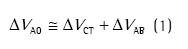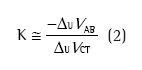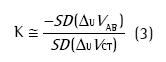ABSTRACT
Objective: To compare two methods of respiratory inductive plethysmography (RIP) calibration in three different positions. Methods: We evaluated 28 healthy subjects (18 women and 10 men), with a mean age of 25.4 ± 3.9 years. For all of the subjects, isovolume maneuver calibration (ISOCAL) and qualitative diagnostic calibration (QDC) were used in the orthostatic, sitting, and supine positions. In order to evaluate the concordance between the two calibration methods, we used ANOVA and Bland-Altman plots. Results: The values of the constant of proportionality (K) were significantly different between ISOCAL and QDC in the three positions evaluated: 1.6 ± 0.5 vs. 2.0 ± 1.2, in the supine position, 2.5 ± 0.8 vs. 0.6 ± 0.3 in the sitting position, and 2.0 ± 0.8 vs. 0.6 ± 0.3 in the orthostatic position (p < 0.05 for all). Conclusions: Our results suggest that QDC is an inaccurate method for the calibration of RIP. The K values obtained with ISOCAL reveal that RIP should be calibrated for each position evaluated.
Keywords:
Plethysmography; Respiratory mechanics; Posture; Calibration.
RESUMO
Objetivo: Comparar dois métodos de calibração da pletismografia respiratória por indutância (PRI) em três posturas diferentes. Métodos: Foram avaliados 28 indivíduos saudáveis (18 mulheres e 10 homens), com média de idade de 25,4 ± 3,9 anos. Todos os indivíduos foram submetidos a isovolume maneuver calibration (ISOCAL, calibração por manobra de isovolume) e qualitative diagnostic calibration (QDC, calibração diagnóstica qualitativa) em ortostatismo, sedestação e decúbito dorsal. Foi utilizada ANOVA e a disposição gráfica de Bland-Altman para a avaliação da concordância dos métodos de calibração. Resultados: Os valores da constante de proporcionalidade (K) foram significativamente distintos entre ISOCAL e QDC nas três posturas avaliadas: 1,6 ± 0,5 vs. 2,0 ± 1,2, em decúbito dorsal; 2,5 ± 0,8 vs. 0,6 ± 0,3, em sedestação; e 2,0 ± 0,8 vs. 0,6 ± 0,3, em ortostatismo (p < 0,05 para todos). Conclusões: Nossos resultados sugerem que QDC não é um método acurado para a calibração da PRI. Os valores de K obtidos por ISOCAL mostram que a PRI deve ser calibrada para cada postura avaliada.
Palavras-chave:
Pletismografia; Mecânica respiratória; Postura; Calibragem.
IntroductionIn the last decades, considerable attention has been directed to methods for noninvasive measurement of the chest wall.(1,2) Chief among the most commonly used methods for assessing thoracoabdominal configuration and coordination is respiratory inductive plethysmography (RIP), established in 1967 by Konno & Mead, who proposed a mathematical model that allowed quantitative assessment of spontaneous respiratory movements.(3) The equation of the proposed model is as follows:
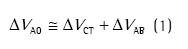
where ∆VAO is the measured change in airway volume, ∆VCT is the change in rib cage volume, and ∆VAB is the change in abdominal volume.(3,4)
Respiratory inductive plethysmographs are generally composed of two elastic bands that are placed around the rib cage and abdomen for movement transduction. These bands generate electrical signals that are proportional to the movements of the thoracic and abdominal compartments. Therefore, they should be previously calibrated for correct evaluation of the respiratory system. Chief among the various methods for calibrating respiratory inductive plethysmographs are isovolume maneuver calibration (ISOCAL),(3) which is considered the gold standard, and qualitative diagnostic calibration (QDC).(4)
For ISOCAL, the subject is instructed to shift volumes between the rib cage and abdomen voluntarily and with occluded airways. This respiratory maneuver causes the ∆VAO value to be zero, therefore establishing the following equation:
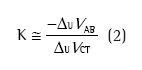
where K estimates the relative contribution of the electrical signals related to the rib cage (∆UVCT) and abdomen (∆UVAB), the signals being uncalibrated (U).(2-7)
The QDC method is performed during a given period of baseline breathing and uses a statistical approximation to equation 2 for determining K without the performance of respiratory maneuvers. The equation that rules QDC is as follows:
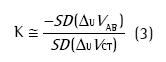
where SD(∆UVAB) and SD(∆UVCT) are the standard deviations of the electrical signals related to the abdomen and rib cage, respectively.(4,8,9)
Although ISOCAL is considered the gold standard for RIP calibration, the vast majority of studies employ QDC because the method requires no specific respiratory maneuvers.(10-13) We are unaware of any studies comparing the two methods of RIP calibration regarding the values of the constant K when different positions are employed.
