ABSTRACT
Objective: To analyze the characteristics of patients with lung cancer. Methods: A retrospective descriptive study of patients receiving a histopathological diagnosis of lung cancer between 1995 and 2002 in the city of Manaus, Brazil. Data were collected from the medical archives of three hospitals. Statistical analyses were carried out, and survival curves were generated by means of an actuarial estimator. Results: Of the 352 patients selected, 262 (74.4%) were male and 90 (25.6%) were female. The mean age was 62 years. The following histological types were identified: squamous cell carcinoma, 62.8%; adenocarcinoma, 24.7%; small cell carcinoma, 9.1%; and large cell carcinoma, 3.4%. The most common stages were stages IIIB and IV, in 45% and 21.5%, respectively. Of the total sample, 73.4% were submitted to treatment. Of these, 51.4% underwent radiotherapy; 16.6%, surgery; 15.8%, chemotherapy; and 16.2%, radiotherapy in association with chemotherapy. Cumulative survival rates were low: three-year survival was 6.5%, and five-year survival was 3.5%. Conclusions: In this group of patients with lung cancer, survival rates were considerably lower than those reported in the literature. This might be attributable to the limited access to the specialized health care system and the advanced stage of the disease at diagnosis.
Keywords:
Lung neoplasms; Neoplasm staging; Survival.
RESUMO
Objetivo: Analisar as características de pacientes com câncer de pulmão. Métodos: Estudo retrospectivo e descritivo
dos pacientes com diagnóstico histopatológico de câncer de pulmão entre 1995 e 2002 em Manaus (AM). Os dados dos pacientes foram coletados nos arquivos médicos de três hospitais. As análises estatísticas foram realizadas,
e as curvas de sobrevida geradas a partir do estimador atuarial. Resultados: Dos 352 pacientes selecionados, 262 (74,4%) eram do sexo masculino e 90 (25,6%) do feminino. A média de idade foi de 62 anos. Os seguintes tipos histológicos foram encontrados: carcinoma de células escamosas, 62,8%; adenocarcinoma, 24,7%; carcinoma de pequenas células, 9,1%; e carcinoma de grandes células, 3,4%. Os estádios IIIB e IV foram os mais comuns, com uma frequência de 45% e 21,5%, respectivamente. Da amostra total, 73,4% foram submetidos a tratamento. Desses, 51,4% foram submetidos à radioterapia; 16,6%, à cirurgia; 15,8%, à quimioterapia; e 16,2%, à radioterapia associada à quimioterapia. Os níveis de sobrevida acumulada foram baixos: a sobrevida em três anos foi de 6,5% e a sobrevida em cinco anos foi de 3,5%. Conclusões: Este grupo de pacientes com câncer de pulmão apresentou uma sobrevida muito pequena, divergindo dos resultados encontrados na literatura. Isto é provavelmente decorrente
da dificuldade de acesso ao sistema de saúde especializado e do estágio avançado do diagnóstico.
Palavras-chave:
Neoplasias pulmonares; Estadiamento de neoplasias; Sobrevivência.
IntroductionWorldwide, lung cancer is one of the most common types of neoplasia and surpasses all others in terms of mortality rates.(1,2) The annual increase in the incidence of lung cancer is 2%, corresponding to 1.2 million new cases annually.(3) In Brazil, lung cancer is the second most common type of cancer among men and the fourth among women. The National Cancer Institute estimates that there were 27,270 new cases nationwide in 2008, 630 occurring in the state of Amazonas (360 in the state capital of Manaus alone). Of those, 61.7% will have occurred in males and 38.2% will have occurred in females, showing that this type of cancer affects men more often than women, at a ratio of 1.6:1.(4) The country presents significant regional differences, having large areas that are quite underdeveloped, areas that are developed and areas where the two conditions can be found. These regions present a broad range of cancer mortality rates. In the southern and southeastern regions, the rates are higher but in decline, whereas they are lower but on the rise in the northern and northeastern regions.(2) Lung cancer is characterized by low survival rates, five-year survival being approximately 15%. One of the reasons for these low rates is that most patients are diagnosed when the disease has already become advanced, locally or disseminated, since early-stage lung tumors are asymptomatic. Despite all efforts to reach an early diagnosis and develop more effective treatments, this situation has changed little over the years.(5)
There are no data in the literature regarding the characteristics of patients with lung cancer in the northern region of the country, and the present study was therefore carried out as a means of redressing this lack. The primary objective of the study was to analyze the characteristics of cases of lung cancer in a group of patients in the city of Manaus.
