ABSTRACT
Objective: To investigate the incidence of asthma symptoms in young amateur swimmers, and to describe the clinical treatment of the children with asthma in a private sports club in the city of São Paulo, Brazil. Methods: The study included 171 amateur swimmers, ranging from 6 to14 years of age. All of the participants or their legal guardians were asked to complete the International Study of Asthma and Allergies in Childhood (ISAAC) questionnaire, and 119 were submitted to pulmonary function testing at rest. Results: The overall incidence of asthma symptoms (ISAAC score ≥ 6) among the swimmers was 16.8%. Of the 119 swimmers submitted to spirometry, 39 (32.7%) presented spirometric alterations (FEV1/FVC < 0.75). Among those with an ISAAC score ≥ 6, there were 10 (31.2%) who stated that they were receiving no asthma treatment. Of those who reported receiving pharmacological treatment, 24% made use of bronchodilators but not of corticosteroids. Conclusions: The incidence of asthma symptoms and pulmonary function alterations among amateur swimmers within the 6-14 age bracket was high. In addition, a relevant proportion of these athletes were receiving no treatment.
Keywords:
Asthma/therapy; Asthma/diagnosis; Child; Swimming; Exercise.
RESUMO
Objetivo: Investigar a frequência de sintomas de asma entre crianças e adolescentes nadadores amadores e descrever o tratamento clínico entre as crianças asmáticas em um clube esportivo privado na cidade de São Paulo. Métodos: Foram incluídos no estudo 171 nadadores amadores de 6 a 14 anos de idade. Todos os participantes ou seus responsáveis foram solicitados a responder o questionário International Study of Asthma and Allergies in Childhood (ISAAC), e 119 realizaram prova de função pulmonar em repouso. Resultados: A frequência geral de sintomas de asma (ISAAC ≥ 6 pontos) entre os nadadores foi de 16,8%. Entre os 119 nadadores que realizaram a espirometria, 39 (32,7%) apresentaram alterações espirométricas (VEF1/CVF < 0,75). Entre os sujeitos com escore ISAAC ≥ 6, 10 (31,2%) alegaram não realizar nenhum tipo de tratamento para a doença. Daqueles que afirmaram realizar tratamento medicamentoso, 24% faziam uso de broncodilatadores mas não de corticosteroides. Conclusões: A frequência de sintomas de asma e de alterações da função pulmonar em nadadores amadores de 6 a 14 anos foi elevada. Além disso, uma proporção considerável destes atletas não recebia tratamento.
Palavras-chave:
Asma/terapia; Asma/diagnóstico; Criança; Natação; Exercício.
IntroductionAmong chronic diseases worldwide, asthma is responsible for the greatest morbidity and mortality among children and adolescents. There is evidence that its prevalence has been increasing over the last 20 years.(1,2) In the city of São Paulo, the prevalence of asthma symptoms ranges from 6.1% to 10%, respectively, in children between 6 and 7 years of age and in adolescents between 13 and 14 years of age.(3) The management of asthma aims to reduce and control respiratory symptoms, to prevent/reduce crises, to maintain pulmonary function as close as possible to within the normal range, to minimize adverse effects of medication and to maintain normality in the performance of activities of daily living, including the practice of aerobic physical exercise.(1)
In asthma patients, pulmonary function and physical capacity respond to physical exercise in an ambiguous manner. Although exertion can result in exercise-induced bronchospasm (EIB),(4) it can also lead to an improvement in physical conditioning and to a reduction in dyspnea when practiced regularly and appropriately.(5,6) The EIB is aggravated when physical activity is performed in a dry, cold environment, and the symptoms resulting from these activities can often prevent the asthma patient from practicing sports or physical activities in groups.(7) Swimming has traditionally been recommended as the most appropriate physical activity for asthma patients, probably due to the warm, humid environment. However, the best modality of aerobic physical activity for individuals with asthma has yet to be defined.(8)
The procedure most commonly used for disinfection of the water in swimming pools is treatment with chlorine-based products. These are concentrated on the surface of the water(9) and can also cause undesirable effects on the respiratory system, as has been shown in studies involving elite swimmers.(10) There is evidence that these swimmers present a higher prevalence of bronchial hyperresponsiveness when compared to athletes participating in other sports.(11) In addition, various reports suggest that chronic exposure to chlorine increases the incidence of laryngeal edema, nasopharyngeal irritation and transitory lacrimation.(10) Although a number of studies have evaluated the incidence of asthma symptoms in elite swimmers,(12) few have done so in amateur swimmers.(12)
The present study aimed to investigate the incidence of asthma symptoms among amateur swimmers from 6 to 14 years of age and to describe the clinical treatment given to those with asthma.