MethodsWe evaluated a convenience sample of 28 adult volunteers (18 women and 10 men; age, 18-65 years) with no history of disease. The exclusion criteria were being a smoker, having been diagnosed with a respiratory disease, having difficulty in understanding explanations and instructions on how to perform the respiratory maneuvers, having a rib cage deformity, having a musculoskeletal disease that altered respiratory mechanics, and presenting with spirometric changes. The local research ethics committee approved the study (Protocol no. 1221/09), and all volunteers gave written informed consent.
The sequence in which the calibration methods and the positions were to be tested was established by random sampling. The study protocol comprised the following steps: obtaining anthropometric data (weight and height) with the use of a calibrated mechanical scale (Welmy S.A., Santa Bárbara do Oeste, Brazil); performing pulmonary function tests (Quark PFT; Cosmed, Rome, Italy); calibrating the electrical signals emitted by the elastic bands; calibrating the flow to be measured by the pneumotachograph; placing the two elastic bands, which were adapted to the size of the subjects, around the chest and abdomen for movement transduction; randomizing the sequence in which the calibration methods (ISOCAL and QDC) were to be tested; and randomizing the sequence in which the (supine, sitting, and orthostatic) positions were to be tested.
The respiratory inductive plethysmograph (Respitrace; NIMS Inc., Miami, FL, USA) used in our study is composed of two elastic bands for movement transduction (Inductotrace System, Ambulatory Monitoring, Ardsley, NY, USA). These bands have several numerical markings, adaptable to any subject, as well as an oscillator and a system for analog signal acquisition and conditioning. The device was connected to the system of a 12-bit analog-digital converter (USB 1208LS, Measurement Computing, Norton, MA, USA), which works at a sampling frequency of 50 Hz, for digital analysis of the data obtained. A Fleisch no. 2 pneumotachograph (Hugo Sachs Elektronik, Freiburg, Germany) and a differential pressure transducer (model HCXPMQ05D6V; Sensortechnics, Puchheim, Germany) were connected to the respiratory inductive plethysmograph for airflow monitoring. In order to prevent water vapor from the exhaled air from condensing in the pneumotachograph, a heating system in the pneumotachograph was supplied with 6 V of alternating current. In addition, a saliva collector was placed between the pneumotachograph and the mouthpiece. The analog electrical signal generated by the differential pressure transducer was amplified by an electronic system with an instrumentation amplifier (model AD620; Analog Devices, Norwood, MA, USA).
The flow signals, as well as the variations in thoracic and abdominal volumes, were integrated and digitized in LabVIEW, version 8.5 (National Instruments, Austin, TX, USA). The signals were monitored in real time, which allowed us to start or stop data recording for subsequent analysis. Signal processing was performed in MATLAB (The Mathworks, Natick, MA, USA), which allowed us to detect the respiratory cycles of the three signals available, as well as to calculate the respiratory parameters and the values of the constant of proportionality (K) of the electrical signals of the thoracic and abdominal compartments. The ISOCAL and QDC K values were calculated from the data related to the respiratory isovolume maneuver and the 5-min sampling period, respectively.
