous versus secondary pneumomediastinum in 89 patients: can multidetector computed tomography be used to reliably distinguish between the 2 entities? J Thorac Imaging. 2012;27(2):85-92. PMid:21436744. http://dx.doi.org/10.1097/RTI.0b013e3182103876
3. Perna V, Vilà E, Guelbenzu JJ, Amat I. Pneumomediastinum: is this really a benign entity? When it can be considered as spontaneous? Our experience in 47 adult patients. Eur J Cardiothorac Surg. 2010;37(3):573-5. PMid:19748792. http://dx.doi.org/10.1016/j.ejcts.2009.08.002
4. Al-Mufarrej F, Badar J, Gharagozloo F, Tempesta B, Strother E, Margolis M. Spontaneous pneumomediastinum: diagnostic and therapeutic interventions. J Cardiothorac Surg. 2008;3:59. PMid:18980688 PMCid:2596119. http://dx.doi.org/10.1186/1749-8090-3-59
5. Conti-de-Freitas LC, Mano JB, Ricz HM, Mamede RC. A importância da suspeita clínica da síndrome de Hamman na sala de urgência. Rev Bras Cir Cabeça Pescoço. 2009;38(2):122-3.
6. Song Y, Tu L, Wu J. Pneumorrhachis with spontaneous pneumomediastinum and subcutaneous emphysema. Intern Med. 2009;48(18):1713-4. PMid:19755782. http://dx.doi.org/10.2169/internalmedicine.48.2256
7. Macklin CC. Transport of air along sheaths of pulmonic blood vessels from alveoli to mediastinum. Arch Intern Med. 1939;64(5):913-26. http://dx.doi.org/10.1001/archinte.1939.00190050019003



