ABSTRACT
Objective: To determine whether a short-term protocol using subcutaneous sensitization with ovalbumin, without the use of adjuvants, would induce an eosinophilic response in the lungs of mice similar to that observed in previous, well-established protocols. Methods: Adult female BALB/c mice were randomized and divided into groups according to the number of sensitizations with ovalbumin and the number/dosage of intranasal ovalbumin challenges. The short-term protocol (10 days) consisted of one sensitization with ovalbumin and three ovalbumin challenges (100 µg). Total and differential cell counts in BAL fluid, levels of eosinophil peroxidase in lung tissue, and histopathological examination of the lungs were performed 24 h after the last ovalbumin challenge. Results: No significant differences were found among the groups regarding the variables studied. The short-term protocol, as well as the other protocols studied, induced an eosinophilic response similar to that obtained in the positive control. Conclusions: Subcutaneous sensitization with ovalbumin and without the use of adjuvants resulted in a significant allergic response in the lungs of mice, even in the short-term protocol group. Our findings suggest that this short-term protocol can be used as a first-line pre-clinical test for the study of new medications, reducing the costs and observation periods.
Keywords:
Ovalbumin; Mice; Asthma.
RESUMO
Objetivo: Determinar se um protocolo curto de sensibilização com ovalbumina subcutânea, sem adjuvante, induziria uma resposta pulmonar eosinofílica em pulmões de camundongos similar àquela encontrada em protocolos previamente estabelecidos. Métodos: Fêmeas adultas de camundongos BALB/c foram randomizadas e divididas em grupos de acordo com o número de sensibilizações com ovalbumina e o número/dosagem de provocação intranasal. O protocolo curto (10 dias) consistiu de uma sensibilização e três provocações com ovalbumina (100 µg). A contagem total e diferencial de células no lavado broncoalveolar, o nível de peroxidase eosinofílica no tecido pulmonar e o exame histopatológico dos pulmões foram realizados 24 h após a última provocação. Resultados: Não houve diferenças significativas entre os grupos em relação às variáveis estudadas. O protocolo curto, assim como os outros protocolos estudados, induziu uma resposta eosinofílica pulmonar semelhante àquela do grupo controle positivo. Conclusões: A sensibilização por ovalbumina subcutânea sem o uso de adjuvante resultou em uma significativa resposta pulmonar alérgica em ratos, mesmo no grupo de protocolo curto. Nossos achados sugerem que esse protocolo curto pode ser utilizado como teste pré-clínico de primeira linha para a pesquisa de novos fármacos, reduzindo custos e o tempo de observação.
Palavras-chave:
Ovalbumina; Camundongos; Asma.
IntroductionAsthma is a chronic lower airway disease that affects approximately 300 million people worldwide, resulting in high morbidity and substantial costs to society. Asthma is characterized by infiltration of CD4+ Th2 cells and eosinophils in the airways, associated with production of allergen-specific IgE.(1) In the study of new therapies for asthma, as well as for a better understanding of the pathophysiology of the disease, animal models have been used for decades.(2) Murine models involving systemic sensitization to antigens, with subsequent airway challenge, have been developed in order to trigger an allergic response in the lungs similar to that of asthma.(3) These models are still the most commonly used in experimental asthma research, despite some recent criticisms of factors related to current animal models of asthma, which do not develop phenotypic characteristics similar to those of asthma in humans.(4)
Among the animals studied, isogenic mice are the most popular, because they are inexpensive, there is detailed knowledge of their genetics, and there is a clear Th2 immune response in their lungs when they are exposed to specific allergens.(3) Classically, BALB/c mice are intraperitoneally sensitized with ovalbumin twice, 14 days apart, together with an adjuvant, i.e., aluminum hydroxide (alum); although this method is routinely used, it is an artificial way of boosting the allergic response in the lungs.(5) In the literature, this has been the standard protocol most commonly used as a murine model of asthma. Overcoming two frequently reported limitations (use of adjuvants and prolonged protocol duration) would be attractive for performing murine models of asthma that are more sophisticated, especially in pre-clinical testing of new drugs.