MethodsA total of 171 amateur swimmers were evaluated, all within the 6-14 age bracket and belonging to the upper middle class. The study was conducted at a private club in the city of São Paulo, Brazil, where the disinfection of the swimming pools was carried out with chlorine-based compounds. The swimmers and the parents or legal guardians were asked to complete a questionnaire to evaluate the incidence of asthma symptoms, and the children were submitted to spirometry at rest. All of the patients and legal guardians were informed of the objectives of the study, and the athletes were included only after written informed consent had been obtained, in accordance with the national legislation. The study design was approved by the Ethics Committee of the São Luiz Hospital (Protocol no. 114/2006).
QuestionnaireThe International Study of Asthma and Allergies in Childhood (ISAAC) questionnaire, validated for the Portuguese language,(13) was used for evaluating the asthma symptoms. In this interpretation, the sum of symptoms is quantified through the use of a scale in which values range from 0 to 14 points. The incidence of asthma symptoms was determined by the cut-off point of the total score, which was set at a score of 6.(13,14) The swimmers between 13 and 14 years of age completed the questionnaire by themselves, whereas the questionnaires of the children between 6 and 7 years were completed by their parents or guardians, as previously described.(15) A number of questions were also added to the questionnaire. These aimed to evaluate the factors that led the child to start the swimming practice, as well as to investigate which medication was used by the children who had previously been diagnosed with asthma or rhinitis. Questionnaires with incomplete data were excluded, as were those containing more than one answer to any given question.
Pulmonary function testsSpirometry was conducted using a manual spirometer (model One Flow Tester Screen; Clement Clarke Int., Harlow, UK), and the highest value obtained in three forced expiratory maneuvers was selected, in accordance with the acceptance and reproducibility criteria of the American Thoracic Society/European Respiratory Society.(16) The selection of PEF, FEV1 and FVC values followed the same recommendations. For this study, a value of 0.75 was defined as the lower limit of normality for the FEV1/FVC ratio.
Statistical analysisThe data are expressed as percentages. Spirometric variables and the incidence of asthma symptoms obtained through the ISAAC questionnaire were compared using the chi-square test.
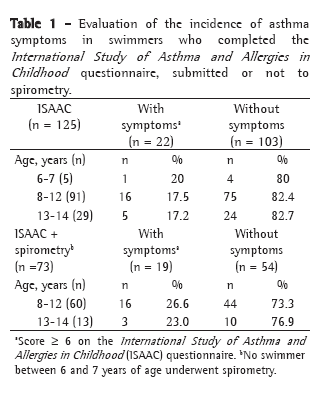
ResultsOf the 171 amateur swimmers who agreed to participate in the study, 125 completed the ISAAC questionnaire and 119 underwent pulmonary function tests. A total of 73 swimmers were submitted to both evaluations. The mean age was 11 ± 1.8 years and 50.3% were female. None of the swimmers between 6 and 7 years of age were submitted to spirometry. The incidence of asthma symptoms among swimmers of all ages was 16.8% (21/125), and the rate of their occurrence was similar in all of the age brackets evaluated (ranging from 17.2% to 20%; Table 1). Among the children between 6 and 7 years of age who had been diagnosed with asthma before taking up the sport of swimming, the incidence of asthma symptoms was 26% (19/73). These values were similar to those observed in the other age brackets (23% and 26.6% in the 8-12 and 13-14 age brackets, respectively).
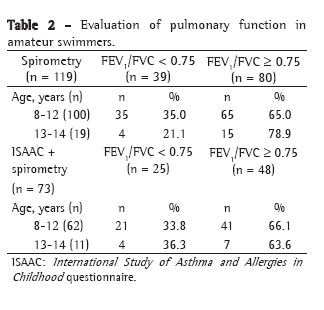
Of the 119 swimmers submitted to spirometry, 39 (32.7%) presented a reduction in the FEV1/FVC ratio. The incidence of the reduction in the pulmonary function was lower in the 13-14 age bracket than in the 8-12 age bracket (21% and 35%, respectively; Table 2). When analyzed among the 73 swimmers who were submitted to spirometry and who completed the ISAAC questionnaire, airway obstruction (FEV1/FVC < 0.75) was similar, regardless of age (33.8% and 36.3%, respectively, in the 8-12 and the 13-14 age brackets).