MethodsThis was a retrospective descriptive study of cases of lung cancer treated between January of 1995 and December of 2002 at the Portuguese Beneficent Society Getúlio Vargas University Hospital or at the Amazonas State Foundation Center for Cancer Research, Prevention, Education and Treatment. These two hospitals are the only treatment centers for patients with cancer in the city of Manaus.
Data were collected from the patient medical charts on file at the hospitals mentioned above. The following aspects were investigated: epidemiological profile; tobacco intake; histological type; staging; treatment; and survival. The tobacco intake obtained from the medical charts was calculated based on patient-reported information: the number of cigarettes smoked per day (20 cigarettes = 1 pack) was multiplied by the number of years of smoking in order to determine the number of pack-years (e.g., 2 packs/day for 1 year = 2 pack-years). The dates of death were obtained preferably by analyzing the medical charts or by searching the Amazonas State Health Department database. When necessary, this information was obtained from the family members of patients.
The classification of lung cancer used was that recommended by the World Health Organization in 1999.(6) Patients were classified using the tumor-node-metastasis staging system.(7) After receiving a histopathological diagnosis of lung cancer, patients underwent computed axial tomography of the chest, abdomen and skull, as well as bone scintigraphy, in order to determine staging.
The inclusion criteria were availability of data regarding histopathological examination with specific diagnosis and availability of data regarding patient survival.
The present study was approved by the Ethics in Research Committee of the Federal University of Amazonas.
Data were analyzed using the program Epi Info for Windows 2004, version 3.2, and the results are presented in life tables. The survival rates were calculated by means of actuarial analysis, thereby generating all survival curves for the patients with lung cancer in the city of Manaus during the study period. The survival curves were stratified by staging, gender, treatment (yes/no), histological type, type of treatment and surgical treatment (yes/no). The number of deaths observed in each group was compared using the log-rank test and Pearson's chi-square test (the level of significance being set at 5%).
ResultsOf the 441 patients initially diagnosed with lung cancer, 352 met the inclusion criteria, since the data related to 89 patients included information regarding specific histopathological examination but not regarding survival. Of those 352 patients, 262 (74.4%) were male and 90 (25.6%) were female. The means age was 62 years.
Information regarding smoking was found in the medical charts of 180 patients, and, of those, 172 (95.6%) were smokers. The mean tobacco intake was 46 pack-years.
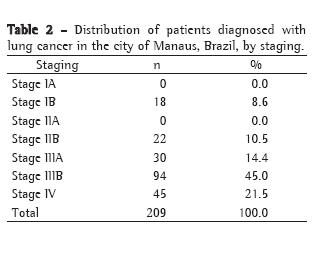
The following histological types were identified (Table 1): squamous cell carcinoma, in 62.8%; adenocarcinoma, in 24.7%; small cell carcinoma, in 9.1%; and large cell carcinoma, in 3.4%. The most common stages were stages IIIB and IV, in 45% and 21.5%, respectively (Table 2). Of the total sample, 73.4% were submitted to treatment. Of those, 51.4% underwent radiotherapy, 16.6% underwent surgery, 16.2% underwent radiotherapy combined with chemotherapy and 15.8% underwent chemotherapy alone.
As shown in the probability curve (Figure 1), the mean survival was 11.7 months, three-year survival was 6.5%, and five-year survival was 3.5%.