In an attempt to find an alternative to the use of adjuvants in murine models of asthma, Conrad et al. have recently demonstrated that subcutaneous sensitization with ovalbumin, without the use of adjuvants, results in an allergic response in the lungs similar to that observed in previously, well-established protocols.(6,7) The results of that study allow the exclusion of the use of adjuvants in murine models of asthma in future studies; the artificial way in which asthma is currently studied in animal models, with the use of adjuvants, has been justifiably criticized. However, in that study, there were three sensitizations, 7 days apart, and the protocol remained too long. To date, there have been no studies testing short-term protocols for use in murine models of asthma, particularly without the use adjuvants. If proven viable, this type of model would be an interesting means to evaluate, preliminarily, new therapies for asthma, particularly those related to an eosinophilic response in the lungs, such a response being a key outcome in therapeutic targets of atopic asthma. In the pharmaceutical industry setting, long-term protocols have been a significant limitation in the study of new drugs.(8)
Therefore, the objective of the present study was to find alternative protocols for animal models of asthma, i.e., protocols that are shorter and less artificial. A 10-day protocol with only one subcutaneous sensitization with ovalbumin and without the use of adjuvants was compared with standard protocols described in previous studies.
MethodsA total of 44 isogenic BALB/c mice (adult females 6-8 weeks of age) were obtained from the Rio Grande do Sul State Foundation for Health Science Research. The animals were fed a balanced chow diet and had ad libitum access to water, being housed in cages and maintained on a 12/12-h light/dark cycle. The animals were divided into the following groups:
five study groups of 7 animals each, in which different models of induction of an allergic response in the lungs were tested
one positive control (C+) group of 5 animals
one negative control (C−) group of 4 animals
The groups were classified according to the type of sensitization (intraperitoneal or subcutaneous sensitization with ovalbumin, with or without the use of adjuvants), the number of sensitizations (one or two), the number of intranasal ovalbumin challenges (two or three), the dosage of intranasal ovalbumin challenge (40 µg or 100 µg), and the observation period (21 or 10 days). The control groups were observed for 28 days.
Sensitization with ovalbumin and intranasal ovalbumin challenge were performed with total volumes of 200 µL and 50 µL, respectively, diluted in Dulbecco's PBS (DPBS). The dose of ovalbumin used for sensitization was 20 µg in all groups except the C− group. For intranasal ovalbumin challenge, the animals were anesthetized with isoflurane in an anesthesia chamber to allow pulmonary aspiration.
The animals in the study groups underwent the following:
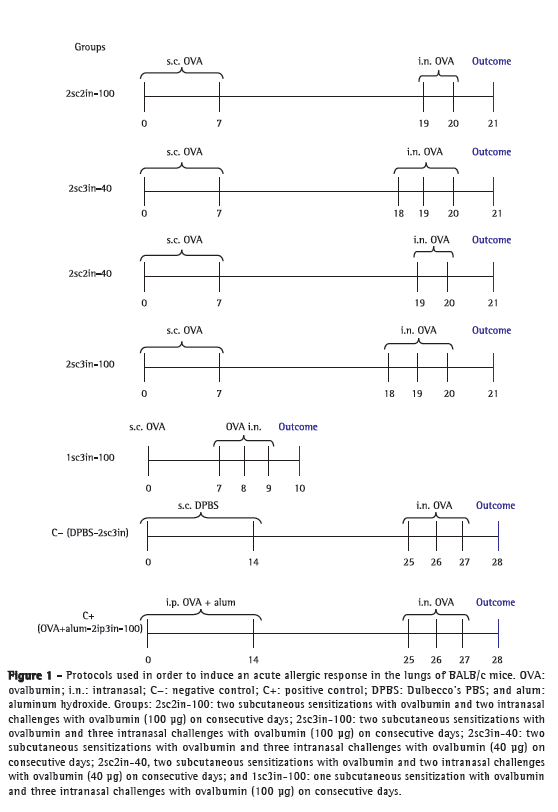
2sc2in-100 group-two subcutaneous sensitizations with ovalbumin (days 0 and 7) and two intranasal ovalbumin challenges (100 µg) on consecutive days (days 19 and 20)
2sc3in-100 group-two subcutaneous sensitizations with ovalbumin (days 0 and 7) and three intranasal ovalbumin challenges (100 µg) on consecutive days (days 18, 19, and 20)
2sc3in-40 group-two subcutaneous sensitizations with ovalbumin (days 0 and 7) and three intranasal ovalbumin challenges (40 µg) on consecutive days (days 18, 19, and 20)
2sc2in-40 group-two subcutaneous sensitizations with ovalbumin (days 0 and 7) and two intranasal ovalbumin challenges (40 µg) on consecutive days (days 19 and 20)
1sc3in-100 group (with a short observation period, which was the primary objective of the present study)-one subcutaneous sensitization with ovalbumin (day 0) and three intranasal ovalbumin challenges (100 µg) on consecutive days (days 7, 8, and 9)
The first four groups were observed for 21 days, whereas the 1sc3in-100 group was observed for 10 days (short-term protocol).