For ISOCAL, the volunteers were instructed on how to perform the required respiratory maneuver, i.e., with the nostrils occluded by a nose clip,(3) in order to avoid the learning effect prior to electrical signal recording. For QDC, the volunteers were instructed to breathe calmly through the mouthpiece of the pneumotachograph for a sampling period of 5 min.(4) In order to ensure upper airway occlusion, a nose clip was used.
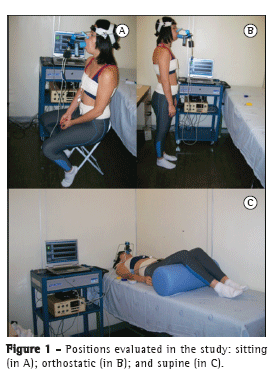
Calibrations were made for each method and for each of the three positions studied. For the supine position, the volunteers were placed horizontally on a stretcher, lying on their backs, with the hips and knees flexed; for the sitting position, the volunteers were sat on a chair without back support, with the hips and knees at a 90° angle; and for the orthostatic position, the volunteers were instructed to stand upright, with arms relaxed at their sides, and distribute their body weight evenly on both legs (Figure 1).
Normality of the data was evaluated by the Kolmogorov-Smirnov test, and the data are expressed as medians (nonparametric data) or as means and respective confidence intervals (parametric data). Repeated measures ANOVA was used for comparing the parameters evaluated, and the level of significance was set at 5% (p < 0.05). In order to evaluate the concordance between the two calibration methods, we used Bland-Altman plots (Figure 2). The statistical analyses were performed with the programs SigmaStat, version 9.1 (Systat Software Inc., San Jose, CA, USA), and MedCalc (MedCalc Software, Mariakerke, Belgium).
 Results
ResultsThe anthropometric characteristics of the study participants are shown in Table 1.
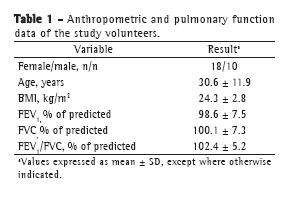
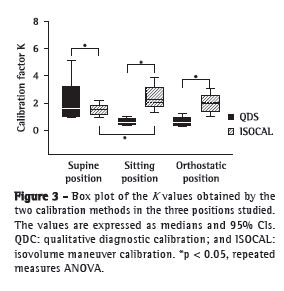
Calibrations were evaluated by a comparative analysis of the constant of proportionality (K). The values of the constant K are shown in Figure 3, which shows that, in the three positions evaluated, the values obtained with the QDC method were different from those obtained with the ISOCAL method. In the supine position, the K values obtained with QDC were significantly higher than were those obtained with ISOCAL (2.2 ± 1.6 vs. 1.50 ± 0.47; p < 0.05). In contrast, in the sitting and orthostatic positions, the K values obtained with QDC were significantly lower than were those obtained with ISOCAL (0.6 ± 0.3 vs. 2.4 ± 0.9 and 0.6 ± 0.3 vs. 1.9 ± 0.7; p < 0.05 for both). There were no differences between the K values obtained with QDC in the supine position and those obtained with ISOCAL in the orthostatic position.
The Bland-Altman plot revealed non-concordance between the calibration methods in the different positions evaluated. As can be seen in Figure 2, the difference between the two methods increases along the x axis, i.e., with the increase in the mean values of the two calibrations (Figure 2).
With regard to the contribution of the thoracic and abdominal compartments, we found that, in the three positions evaluated, the contribution of the rib cage was greater than was that of the abdomen, given that the K values obtained with ISOCAL were greater than 1.0 in the supine, sitting, and orthostatic positions (1.5 ± 0.4; 2.4 ± 0.9; and 1.9 ± 0.7, respectively). The addition of the flow monitoring system allowed accurate evaluation of the respiratory variables, which were measured during baseline breathing (Table 2).
 Discussion
DiscussionThe present study showed that, regardless of the calibration method, the K values differed among the three positions, which suggests that calibration should be performed for each position evaluated. In addition, the results obtained by QDC were found to be different from those obtained by ISOCAL, regardless of the position evaluated, suggesting that the former cannot be considered accurate.
