ABSTRACT
Pancoast syndrome consists of signs and symptoms resulting from a tumor affecting the pulmonary apex and adjacent structures. The process is typically caused by a neoplasm. The majority of cases of Pancoast syndrome are caused by bronchogenic carcinoma. The most commonly found histologic subtypes are adenocarcinoma and epidermoid carcinoma. There have been very few reports of small cell lung carcinoma in the genesis of Pancoast syndrome. We describe the case of a patient with Pancoast syndrome caused by small cell lung carcinoma and discuss the aspects related to the diagnosis and treatment.
Keywords:
Pancoast syndrome; Small cell lung carcinoma; Lung neoplasms.
RESUMO
A síndrome de Pancoast consiste de sinais e sintomas decorrentes do acometimento do ápice pulmonar e estruturas adjacentes por um tumor. Na maioria das vezes, o processo causal é uma neoplasia. O carcinoma broncogênico é a principal neoplasia causadora da síndrome. Os subtipos histológicos mais encontrados são o adenocarcinoma e o carcinoma epidermoide. A ocorrência de carcinoma de pequenas células de pulmão como gênese da síndrome de Pancoast é rara, com poucos relatos na literatura. Descrevemos o caso de um doente com síndrome de Pancoast causado por um carcinoma de pequenas células de pulmão, discutindo aspectos referentes ao diagnóstico e à terapêutica.
Palavras-chave:
Síndrome de Pancoast; Carcinoma de pequenas células; Neoplasias pulmonares.
IntroductionPancoast syndrome is defined as a set of signs and symptoms secondary to the neoplastic impairment of the brachial plexus, parietal pleura, first/second ribs (and adjacent vertebral bodies), first/second thoracic nerves, paravertebral sympathetic chain and stellate ganglion, due to a tumor in the superior sulcus, also known as a Pancoast tumor. Clinically, the symptoms are pain in the shoulder and dorsal face of the ipsilateral affected arm and hypesthesia of the elbow/forearm, evolving to weakness and muscle hypotrophy, including atrophy of the ring finger and little finger. Horner's syndrome, which involves stellate ganglion impairment, clinically manifesting as palpebral myosis/ptosis, enophthalmos and anhidrosis, can be included in the spectrum of Pancoast syndrome features.(1) Most patients with Pancoast tumors have non-small cell bronchogenic carcinoma, most often epidermoid carcinoma or adenocarcinoma.(2)
Less common causes of superior sulcus tumors, such as other primary malignant neoplasias of the chest, metastatic malignant diseases and benign pathologies, have been described.(3-6) However, Pancoast syndrome involving small cell lung carcinoma is rare.(1)
Here, we present the case of a patient with Pancoast syndrome caused by small cell lung carcinoma.
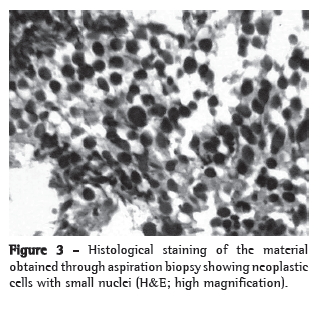
Case reportWe report a case of a 74-year-old hypertensive white male, a painter, with peripheral vascular insufficiency of the lower limbs. The patient had been a smoker for 54 years (one pack of cigarettes per day). He presented with a two-month history of sharp, right-sided pleuritic pain, accompanied by productive cough with watery expectoration, as well as by dyspnea upon exertion. Physical examination at admission showed only universal reduction in breath sounds, and reduced dorsalis pedis pulse rate, without neurological deficits. No alterations were observed in the results of the blood workup, biochemical blood tests or urinalysis. His PPD was nonreactor and testing for acid-fast bacilli in sputum was negative. Chest imaging tests (Figures 1 and 2) showed a mass with regular borders in the right superior sulcus, affecting the adjacent vertebrae and ribs. Whole-body gallium scintigraphy and CT of the skull were normal. The patient was submitted to thoracic punch biopsy, the histopathological study of which showed small cell lung carcinoma (Figure 3). During his hospital stay, the patient evolved to paresthesia in the right axilla region and worsening of the chest pain, which became intense over the right scapula.