The animals in the control groups underwent the following:
C+ group: two intraperitoneal sensitizations with 1 mg of ovalbumin + alum (days 0 and 14) and three intranasal ovalbumin challenges (100 µg) on consecutive days (days 25, 26, and 27)
C− group: two subcutaneous administrations of DPBS (days 0 and 14) and three intranasal instillations of DPBS on consecutive days (days 25, 26, and 27)
The protocols are shown in Figure 1.
For BAL, the animals were anesthetized with a solution of xylazine (100 mg/mL) and ketamine (100 mg/mL), at a ratio of 1:9 (dose, 0.1 mL), and the trachea was cannulated with a blunt needle. A DPBS solution (1 mL) was instilled intratracheally and immediately aspirated. This procedure was performed three consecutive times. After the BAL procedure, the animals were euthanized with lethal doses of the drugs used for anesthesia (dose, 0.3 mL i.p.) and were disposed of in accordance with the norms of the institution.
The BAL fluid was weighed and centrifuged at 1,500 rpm for 10 min at 4°C. The precipitate was resuspended in 1 mL of DPBS. For all samples, total cell count and cell viability in the suspension were determined by the trypan blue exclusion test with a Neubauer chamber (BOECO, Hamburg, Germany). For the differential cytologic analysis, the precipitate suspension (30 g) was placed in a cytospin centrifuge for 5 min. The cells were analyzed for their morphology by the May-Grünwald-Giemsa method. The cell types observed under an optical microscope are expressed as percentages, after the counting of 200 cells.
After BAL and lung resection, we used ortho-phenylenediamine (a chromogenic substrate) in order to produce a chemical reaction and measure eosinophil activity in lung tissue. As demonstrated by Strath et al.,(9) this method allows us to quantify eosinophil activity on the basis of the eosinophil peroxidase (EPO) reaction, by measuring optical absorbance, without interference from other peroxidases that might be present in the tissue analyzed. In brief, lung tissue fragments were frozen and thawed three times in liquid nitrogen. After centrifugation for 10 min at 4°C, the supernatant was serially diluted five times in 96-well plates (50 µL/well). Subsequently, 100 mL of substrate (1.5 mM ortho-phenylenediamine and 6.6 mM hydrogen peroxide diluted in 0.05 M Tris-HCl buffer, pH 8.0) were added. After 30 min, at room temperature, the reaction was stopped by the addition of 1 M sulfuric acid, and the absorbance of the samples was measured at 492 nm.
After having been removed, the lungs were perfused with 10% buffered formalin on a gravity column (20 mmHg). The specimens were embedded in paraffin blocks, cut into 4-µm sections, stained with H&E, and mounted on slides. In order to determine the severity of eosinophilic inflammation, we performed a qualitative assessment of bronchial inflammatory response under an optical microscope, by counting the number of eosinophils in a given field, in three different bronchi.