It is a fact that RIP has been widely used; however, because of the difficulty in performing the gold standard method (ISOCAL), various studies have suggested the use of the QDC method.(11-14) One of the major advantages of the QDC method is that it is easy to perform, given that, for QDC, individuals need only maintain baseline breathing for 5 min, and calibration is performed on the basis of the variation in the results obtained for each compartment. This method is questionable in view of the RIP calibration principle, i.e., variation in calibration because of volume shifts between the rib cage and abdomen.(3) In addition, the QDC method requires that subjects maintain a breathing pattern throughout the measurement period, which does not seem to have happened during our measurements.
Sackner et al.(4) hypothesized that QDC requires a constant breathing pattern in order to allow the determination of K. However, our findings show that there was wide dispersion of respiratory cycle times, associated with high standard deviation values for tidal volume during baseline breathing (Table 2). These data suggest that, during data collection for QDC, the breathing pattern was not constant, which in turn suggests that 5 min of quiet breathing for data acquisition might not be sufficient to determine the K value for the contribution of the thoracic and abdominal compartments. In this sense, a study conducted by Sartene et al.(7) demonstrated that, during quiet breathing, there is dispersion of approximately 20% of the mean tidal volume, and only 8% of this value corresponds to the contribution of the thoracic and abdominal compartments. Therefore, the authors stated that the use of calibrations requiring quiet breathing is questionable when quiet breathing is employed in devices with two degrees of freedom, given that most of the study participants, when evaluated in the supine position, predominantly used only one degree of freedom.
Our findings are corroborated by those reported in a study by Thompson,(15) who also found differences between the two calibration methods in terms of the values of the constant K. In that study, Thompson suggested that QDC has significant limitations related to the calculation of K, given that the sum of the reading of the signals is considered to be constant for the thoracic and abdominal compartments, and that the participation of each compartment is obtained by subtracting this estimate. De Groote et al.(8) demonstrated that decreased variability in the contribution of the thoracic and abdominal movements can generate an inaccurate calibration factor when measurements are taken during breathing at constant or nearly constant tidal volume, as is the case with QDC.
In children, the QDC method was found to be unreliable for estimating tidal volume.(11) According to the authors, the contributions of the rib cages and abdomens of anesthetized children were insufficient to derive K. One of the findings of the present study was the contribution of the rib cage to the tidal volumes obtained, which were unexpectedly high. In contrast, Adams et al.(14) reported obtaining satisfactory K values when QDC was performed in neonates. However, the authors did not evaluate the relative contribution of the thoracic and abdominal compartments or the accuracy of the K values obtained.
Our study has some potential limitations. The measurements were taken by a pneumotachograph, with the volunteers breathing through the mouth, mouth breathing having been ensured by the use of a nose clip. This might have changed the flow of inspired air and the breathing pattern. Nevertheless, we found no significant changes in the breathing pattern with the addition of the flow monitoring system to the RIP system. We believe that our choice of a Fleisch pneumotachograph, which is considered a low-resistance flow transducer, might have contributed positively to the breathing pattern observed.
Although it is considered unattractive from a practical standpoint, ISOCAL remains the gold standard for RIP calibration.(16) In our study, we tried to ensure the quality of the data obtained by instructing the volunteers on how to perform the respiratory maneuver for ISOCAL. This might be a strategy to facilitate the use of this calibration method. Our hypothesis is that even the ISOCAL method is influenced by body position. We are aware of only one study demonstrating that postural changes, especially in the transitions from the orthostatic position to the sitting position, lead to changes in volume-motion coefficients, changes that can significantly affect the accuracy of the calibration method and, consequently, the estimates of volume derived from RIP signals.(17)
The results of our study were similar to those reported by Zimmerman et al.,(17) given that there were differences among the positions evaluated even for the calibration method considered the gold standard (ISOCAL), and those differences were even more pronounced in the transitions from the orthostatic position to the sitting position (Figure 3). Our results suggest that RIP should be calibrated for each position evaluated when used for estimating thoracic and abdominal volumes in the same individual.