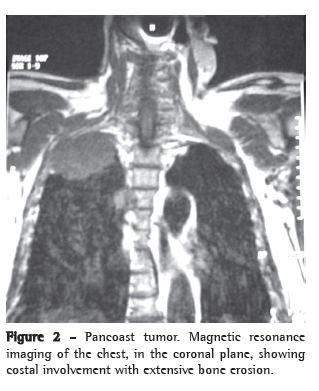
Despite the fact that the patient presented locally advanced disease, due to the comorbidities, he was submitted only to radiotherapy in a single dose of 50 Gy. After two weeks of radiotherapy, the patient presented complete remission of the neurological signs and symptoms. He was then discharged from the hospital. He was referred for palliative treatment. Six months after discharge from the hospital, the disease progressed, evolving to death one month later.
DiscussionAlthough most Pancoast tumors are caused by bronchogenic carcinoma, they are concomitant with superior sulcus tumors in only 5% of cases.(1) Due to its biological characteristics, small cell lung carcinoma has rarely been reported as a cause of Pancoast tumors.(1,2,7) Only 4.5% of small cell carcinomas manifest as superior sulcus tumors, and slightly more than 1% manifest as Horner's syndrome.(7)
In the case reported here, the patient presented symptoms typical of Pancoast syndrome, with involvement of the brachial plexus, together with costal and vertebral erosion, although without Horner's syndrome.(8) The diagnosis of these types of tumors can sometimes be delayed, since there is often diagnostic confusion with painful shoulder syndrome.(8) In our patient, the time between symptom onset and diagnosis was relatively short. However, other factors were determinant to the disease outcome, as explained below.
The pulmonary mass was investigated using CT and magnetic resonance imaging of the chest. Even with the advances in CT imaging acquisition techniques, with better detection and evaluation of the tumor growth, as well as of the extent of infiltration into the chest wall and mediastinal involvement,(9) magnetic resonance imaging of the chest is still the best means of evaluating superior sulcus tumors.(10-12) Although magnetic resonance imaging of the chest provides the same information that CT does, it allows better evaluation of the central nervous system impairment.(10)
Biopsy via bronchoscopy has a low yield due to the anatomical location of the tumor mass.(2) The diagnostic procedure of choice for material acquisition is image-guided transthoracic needle aspiration biopsy, which has low complication rates.(1,2,8) When it is not possible to obtain material through aspiration biopsy, video-assisted thoracoscopy, which also provides more information on staging, should be used.(8) We performed biopsy and aspiration of the lesion, both of which provided samples that were characterized as small cell lung carcinoma in the histopathological examination. Due to the rarity of small cell lung carcinoma in such cases, the specimens were reviewed, including the use of specific stains for small cell tumors (Figure 3) before delivering the final result. Histological diagnosis is currently imperative prior to the initiation of treatment, and emergency radiotherapy is reserved for the treatment of exceptional cases in which no diagnosis has been made.(12,13)
The standard treatment for small cell lung carcinoma is chemotherapy, based on the combination of a platin analog and irinotecan, with or without local radiotherapy.(12,13) In cases of better prognosis, the combination of chemotherapy and radiotherapy, the latter administered approximately 30 days after the initiation of the former, would be indicated.(14) The use of radiotherapy alone is effective, with a good rate of symptom relief, especially in apical tumors.(15) Due to the comorbidities presented by our patient, local isolated radiotherapy was first administered, and there was a good response in terms of the neurological symptoms. Small cell lung carcinoma is a rapid-progression neoplasia, the mean survival after diagnosis being two to four months in untreated patients.(14) In the case presented here, the disease progressed and the patient died seven months after discharge from the hospital, which is consistent with this kind of neoplasia.(7) Chemotherapy should be considered even in elderly patients with poor prognosis or significant comorbidities.(12) Submitting our patient to the standard treatment (chemotherapy) might have increased survival.