In men and women, five-year survival was 4.3% and 3.1%, respectively. However, this difference was not significant (p = 0.78).


Five-year survival rates for stages IB, IIB, IIIB and IV were 19.8%, 4.5%, 5.6% and 0%, respectively (Figure 2), the difference between stages IB and IIB being statistically significant (p = 0.014).

Mean five-year survival was 4% in patients with squamous cell carcinoma, 4.7% in those with adenocarcinoma and 0% in those with small cell carcinoma or large cell carcinoma. There was no statistical difference among the histological types (p = 0.8127).
Survival was 4.5 times higher in patients who were submitted to some type of treatment than in those who were not. As a result of the treatments used, five-year survival was 15.5% in patients who underwent surgery, 4.9% in those who underwent chemotherapy, 2.9% in those who underwent radiotherapy and 0% in those who underwent chemotherapy in association with radiotherapy. There was a statistically significant difference in terms of survival between patients who underwent treatment and those who did not (p = 0.0005), as well as between patients who underwent surgical treatment and those in whom another treatment modality was applied (p = 0.005; Figure 3).
 Discussion
DiscussionAmong all types of cancer, lung cancer presents one of the lowest survival rates, which varies according to the population studied. In studies conducted in North America, Europe, South America and Greece, lung cancer survival rates were found to be 15.5%, 10.8%, 14% and 18.75%, respectively. Therefore, it is possible to observe that lung cancer is an extremely aggressive type of cancer, with low survival rates. When survival among different types of lung cancer is studied, bronchogenic carcinoma is identified as the type presenting the worst prognosis.(6,8) This has also been reported in studies conducted in European countries.(9,10) In the Americas, five-year survival rates as high as 28% are found.(11,12) Although the survival rates for lung cancer obtained in our study were lower than those observed in most of the studies found in the literature, a study of the indigenous population in Australia reported a survival rate similar to that found in our study, in which the five-year survival rate was only 5.2%.(13)
Some authors have reported that women with lung cancer present higher survival rates than do men, regardless of stage at diagnosis, cell type or treatment instituted.(14) In addition, when evaluating only patients who underwent resection, better survival rates are identified among women, especially those whose tumors were classified as stage I at the time of the operation.(15,16) There was no gender-related statistical difference in terms of overall survival rates in our sample, a finding that is in agreement with those of other authors.(5,17)
Smoking constitutes the principal trigger for lung cancer, accounting for one in four deaths from lung cancer among European men.(18) However, most physicians do not investigate tobacco intake in patients with lung cancer. Approximately 88% and 71% of all lung cancer deaths are related to the smoking habit in men and women, respectively. In the present study, nearly all of the patients (95.6%) were smokers. Mortality rates among women have been increasing in recent decades, whereas those among men have declined, reflecting the historic gender-related differences in tobacco consumption trends.(18) A seven-decade retrospective study showed that smoking reduction constitutes an important measure to increase survival rates.(19)
At the time of lung cancer diagnosis, approximately 50% of patients present stage IV, 30% present stage III and 10% present stage I or II.(3) In our study, most patients (66.5%) were classified as having advanced stage tumors (stage IIIB or IV) at diagnosis, which might account for the low survival rates.
The influence of staging on patient survival can be better observed when survival rates are calculated by stage. Stage I survival rates range from 16 to 95 months, stage II survival rates range from 9 to 78 months, stage III survival rates range from 7 to 33 months and stage IV survival rates range from 3 to 19 months.(10,20) In our study, we observed that the stages presenting the best prognosis corresponded to only 19.1% of the cases, whereas most patients (80.9%) presented stages III or IV, drastically affecting the survival rates.
In general, lung cancer does not present uniform behavior, thereby involving various histological types with different biological activity and different degrees of aggressiveness. Therefore, awareness of the histological type involved and the anatomical extent of the neoplasm are of utmost importance for selecting the appropriate treatment and for
obtaining better patient survival rates.