The statistical analysis was performed with the Statistical Package for the Social Sciences, version 17.0 (SPSS Inc., Chicago, IL, USA). After descriptive analysis of the variables, we used the Kruskal-Wallis test with Dunn's post hoc test for comparisons that reached statistical significance. The C− group was statistically tested separately for each study group by the Mann-Whitney test, with adjustment for multiple comparisons. The level of statistical significance was set at 0.05. The eosinophil count in BAL fluid was used as the primary outcome measure because eosinophils are the most important immune effector cells in this experimental model.
The sample size was calculated at 7 animals per study group. This calculation was based on the following: absolute eosinophil count in BAL fluid for a mean of 0.7 × 106 cells/mL as the primary outcome measure; a standard deviation of 0.34; a value of p = 0.05; and a power of 80%, the difference among the means for the groups having been estimated at 80%.
The present study was approved by the local animal research ethics committee and was conducted in accordance with current ethical norms for animal model research, following the guidelines of the Brazilian Association for Laboratory Animal Science, using as few animals as possible, and managing pain and suffering during all procedures, including euthanasia.
ResultsIn the present study, models that induce an acute allergic response in the lungs of mice by using subcutaneous sensitization with ovalbumin and different numbers and doses of intranasal ovalbumin challenges were compared with one another and with the traditional model (C+ group). The primary goal of the study was to determine whether the use of a short-term (10-day) protocol consisting of one sensitization would induce an allergic response in the lungs similar to that observed in standard protocols in the literature. The mean BAL fluid return volume for all animals was 0.55 ± 0.15 mL, and the mean cell viability was 100%. The mean eosinophil count in the C− and C+ groups was 2.5 ± 3.0% and 40.1 ± 10.0%, respectively.
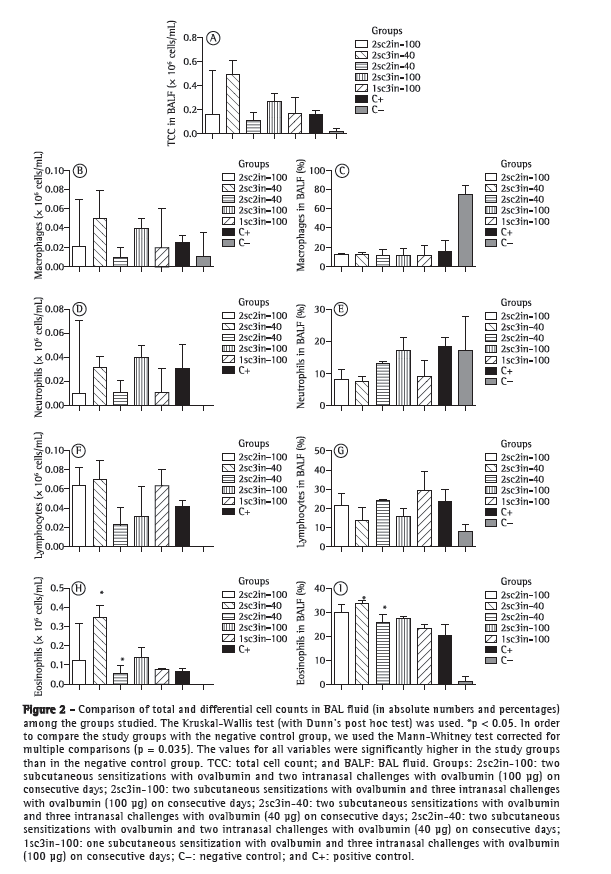
There were no significant differences between the study groups and the C+ group regarding total cell count (p = 0.1), lymphocyte count (p = 0.36), macrophage count (p = 0.24), or neutrophil count (p = 0.059) in BAL fluid. The eosinophil count was higher in the 2sc3in-40 group than in the 2sc2in-40 group (p = 0.032; Figure 2). There were no significant differences in cellular inflammatory response in the lungs between the animals undergoing the short-term protocol, without the use of adjuvants, and those undergoing the 21-day protocol that is widely used in animal models of asthma. In comparison with the C− group, the study groups showed significantly higher total and differential cell counts (p < 0.05).