When evaluating the concordance between the incidence of asthma symptoms and the reduction in pulmonary function among the swimmers, we observed that the incidence of a reduction in the FEV1/FVC ratio was higher than was that of asthma symptoms (34.2% vs. 15%; p < 0.01; Table 3). Although the incidence of a reduction in pulmonary function was higher among swimmers who had previously been diagnosed with asthma, there was no significant difference in comparison with swimmers without asthma (47% vs. 29.6%; p = 0.29). There was no concordance between the alterations in pulmonary function and the incidence of asthma symptoms in swimmers with or without asthma (p < 0.01; Table 3).

When asked about their reasons for choosing swimming, 112 (89.6%) of the 125 participants who completed the questionnaire reported the preference for the sports modality, whereas 6 (4.8%) cited the love of competition, 5 (4.0%) stated that they were motivated by the presence of respiratory problems, and 2 (1.6%) cited the need to correct orthopedic or postural problems.
In the same group of participants, 32 (25.6%) reported having been diagnosed with asthma or bronchitis and 73 (58.4%) reported having a relative with asthma. In answering the question related to the pharmacological treatment for asthma, 10 swimmers (31.2%) reported not being submitted to any type of treatment, whereas 22 (68.7%) described various treatments. The treatment was categorized according to the modalities most frequently reported: homeopathy or naturopathy only (in 13%); antibiotic therapy, with or without another treatment modality (in 9%); bronchodilator, with or without another treatment modality, excluding the use of corticosteroids (in 24%); and the combination of a corticosteroid and bronchodilator (in 16%).
DiscussionThe present study shows that the incidence of asthma symptoms among amateur swimmers is higher than that observed in the general population of Brazil, and that the incidence of spirometric alterations is higher still. These results suggest discordance between the reported incidence of asthma symptoms and the spirometric evaluations in this population. The percentage of children diagnosed with asthma is high among those practicing swimming. However, only a few are receiving clinical and pharmacological treatment as recommended by the national and international consensuses.
Swimming is considered the ideal physical activity for individuals with asthma, probably due to the high humidity of the inhaled air, which helps prevent and reduce EIB.(17) The benefits of swimming for individuals with asthma are reinforced by studies that suggest a reduction in the symptoms,(18) improved endurance(19) and reduction in EIB intensity.(20) However, there are reports showing that the disinfection of the pools with chlorine-based products can cause airway irritation and alterations,(20-22) which are well-established in elite swimmers but unknown in amateur swimmers. These alterations have been thought to be associated with the intensity of the training and chronic exposure to chlorine.
Our results show an incidence of asthma symptoms of approximately 20% among amateur swimmers, regardless of the age bracket evaluated and, therefore, higher than those described in children who do not practice sports in the southern region of Brazil (4.9-10.2%).(23) There are two hypotheses for this high incidence of asthma symptoms among amateur swimmers: that a greater number of children with asthma seek swimming on the advice of their physicians; and that exposure to the irritants contained in chlorine-based products provokes asthma symptoms.
Both hypotheses seem to be involved in the high incidence of asthma symptoms among amateur swimmers, since the number of children having been previously diagnosed with asthma was high (23-26%). This incidence of symptoms was comparable between the group of swimmers having been previously diagnosed with asthma and those not having been so diagnosed (Table 1). Our results suggest that, for children with asthma, swimming in pools in which the water is disinfected with chlorine-based products is not a physical activity that reduces the levels of symptoms. In addition, the practice of these sports in such pools seem to increase the incidence of asthma symptoms in amateur swimmers without asthma to a degree similar to that found in swimmers with asthma.
A recent systematic review suggested that physical activity, when performed at the appropriate intensity and for an adequate duration, can improve physical capacity, as well as reducing dyspnea, in asthma patients.(5) Although swimming is considered an ideal modality for individuals with asthma, there are reports suggesting that elite swimmers have shown a high incidence of bronchial hyperresponsiveness and asthma symptoms, as well as a high number of eosinophils and neutrophils in induced sputum, when compared with athletes in other endurance sports,(11) suggesting that the chronic exposure to chlorine derivatives induces airway inflammation. (24) The higher incidence of asthma among amateur swimmers not previously diagnosed with asthma reinforces the hypothesis that the type of sport can truly be an essential factor in the development of asthma symptoms. Curiously, counter to the idea that individuals with asthma tend to choose swimming precisely because of their respiratory problem,(9) most of the subjects interviewed in the present study reported that the choice was based exclusively on personal preference for the sport. Only 4.8% of the participants stated that they chose swimming due to respiratory problems.