In our sample, the evaluation of survival in non-small cell carcinoma reveals that large cell carcinoma is responsible for the lowest rates, as has also been reported by various other authors.(9,11,21) In such cases, the probability of patients whose tumors were resected presenting temporary cure ranges from 60% to 80%, so that, according to the initial presentation of the tumor, there can be local recurrence or distant metastasis, thereby contributing to the low survival rates mentioned.(22)
Clinical and pathological staging of non-small cell carcinoma, however, have presented discrepancies. It has been observed that higher clinical stages translate to greater discrepancies, with a kappa index of 0.74 (IA) and 0.33 (IB). A retrospective study, involving 180 patients, demonstrated that the concordance between clinical and pathological staging was 77% for stage IA, 51.6% for stage IB, 42.2% for stage IIB and 33.3% for stage IIIB. In addition, 26% of the patients were understaged regarding lymph node involvement. Such clinical understaging, as well as the less common overstaging, can affect survival rates among patients with lung cancer.(23) The low survival rates found in our study might be related to the understaging of patients.
Squamous cell carcinoma typically presents the highest survival rates and has been shown to constitute the most common cell type,(9,11,20) which corroborates our findings. However, in recent decades, adenocarcinoma, which is the histological type with the best prognosis among women,(21)
has presented an increasing incidence, surpassing that of the squamous type in various studies in the literature.(15) Studies have concluded that the increased incidence of the former was due to changes in smoking behavior and in the type of cigarettes. The increased production of nitrogen oxides contributes to the increased formation of tobacco-specific nitrosamines, constituting a possible factor for the increased incidence of adenocarcinoma. In experiments on rats, these nitrosamines induced lung carcinoma, predominantly adenoma and adenocarcinoma.(24)
The modern staging systems require precision, since physicians tend to base their recommendations for surgery, as well as for neoadjuvant and adjuvant treatment, on the staging classification.(1)
Among the treatments used, surgery with the intent to cure-indicated for stages I and IIA/B-(15) is the one with the best results in terms of survival,(25) with five-year survival rates ranging from 50% to 80% in stage I, from 35% and 50% in stage II(14) and reaching up to 70.8% when such treatment is possible in stage IA.(26,27) After receiving surgical treatment, most patients with lung cancer in stages T1 or N1 present better prognoses than do patients with stage IIIB or IV tumors.(28) In contrast, in our study, five-year survival for patients who underwent surgery was below 16%, much lower than that found in other studies. This discrepancy could be explained by the preoperative understaging.
The combination of radiotherapy and chemotherapy has been shown to improve life expectancy of patients classified as having stage III tumors. The great technical advances in radiotherapy, together with the development of drugs with the same therapeutic effect and fewer side effects, are also noteworthy.(22)
Radiotherapy, despite having lower efficacy than does surgery, can provide favorable results, especially in patients who undergo radical radiotherapy.(29) As previously mentioned, chemotherapy alone is typically used in advanced cases, survival rates therefore being low in such cases. In addition to the improvement in quality of life, despite the side effects of the chemotherapeutic agents, the mean survival rate in responsive patients has been reported to be as high as 15 months,(30) slightly higher than that found in our study (11.7 months).
The great number of patients referred for radiotherapy in the present study can be explained by the fact that, during a seven-year period (1995-2002), there was no thoracic surgeon at the Foundation Center for Cancer Research, Prevention, Education and Treatment.
The present study has limitations because it was a retrospective study. However, it surely revealed our current situation regarding lung cancer. Attempts at improving survival of patients with lung cancer include the restructuring of the health care system, with availability of equipment and the development of human resources, so that this disease, whose mortality rates are so high, can be detected earlier.