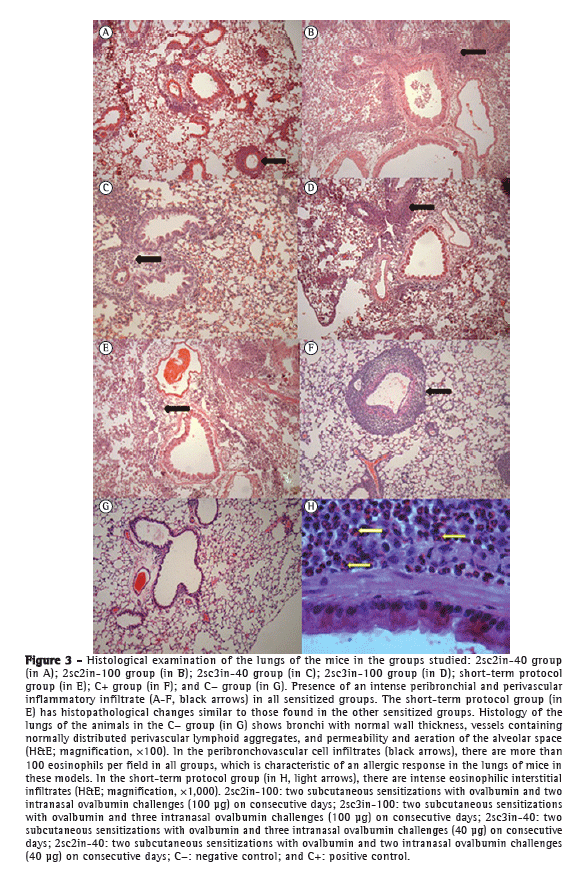
Histological examination revealed intense peribronchovascular inflammatory infiltrates in all groups, with a predominance of lymphocytes and the presence of more than 100 peribronchial eosinophils per field. The anatomy of the animals in the C− group was preserved, without inflammatory changes, a finding that is characteristic of healthy animals. From a histological standpoint, there was no difference in the severity of pulmonary inflammation among the groups, including the group undergoing the short-term protocol (Figure 3). Analysis of EPO levels in lung tissue, which reflect eosinophil activity in the lungs, revealed no differences among the groups studied (Figure 4).
 Discussion
DiscussionAnimal models of asthma with shorter-term protocols and without the use of adjuvants seem to be an attractive alternative for experimental studies of asthma in certain situations. Using the outcome variables that are more directly related to the presence and activity of eosinophils in the lung, we compared different groups of BALB/c mice sensitized with ovalbumin and found no significant differences among the different protocols studied, including a short-term (10-day) protocol.
The most important finding of the present study, especially if we take into consideration that no adjuvants were used, is that there were no differences among the protocols despite their differences in duration (10, 21, or 28 days). We demonstrated for the first time that a shorter-term protocol, without the use of adjuvants, can induce an allergic response in the lungs of mice similar to that observed in previous, well-established protocols. The use of a 10-day protocol inducing the same eosinophilic response in the lungs as that observed in previous, longer-term protocols widely used in the literature can facilitate pre-clinical trials (particularly those investigating new therapeutic targets), reducing the costs and the duration of experiments. In addition, shorter-term protocols are in accordance with all ethical principles currently guiding the use of animals in research, reducing the duration of the experimental procedures that animals undergo. There were no significant differences between the short-term protocol tested in the present study and the protocol used in the C+ group in terms of total cell counts and eosinophil counts in BAL fluid or in terms of EPO levels in lung tissue. In addition, for the short-term protocol, histological examination revealed a significant peribronchovascular inflammatory cell infiltrate, with a predominance of eosinophils, with the same characteristics as those observed for the other protocols.
In 2008, Hahn & Erb published an article questioning the time it takes to identify and develop new treatments for asthma; this process begins with identifying a molecule and determining whether it is actually involved in the disease process, and it is followed by identification of the structural components and synthetic modification of the molecule, culminating in pre-clinical testing in animals.(8) In addition to this long and costly process, there are long periods of experiments in mice. It is of note that the results obtained with the model proposed in the present study are related to the analysis of acute response to a single allergen (i.e., ovalbumin). It is also of note that experimental models of asthma involving chronic exposure have been proposed and are important in the study of new drugs, being probably performed in a later sequence of experiments, when therapeutic targets are sought.(10,11) Shorter-term protocols can nevertheless be an interesting screening model for new therapeutic targets.