With regard to the participation of the thoracic and abdominal compartments in ventilation, we found greater contribution of the rib cage to tidal volume in the three positions evaluated (Figure 3), given that the mean K values (ratio between thoracic and abdominal participation) obtained with the ISOCAL method were greater than 1.0 in the supine, sitting, and orthostatic positions. This result is corroborated by those reported in a study by Verschakelen & Demedts,(16) who demonstrated that there is greater contribution of the rib cage in higher positions, such as the sitting and orthostatic positions. According to the same authors, the contribution of the rib cage, especially in higher positions, is greater in women than in men. In the present study, women predominated (65.2%), which could also explain the K values obtained in the two positions. In addition, the movements of the rib cage and abdomen depend on the state of contraction of the respiratory muscles, and the contribution of the diaphragm to the movement of those compartments depends on gravity. Therefore, the participation of the abdomen in ventilation will be greater in the orthostatic position than in the sitting position because of the hydraulic action of the abdominal contents, which favors increased abdominal compliance.(18) The data obtained in our study confirm this hypothesis; although there was greater contribution of the rib cage in the two positions, the K value obtained for the orthostatic position (1.9 ± 0.7) was lower than was that obtained for the sitting position (2.4 ± 0.9). We believe that there is greater participation of the abdomen in the orthostatic position than in the sitting position, although the movement is primarily thoracic.
Although our results are considered satisfactory in terms of the applicability of ISOCAL in RIP calibration, a system for monitoring the pressure of the air trapped in the mouth during ISOCAL was not coupled to the equipment. This can be considered a major limitation of our study, given that it was impossible to determine quantitatively whether there was air compression in the mouths of the patients.(19) However, qualitatively, it was observed that the volunteers did not trap air in their mouths, given that they did not distend their cheeks.
The data obtained in the present study suggest that QDC cannot be considered an accurate method of RIP calibration and that ISOCAL should be performed for each position evaluated.
AcknowledgmentsThe authors would like to thank researchers José António Fernandes and Liane Hirano Shiguemichi for their collaboration.
References1. Banovcin P, Seidenberg J, von der Hardt H. Pressure sensor plethysmography: a method for assessment of respiratory motion in children. Eur Respir J. 1995;8(1):167-71. PMid:7744184. http://dx.doi.org/10.1183/09031936.95.08010167
2. Brüllmann G, Fritsch K, Thurnheer R, Bloch KE. Respiratory monitoring by inductive plethysmography in unrestrained subjects using position sensor-adjusted calibration. Respiration. 2010;79(2):112-20. PMid:19365103. http://dx.doi.org/10.1159/000212117
3. Konno K, Mead J. Measurement of the separate volume changes of rib cage and abdomen during breathing. J Appl Physiol. 1967;22(3):407-22. PMid:4225383.
4. Sackner MA, Watson H, Belsito AS, Feinerman D, Suarez M, Gonzalez G, et al. Calibration of respiratory inductive plethysmograph during natural breathing. J Appl Physiol. 1989;66(1):410-20. PMid:2917945.
5. De Groote A, Wantier M, Cheron G, Estenne M, Paiva M. Chest wall motion during tidal breathing. J Appl Physiol. 1997;83(5):1531-7. PMid:9375316.
6. Kondo T, Uhlig T, Pemberton P, Sly PD. Laser monitoring of chest wall displacement. Eur Respir J. 1997;10(8):1865-9. PMid:9272932. http://dx.doi.org/10.1183/09031936.97.10081865
7. Sartene R, Dartus C, Bernard JL, Mathieu M, Goldman MD. Comparison of thoracoabdominal calibration methods in normal human subjects. J Appl Physiol. 1993;75(5):2142-50. PMid:8307871.
8. De Groote A, Wantier M, Cheron G, Estenne M, Paiva M. Chest wall motion during tidal breathing. J Appl Physiol. 1997;83(5):1531-7. PMid:9375316.