In recent decades, the prevalence of asthma symptoms in children and teenagers has shown a progressive increase in several countries.(2) The social and economic consequences of the disease are significant, since they impair the quality of life of individuals with asthma, making asthma a public health problem.(25) Spirometry is the gold standard for the evaluation of pulmonary function.(13) However, due to limitations related to cost, time and trained staff, the ISAAC questionnaire was developed for use in epidemiological studies aimed at determining the incidence of asthma and allergic diseases.(26) The ISAAC questionnaire is considered to be easily understood, self-applicable and not dependent on the presence of an interviewer,(12) having been evaluated for children between 6 and 7 years of age and adolescents between 13 and 14 years of age.(25) In the present study the ISAAC questionnaire was also applied in children between 8 and 12 years of age and produced results similar to those found in the age brackets for which the questionnaire is validated. It is of interest that 30.1% of the swimmers who underwent spirometry and completed the questionnaire presented a negative incidence of asthma symptoms but showed signs of airway obstruction.
Since the swimmers evaluated in the present study swam in a pool in which the water treatment was chlorine-based, our findings cannot be extrapolated to swimmers who practice their sport in pools in which other types of water treatment are employed.
In cases of asthma, the determination of its severity is important for devising an appropriate plan for its management. Corticosteroids, especially those administered through inhalation and in combination with β2 agonists, are the most effective pharmacological therapy for asthma.(1)
In the present study, only 16% of the athletes who reported having physician-diagnosed asthma were making use of the pharmacological therapy suggested by the medical consensuses. In addition, 8% of the athletes previously diagnosed with asthma reported not being under any kind of treatment, and more than 20% of the swimmers were receiving clinical treatment other than that recommended by the national and international consensuses for the treatment of asthma.(1)
The methods used for identifying pulmonary alterations in the amateur swimmers do not constitute the standard for the diagnosis of asthma in isolation, making physician evaluation indispensible in this case. Although the ISAAC protocol is validated for use in Brazil and is useful in epidemiological studies, it is not sufficient for making a diagnosis of asthma. Furthermore, spirometry at rest is considered nonspecific for the diagnosis of asthma, and bronchodilator testing is the best means of measuring bronchial responsiveness. In the present study, bronchodilator testing was not performed due to reluctance on the part of the parents and legal guardians to allow the use of medication during the spirometry.
Our results show that the incidence of asthma symptoms and the alterations in pulmonary function in young amateur swimmers who practice the sport in pools with chlorine-based water treatment was higher than that observed in the general population. In addition, most swimmers with asthma were receiving clinical or pharmacological treatment other than that recommended based on the established clinical criteria. These results suggest the need for better clinical monitoring of amateur swimmers in order to identify respiratory alterations.
References 1. Bateman ED, Hurd SS, Barnes PJ, Bousquet J, Drazen JM, FitzGerald M, et al. Global strategy for asthma management and prevention: GINA executive summary. Eur Respir J. 2008;31(1):143-78.
2. Burr ML, Butland BK, King S, Vaughan-Williams E. Changes in asthma prevalence: two surveys 15 years apart. Arch Dis Child. 1989;64(10):1452-6.
3. Solé D, Camelo-Nunes IC, Wandalsen GF, Pastorino AC, Jacob CM, Gonzalez C, et al. Prevalence of symptoms of asthma, rhinitis, and atopic eczema in Brazilian adolescents related to exposure to gaseous air pollutants and socioeconomic status. J Investig Allergol Clin Immunol. 2007;17(1):6-13.
4. Orestein DM. Asthma and sports. In: Bar-Or O, editor. The child and the adolescent athlete. London: Wiley-Blackwell; 1996. p. 433-54.
5. Ram FS, Robinson SM, Black PN, Picot J. Physical training for asthma. Cochrane Database Syst Rev. 2005;(4):CD001116.
6. Disabella V, Sherman C, DiNubile NA. Exercise for Asthma Patients: Little Risk, Big Rewards. Physician Sports Med. 1998;26(6):75-85.
7. Matsumoto I, Araki H, Tsuda K, Odajima H, Nishima S, Higaki Y, et al. Effects of swimming training on aerobic capacity and exercise induced bronchoconstriction in children with bronchial asthma. Thorax. 1999;54(3):196-201.
8. Helenius I, Haahtela T. Allergy and asthma in elite summer sport athletes. J Allergy Clin Immunol. 2000;106(3):444-52.
9. Nemery B, Hoet PH, Nowak D. Indoor swimming pools, water chlorination and respiratory health. Eur Respir J. 2002;19(5):790-3.
10. Zwick H, Popp W, Budik G, Wanke T, Rauscher H. Increased sensitization to aeroallergens in competitive swimmers. Lung. 1990;168(2):111-5.
11. Helenius IJ, Tikkanen HO, Sarna S, Haahtela T. Asthma and increased bronchial responsiveness in elite athletes: atopy and sport event as risk factors. J Allergy Clin Immunol. 1998;101(5):646-52.