In 2004, Cates et al. conducted a study involving a short-term (10-day) protocol of sensitization with house dust mites (HDM) and demonstrated eosinophilic inflammation in the lungs of mice, as well as increased expression of Th2 effector cells (CD3+, CD4+, and T1/ST2+), together with increased levels of total IgE and HDM-specific IgG1.(12) The results of that study and those of our study demonstrate that it is possible to perform a short-term (10-day) protocol using either ovalbumin or HDM.
Various authors have criticized the use of alum in murine models of asthma because alum is an artificial substance for the induction of an immune response, inducing pro-inflammatory cytokine production and activating Th2 lymphocytes.(5,13,14) Alum also activates the immune system via dendritic cell maturation and by co-stimulation of expression molecules.(15,16) In addition, alum has been shown to cause major stress in animals up to 4 h after exposure.(6) Studies in which alum was not used demonstrated that this substance is not necessary for the induction of an allergic response in the lungs of mice and that there is no difference between subcutaneous sensitization without the use of adjuvants and intraperitoneal sensitization with alum. Those studies, involving protocols without the use of adjuvants, demonstrated different levels of inflammation, different levels of immune tolerance to the allergen, or protocols that were often too long.(7,17-20) More recently, Conrad et al. found no significant differences in BAL cellularity, lung histology, or interleukin (IL-5, IL-10, and IL-13) levels using subcutaneous sensitization with ovalbumin and no adjuvants.(6) However, in that study, there were three sensitizations, which makes the experiment relatively long for an acute model of asthma. The mechanism by which subcutaneous sensitization is effective without the use of adjuvants still needs to be clearly characterized. One hypothesis is that the subcutaneous tissue compartment has a larger and more effective number of antigen-presenting cells, which results in a more robust response to a given allergen, no adjuvants being required.
The cell counts in BAL fluid in the present study showed that eosinophil counts were lower in the groups undergoing subcutaneous sensitization with ovalbumin (21 days) and two intranasal ovalbumin challenges (40 µg) than in the group undergoing three ovalbumin challenges (Figure 2). This finding can be explained by the fact that fewer intranasal ovalbumin challenges induce less inflammation in the animal. However, in the context of the primary objectives of our study, this finding does not seem to be of great relevance.
One limitation of the present study was the fact that we did not measure cytokines or ovalbumin-specific IgE or conduct pulmonary function testing. Because we did not investigate any disease mechanism or any mechanism of antigen sensitization in the present study, we believe that the analysis performed, with a major focus on eosinophil activity in the lungs (eosinophil levels in BAL fluid, eosinophil levels in histological sections, and EPO levels in lung tissue), does not significantly change the final interpretation of the results in general. However, we understand that further studies involving a better characterization of the inflammatory response in the lungs are needed in order to validate our model. One question that remains unanswered is whether this short period is sufficient for a significant production of ovalbumin-specific IgE.
In conclusion, new models of asthma using lower doses of ovalbumin, a smaller number of sensitizations, a smaller number of intranasal challenges, and no adjuvants have shown an inflammatory response in the lungs, with a predominance of eosinophils (key effector cells in Th2 immune response). Our proposed model, of shorter duration, can be a future option for pre-clinical testing and the study of therapeutic targets in asthma, reducing the duration and cost of studies, provided that new studies are carried out and the appropriateness of the model is confirmed.
References1. Taussig LM, Landau LI, editors. Pediatric respiratory medicine. St. Louis: Mosby; 1999.