9. Mayer OH, Clayton RG Sr, Jawad AF, McDonough JM, Allen JL. Respiratory inductance plethysmography in healthy 3- to 5-year-old children. Chest. 2003;124(5):1812-9. PMid:14605053. http://dx.doi.org/10.1378/chest.124.5.1812
10. Warren RH, Horan SM, Robertson PK. Chest wall motion in preterm infants using respiratory inductive plethysmography. Eur Respir J. 1997;10(10):2295-300. PMid:9387956. http://dx.doi.org/10.1183/09031936.97.10102295
11. Brown K, Aun C, Jackson E, Mackersie A, Hatch D, Stocks J. Validation of respiratory inductive plethysmography using the Qualitative Diagnostic Calibration method in anaesthetized infants. Eur Respir J. 1998;12(4):935-43. PMid:9817172. http://dx.doi.org/10.1183/09031936.98.12040935
12. Miller C, Hoffman AM, Hunter J. Thoracoabdominal asynchrony failed to grade airway obstructions in foals. J Appl Physiol. 2000;88(6):2081-7. PMid:10846021.
13. Panka GF, Oliveira MM, França DC, Parreira VF, Britto RR, Velloso M. Ventilatory and muscular assessment in healthy subjects during an activity of daily living with unsupported arm elevation. Rev Bras Fisioter. 2010;14(4):337-44. PMid:20949234. http://dx.doi.org/10.1590/S1413-35552010005000013
14. Adams JA, Zabaleta IA, Stroh D, Johnson P, Sackner MA. Tidal volume measurements in newborns using respiratory inductive plethysmography. Am Rev Respir Dis. 1993;148(3):585-88. http://dx.doi.org/10.1164/ajrccm/148.3.585
15. Thompson JR. Qualitative diagnostic calibration technique. J Appl Physiol. 1999;87(2):869-72. PMid:10484687.
16. Verschakelen JA, Demedts MG. Normal thoracoabdominal motions. Influence of sex, age, posture, and breath size. Am J Respir Crit Care Med. 1995;151(2 Pt 1):399-405. PMid:7842198.
17. Zimmerman PV, Connellan SJ, Middleton HC, Tabona MV, Goldman MD, Pride N. Postural changes in rib cage and abdominal volume-motion coefficients and their effect on the calibration of a respiratory inductance plethysmograph. Am Rev Respir Dis. 1983;127(2):209-14. PMid:6830037.
18. Agostini EP, Mognoni P, Torri G, Saracino F. Relation between changes of rib cage circumference and lung volume. J Appl Physiol. 1965;20(6):1179-86.
19. Gonzalez H, Haller B, Watson HL, Sackner MA. Accuracy of respiratory inductive plethysmograph over wide range of rib cage and abdominal compartmental contributions to tidal volume in normal subjects and in patients with chronic obstructive pulmonary disease. Am Rev Respir Dis. 1984;130(2):171-4. PMid:6465670.
* Study carried out in the Department of Physical Therapy and in the Biomedical Engineering Laboratory, University of São Paulo, São Paulo, Brazil.
Correspondence to: Celso R. F. Carvalho. Faculdade de Medicina da Universidade de São Paulo, Avenida Dr. Arnaldo, 455, sala 1210, CEP 01246-903, São Paulo, SP, Brasil.
Tel. 55 11 3061-7317. Fax: 55 11 3085-0992. E-mail: cscarval@usp.br
Financial support: None.
Submitted: 3 June 2011. Accepted, after review: 14 February 2012.
About the authorsRenata Cléia Claudino Barbosa
Master's Student in Rehabilitation Sciences. University of São Paulo School of Medicine, São Paulo, Brazil, and Assistant Professor, São
Camilo University Center, São Paulo, Brazil.
Celso Ricardo Fernandes de Carvalho
Associate Professor. Department of Physical Therapy, University of São
Paulo School of Medicine, São Paulo, Brazil.
Henrique Takachi Moriya
Assistant Professor. Biomedical Engineering Laboratory, University of São Paulo Polytechnic Institute, São Paulo, Brazil.