In conclusion, we found that, in the group of patients studied, unlike in most patient populations evaluated in recent studies in the literature, squamous cell carcinoma was the most common type of neoplasia. In this group of patients with lung cancer studied in the city of Manaus, survival rates were quite low. This might be attributable to the advanced stage of the disease at diagnosis, which is a result of the limited access to the health care system.
References 1. Zamboni M. Epidemiologia do câncer do pulmão. J Pneumol. 2002;28(1):41-7.
2. Castro MS, Vieira VA, Assunção RM. Padrões espaço-temporais da mortalidade por câncer de pulmão no Sul do Brasil. Rev Bras Epidemiol. 2004;7(2):131-43.
3. Barros JA, Valladares G, Faria AR, Fugita EM, Ruiz AP, Vianna AG, et al. Early diagnosis of lung cancer: the great challenge. Epidemiological variables, clinical variables, staging and treatment. J Bras Pneumol. 2006;32(3):221-7.
4. Brasil. Ministério da Saúde. Secretaria de Atenção à Saúde. Instituto Nacional de Câncer. Coordenação de Prevenção e Vigilância de Câncer. Estimativas 2008: Incidência de Câncer no Brasil. Rio de Janeiro: INCA; 2007.
5. Uehara C, Santoro I, Jamnik S. Câncer de Pulmão: comparação entre os sexos. J Pneumol. 2000;26(6):286-90.
6. World Health Organization. Histological typing of lung tumors and pleural tumors. 3rd ed. Geneva: WHO; 1999. p. 28.
7. Mountain CF. Revisions in the International System for Staging Lung Cancer. Chest. 1997;111(6):1710-7.
8. Gatta G, Capocaccia R, Coleman MP, Gloeckler Ries LA, Hakulinen T, Micheli A, et al. Toward a comparison of survival in American and European cancer patients. Cancer. 2000;89(4):893-900.
9. Trédaniel J, Boffetta P, Chastang C, Hirsch A. Clinico-pathological features and survival of lung cancer patients in Paris, France. Eur J Cancer. 1995;31A(13-14):2296-301.
10. Janssen-Heijnen ML, Coebergh JW. The changing epidemiology of lung cancer in Europe. Lung Cancer. 2003;41(3):245-58.
11. Younes RN, Deutsch F, Badra C, Gross J, Haddad F, Deheinzelin D. Nonsmall cell lung cancer: evaluation of 737 consecutive patients in a single institution. Rev Hosp Clin Fac Med Sao Paulo. 2004;59(3):119-27.
12. Xie L, Ugnat AM, Morriss J, Semenciw R, Mao Y. Histology-related variation in the treatment and survival of patients with lung carcinoma in Canada. Lung Cancer. 2003;42(2):127-39.
13. Condon JR, Barnes T, Armstrong BK, Selva-Nayagam S, Elwood JM. Stage at diagnosis and cancer survival for Indigenous Australians in the Northern Territory. Med J Aust. 2005;182(6):277-80.
14. International Early Lung Cancer Action Program Investigators; Henschke CI, Yip R, Miettinen OS. Women's susceptibility to tobacco carcinogens and survival after diagnosis of lung cancer. JAMA. 2006;296(2):180-4. Erratum in: JAMA. 2008;299(15):1775.
15. Abreu CM, Chatkin JM, Fritscher CC, Wagner MB, Pinto JA. Long time survival rate in lung carcinoma after surgical treatment: is gender a prognostic factor? J Bras Pneumol. 2004;30(1):2-8.
16. Pauk N, Kubík A, Zatloukal P, Krepela E. Lung cancer in women. Lung Cancer. 2005;48(1):1-9.
17. Ouellette D, Desbiens G, Emond C, Beauchamp G. Lung cancer in women compared with men: stage, treatment, and survival. Ann Thorac Surg. 1998;66(4):1140-3; discussion 1143-4.
18. Zorrilla-Torras B, García-Marín N, Galán-Labaca I, Gandarillas-Grande A. Smoking attributable mortality in the community of Madrid: 1992-1998. Eur J Public Health. 2005;15(1):43-50.