2. Bates JH, Rincon M, Irvin CG. Animal models of asthma. Am J Physiol Lung Cell Mol Physiol. 2009;297(3):L401 10. PMid:19561139 PMCid:2739768. http://dx.doi.org/10.1152/ajplung.00027.2009
3. Zosky GR, Sly PD. Animal models of asthma. Clin Exp Allergy. 2007;37(7):973-88. http://dx.doi.org/10.1111/j.1365-2222.2007.02740.x
4. Szelenyi I. Animal models of bronchial asthma. Inflamm Res. 2000;49(12):639-54. PMid:11211914. http://dx.doi.org/10.1007/s000110050642
5. Eisenbarth SC. Use and limitations of alum-based models of allergy. Clin Exp Allergy. 2008;38(10):1572-5. http://dx.doi.org/10.1111/j.1365-2222.2008.03069.x
6. Conrad ML, Yildirim AO, Sonar SS, Kiliç A, Sudowe S, Lunow M, et al. Comparison of adjuvant and adjuvant-free murine experimental asthma models. Clin Exp Allergy. 2009;39(8):1246-54. http://dx.doi.org/10.1111/j.1365-2222.2009.03260.x
7. Renz H, Smith HR, Henson JE, Ray BS, Irvin CG, Gelfand EW. Aerosolized antigen exposure without adjuvant causes increased IgE production and increased airway responsiveness in the mouse. J Allergy Clin Immunol. 1992;89(6):1127-38. http://dx.doi.org/10.1016/0091-6749(92)90296-E
8. Hahn C, Erb KJ. The preclinical testing strategy for the development of novel chemical entities for the treatment of asthma. Curr Drug Targets. 2008;9(6):443-51. PMid:18537583. http://dx.doi.org/10.2174/138945008784533552
9. Strath M, Warren DJ, Sanderson CJ. Detection of eosinophils using an eosinophil peroxidase assay. Its use as an assay for eosinophil differentiation factors. J Immunol Methods. 1985;83(2):209-15. http://dx.doi.org/10.1016/0022-1759(85)90242-X
10. Johnson JR, Wiley RE, Fattouh R, Swirski FK, Gajewska BU, Coyle AJ, et al. Continuous exposure to house dust mite elicits chronic airway inflammation and structural remodeling. Am J Respir Crit Care Med. 2004;169(3):378 85. PMid:14597485. http://dx.doi.org/10.1164/rccm.200308-1094OC
11. Fattouh R, Al-Garawi A, Fattouh M, Arias K, Walker TD, Goncharova S, et al. Eosinophils are dispensable for allergic remodeling and immunity in a model of house dust mite-induced airway disease. Am J Respir Crit Care Med. 2011;183(2):179-88. PMid:20732990. http://dx.doi.org/10.1164/rccm.200905-0736OC
12. Cates EC, Fattouh R, Wattie J, Inman MD, Goncharova S, Coyle AJ, et al. Intranasal exposure of mice to house dust mite elicits allergic airway inflammation via a GM-CSF-mediated mechanism. J Immunol. 2004;173(10):6384-92. PMid:15528378.
13. Brewer JM, Conacher M, Hunter CA, Mohrs M, Brombacher F, Alexander J. Aluminium hydroxide adjuvant initiates strong antigen-specific Th2 responses in the absence of IL-4- or IL-13-mediated signaling. J Immunol. 1999;163(12):6448-54. PMid:10586035.
14. Shapiro SD. Animal models of asthma: Pro: Allergic avoidance of animal (model[s]) is not an option. Am J Respir Crit Care Med. 2006;174(11):1171-3. PMid:17110653. http://dx.doi.org/10.1164/rccm.2609001
15. Kool M, Soullié T, van Nimwegen M, Willart MA, Muskens F, Jung S, et al. Alum adjuvant boosts adaptive immunity by inducing uric acid and activating inflammatory dendritic cells. J Exp Med. 2008;205(4):869-82. PMid:18362170 PMCid:2292225. http://dx.doi.org/10.1084/jem.20071087
16. Shi Y, Evans JE, Rock KL. Molecular identification of a danger signal that alerts the immune system to dying cells. Nature. 2003;425(6957):516-21. PMid:14520412. http://dx.doi.org/10.1038/nature01991
17. Clausen SK, Bergqvist M, Poulsen LK, Poulsen OM, Nielsen GD. Development of sensitisation or tolerance following repeated OVA inhalation in BALB/cJ mice. Dose-dependency and modulation by the Al(OH)3 adjuvant. Toxicology. 2003;184(1):51-68. http://dx.doi.org/10.1016/S0300-483X(02)00583-8
18. Van Hove CL, Maes T, Joos GF, Tournoy KG. Prolonged inhaled allergen exposure can induce persistent tolerance. Am J Respir Cell Mol Biol. 2007;36(5):573 84. PMid:17218615. http://dx.doi.org/10.1165/rcmb.2006-0385OC
19. Keller AC, Mucida D, Gomes E, Faquim-Mauro E, Faria AM, Rodriguez D, et al. Hierarchical suppression of asthma-like responses by mucosal tolerance. J Allergy Clin Immunol. 2006;117(2):283-90. PMid:16461128. http://dx.doi.org/10.1016/j.jaci.2005.10.019
20. Holt PG, Reid M, Britten D, Sedgwick J, Bazin H. Suppression of IgE responses by passive antigen inhalation: dissociation of local (mucosal) and systemic immunity. Cell Immunol. 1987;104(2):434-9.