12. Solé D, Vanna AT, Yamada E, Rizzo MC, Naspitz CK. International Study of Asthma and Allergies in Childhood (ISAAC) written questionnaire: validation of the asthma component among Brazilian children. J Investig Allergol Clin Immunol. 1998;8(6):376-82.
13. Solé D. The International Study of Asthma and Allergies in Childhood (ISAAC): what have we learned? J Bras Pneumol. 2005;31(2):93-5.
14. Boechat JL, Rios LJ, Sant´anna CC, França AT. Prevalence and severity of asthma symptoms in school-age children in the city of Duque de Caxias, Rio de Janeiro, Brazil. J Bras Pneumol. 2005;31(2):111-7.
15. Miller MR, Hankinson J, Brusasco V, Burgos F, Casaburi R, Coates A, et al. Standardisation of spirometry. Eur Respir J. 2005;26(2):319-38.
16. Bar-Or O, Inbar O. Swimming and asthma. Benefits and deleterious effects. Sports Med. 1992;14(6):397-405.
17. Fitch KD, Morton AR, Blanksby BA. Effects of swimming training on children with asthma. Arch Dis Child. 1976;51(3):190-4.
18. Svenonius E, Kautto R, Arborelius M Jr. Improvement after training of children with exercise-induced asthma. Acta Paediatr Scand. 1983;72(1):23-30.
19. Drobnic F, Freixa A, Casan P, Sanchis J, Guardino X. Assessment of chlorine exposure in swimmers during training. Med Sci Sports Exerc. 1996;28(2):271-4.
20. Nemery B, Hoet PH, Nowak D. Indoor swimming pools, water chlorination and respiratory health. Eur Respir J. 2002;19(5):790-3.
21. Potts J. Factors associated with respiratory problems in swimmers. Sports Med. 1996;21(4):256-61.
22. Chatkin MN, Menezes AM. Prevalence and risk factors for asthma in schoolchildren in southern Brazil. J Pediatr (Rio J.). 2005;81(5):411-6.
23. Bonsignore MR, Morici G, Riccobono L, Profita M, Bonanno A, Paternò A, et al. Airway cells after swimming outdoors or in the sea in nonasthmatic athletes. Med Sci Sports Exerc. 2003;35(7):1146-52.
24. Fanelli A, Cabral AL, Neder JA, Martins MA, Carvalho CR. Exercise training on disease control and quality of life in asthmatic children. Med Sci Sports Exerc. 2007;39(9):1474-80.
25. Thickett KM, McCoach JS, Gerber JM, Sadhra S, Burge PS. Occupational asthma caused by chloramines in indoor swimming-pool air. Eur Respir J. 2002;19(5):827-32.
26. Amorim AJ, Daneluzzi JC. Prevalence of asthma in schoolchildren [Article in Portuguese]. J Pediatr (Rio J). 2001;77(3):197-202.
Study carried out at the São Luiz Hospital, São Paulo, Brazil, and the ABC School of Medicine, Santo André, Brazil.
Correspondence to: Iara Nely Fiks. Rua Dr. João Clímaco Pereira, 51, Itaim Bibi, CEP 04532-070, São Paulo, Brazil.
Tel 55 11 3845-3800. E-mail: ifiks@uol.com.br
Financial support: None.
Submitted: 20 February 2008. Accepted, after review: 5 September 2008.
About the authorsIara Nely Fiks
Professor of Pulmonology. ABC School of Medicine, Santo André, Brazil.
Leonardo Carlos Araujo Santos
Physical Therapist. São Luiz Hospital, São Paulo, Brazil.
Telma Antunes
Pulmonologist. Department of Cardiorespiratory Diseases. The Heart Institute of the Faculdade de Medicina da Universidade de São Paulo - FMUSP, University of São Paulo School of Medicine - São Paulo, Brazil.
Raquel Calvo Gonçalves
Physical Therapist. Department of Physical Therapy, Faculdade de Medicina da Universidade de São Paulo - FMUSP, University of São Paulo School of Medicine - São Paulo, Brazil.
Celso Ricardo Fernandes de Carvalho
Tenured Associate Professor. Department of Physical Therapy, Speech Therapy and Occupational Therapy, Faculdade de Medicina da Universidade de São Paulo - FMUSP, University of São Paulo School of Medicine - São Paulo, Brazil.
Carlos Roberto Ribeiro Carvalho
Tenured Associate Professor. Department of Cardiorespiratory Diseases. The Heart Institute of the Faculdade de Medicina da Universidade de São Paulo - FMUSP, University of São Paulo School of Medicine - São Paulo, Brazil.