19. Kabir Z, Connolly GN, Clancy L, Jemal A, Koh HK. Reduced lung cancer deaths attributable to decreased tobacco use in Massachusetts. Cancer Causes Control. 2007;18(8):833-8.
20. Marel M, Kalina P, Melínová T, Krenarová J, Lutzbauerová J, Rehorová Z. Epidemiological studies on lung cancer in the Bohemia region. Lung Cancer. 1994;10(5-6):325-31.
21. Cerfolio RJ, Bryant AS, Scott E, Sharma M, Robert F, Spencer SA, et al. Women with pathologic stage I, II, and III non-small cell lung cancer have better survival than men. Chest. 2006;130(6):1796-802.
22. Carvalho HA. Radioterapia no câncer de pulmão. J Pneumol. 2002;28(6):345-50.
23. Santos PA, Rocha RS, Pipkin M, Silveira ML, Cypel M, Rios JO, et al. Concordance between clinical and pathological staging in patients with stages I or II non-small cell lung cancer subjected to surgical treatment. J Bras Pneumol. 2007;33(6):647-54.
24. Alberg AJ, Samet JM. Epidemiology of lung cancer. Chest. 2003;123(1 Suppl):S21-S49.
25. Van Schil PE. Surgery for non-small cell lung cancer. Lung Cancer. 2001;34(Suppl 2):S127-S32.
26. Fang D, Zhang D, Huang G, Zhang R, Wang L, Zhang D. Results of surgical resection of patients with primary lung cancer: a retrospective analysis of 1,905 cases. Ann Thorac Surg. 2001;72(4):1155-9.
27. Naruke T, Tsuchiya R, Kondo H, Asamura H. Prognosis and survival after resection for bronchogenic carcinoma based on the 1997 TNM-staging classification: the Japanese experience. Ann Thorac Surg. 2001;71(6):1759-64.
28. Flieder DB. Commonly encountered difficulties in pathologic staging of lung cancer. Arch Pathol Lab Med. 2007;131(7):1016-26.
29. Schaafsma J, Coy P. The effect of radiotherapy on the survival of non-small cell lung cancer patients. Int J Radiat Oncol Biol Phys. 1998;41(2):291-8.
30. Klastersky J, Paesmans M. Response to chemotherapy, quality of life benefits and survival in advanced non-small cell lung cancer: review of literature results. Lung Cancer. 2001;34(Suppl 4):S95-S101.
About the authors
Fernando Luiz Westphal
Coordinator of the Teaching and Research Center. Getúlio Vargas University Hospital, Federal University of Amazonas, Manaus, Brazil.
Luis Carlos de Lima
Head of the Department of Thoracic Surgery. Getúlio Vargas University Hospital, Federal University of Amazonas, Manaus, Brazil.
Edson Oliveira Andrade
Head of the Department of Pulmonology. Foundation Center for Cancer Research, Prevention, Education and Treatment, Manaus, Brazil.
José Corrêa Lima Netto
Attending Physician in the Department of Thoracic Surgery. Getúlio Vargas University Hospital, Federal University of Amazonas, Manaus, Brazil.
Andrei Salvioni da Silva
Resident. Getúlio Vargas University Hospital, Federal University of Amazonas, Manaus, Brazil.
Bruna Cecília Neves de Carvalho
Medical Student. Federal University of Amazonas, Manaus, Brazil.
Study carried out at the Federal University of Amazonas, Manaus, Brazil.
Correspondence to: Fernando Luiz Westphal. Avenida Perimetral, 2450, Residencial Jardim Itália, Edifício Turin, apto. 401, Parque 10, CEP 69055-021, Manaus, AM, Brasil.
Tel 55 92 234-6334. E-mail: f.l.westphal@uol.com.br
Financial support: None.
Submitted: 11 March 2008. Accepted, after review: 8 August 2008.