In summary, we have presented the case of a patient with a Pancoast tumor, Pancoast syndrome (without Horner's syndrome) and a histopathological diagnosis of small cell lung carcinoma. Although rare, small cell lung carcinoma should always be considered in the differential diagnosis of superior sulcus tumors.
References 1. Arcasoy SM, Jett JR. Superior pulmonary sulcus tumors and Pancoast's syndrome. N Engl J Med. 1997;337(19):1370-6.
2. Archie VC, Thomas CR Jr. Superior sulcus tumors: a mini-review. Oncologist. 2004;9(5):550-5.
3. Doganova A, Moreira AL, Bona M, Moreira JS. Síndrome de Pancoast causada por linfoma. J Pneumol. 2000;26(3):145-8.
4. Montero C, Deben G, de la Torre M, Alvarez A, Verea H. Pancoast syndrome and endobronchial tumor infiltration as the first manifestation of lymphoma [Article in Spanish]. Arch Bronconeumol. 2004;40(6):287-9.
5. Fibla JJ, Penagos JC, Leon C. Pseudo-pancoast syndrome caused by a solitary fibrous tumor of the pleura [Article in Spanish]. Arch Bronconeumol. 2004;40(5):244-5.
6. Silverman MS, MacLeod JP. Pancoast's syndrome due to staphylococcal pneumonia. CMAJ. 1990;142(4):343-5.
7. Johnson DH, Hainsworth JD, Greco FA. Pancoast's syndrome and small cell lung cancer. Chest. 1982;82(1):602-6.
8. Khosravi Shahi P. Pancoast's syndrome (superior pulmonary sulcus tumor): review of the literature [Article in Spanish]. An Med Interna. 2005;22(4):194-6.
9. Chaefer-Prokop C, Prokop M. New imaging techniques in the treatment guidelines for lung cancer. Eur Respir J Suppl. 2002;35:S71-S83.
10. Heelan RT, Demas BE, Caravelli JF, Martini N, Bains MS, McCormack PM, et al. Superior sulcus tumors: CT and MR imaging. Radiology. 1989;170(3 Pt 1):637-41.
11. Peces-Barba G. New applications of magnetic resonance imaging for the thorax [Article in Spanish]. Arch Bronconeumol. 2002;38(10):461-2.
12. Alberts WM; American College of Chest Physicians. Diagnosis and management of lung cancer executive summary: ACCP evidence-based clinical practice guidelines (2nd Edition). Chest. 2007;132(3 Suppl):S1-S19.
13. Shahian DM. Contemporary management of superior pulmonary sulcus (Pancoast) lung tumors. Curr Opin Pulm Med. 2003;9(4):327-31.
14. De Ruysscher D, Pijls-Johannesma M, Vansteenkiste J, Kester A, Rutten I, Lambin P. Systematic review and meta-analysis of randomised, controlled trials of the timing of chest radiotherapy in patients with limited-stage, small-cell lung cancer. Ann Oncol. 2006;17(4):543-52.
15. Komaki R, Roh J, Cox JD, Lopes da Conceicao A. Superior sulcus tumors: results of irradiation of 36 patients. Cancer. 1981;48(7):1563-8.
About the authors
Jefferson Fontinele e Silva
Resident in Pulmonology. Hospital de Base of the Federal District of Brasília, Brasília, Brazil.
Melânio de Paula Barbosa
Preceptor for the Department of Pulmonology. Hospital de Base of the Federal District of Brasília, Brasília, Brazil.
Cláudio Luiz Viegas
Preceptor for the Department of Pulmonology. Hospital de Base of the Federal District of Brasília, Brasília, Brazil.
Study carried out at the Hospital de Base of the Federal District of Brasília, Brasília, Brazil.
Correspondence to: Jefferson Fontinele e Silva. Quadra 2, Conjunto C15, Bloco C, apto. 103, Edifício Santa Clara, CEP 73015-315, Sobradinho, DF, Brasil.
Tel 55 61 3325-4818. E-mail: jefejane@hotmail.com
Financial support: None.
Submitted: 6 February 2008. Approved, after review: 20 June 2008.