* Study carried out at the Pontifícia Universidade Católica do Rio Grande do Sul - PUCRS, Pontifical Catholic University of Rio Grande do Sul - Porto Alegre, Brazil.
Correspondence to: Andrea M Rodrigues. Centro Infant, Avenida Ipiranga, 6681, Prédio 60 (HSL), 2º andar, Parthenon, CEP 90619‑900, Porto Alegre, RS, Brasil.
Tel. 55 51 3320-3000, extension 2313, or 55 51 3320-3353. E-mail: andream_rodrigues@hotmail.com
Financial support: Andrea Mendonça Rodrigues, Lucien Peroni Gualdi, and Raquel Giacomelli Cao are recipients of doctoral scholarships from the Brazilian Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq, National Council for Scientific and Technological Development). Nailê Karine Nuñez is the recipient of a master's scholarship from CNPq.
Submitted: 26 March 2012. Accepted, after review: 3 August 2012.
About the authorsAndrea Mendonça Rodrigues
Doctoral Student. Graduate Program in Pediatrics and Child Health, Pontifícia Universidade Católica do Rio Grande do Sul - PUCRS, Pontifical Catholic University of Rio Grande do Sul - Porto Alegre, Brazil.
Camila Zanelatto Parreira Schmidt
Pediatric Pulmonologist. Pontifícia Universidade Católica do Rio Grande do Sul - PUCRS, Pontifical Catholic University of Rio Grande do Sul - Porto Alegre, Brazil.
Lucien Peroni Gualdi
Doctoral Student. Graduate Program (Joint Doctoral Program) in Pediatrics and Child Health, Pontifícia Universidade Católica do Rio Grande do Sul - PUCRS, Pontifical Catholic University of Rio Grande do Sul - Porto Alegre, Brazil.
Raquel Giacomelli Cao
Doctoral Student. Graduate Program (Joint Doctoral Program) in Pediatrics and Child Heath, Pontifícia Universidade Católica do Rio Grande do Sul - PUCRS, Pontifical Catholic University of Rio Grande do Sul - Porto Alegre, Brazil.
Rodrigo Godinho de Souza
Technician. Laboratory of Pediatric Pulmonology, Biomedical Research Institute, Pontifícia Universidade Católica do Rio Grande do Sul - PUCRS, Pontifical Catholic University of Rio Grande do Sul - Porto Alegre, Brazil.
Ana Cláudia Pereira
Biology Student. Pontifícia Universidade Católica do Rio Grande do Sul - PUCRS, Pontifical Catholic University of Rio Grande do Sul - Porto Alegre, Brazil.
Nailê Karine Nuñez
Master's Student. Pontifícia Universidade Católica do Rio Grande do Sul - PUCRS, Pontifical Catholic University of Rio Grande do Sul - Porto Alegre, Brazil.
Alisson Passos Schleich
Biology Student. Pontifícia Universidade Católica do Rio Grande do Sul - PUCRS, Pontifical Catholic University of Rio Grande do Sul - Porto Alegre, Brazil.
Paulo Márcio Condessa Pitrez
Professor. Pontifícia Universidade Católica do Rio Grande do Sul - PUCRS, Pontifical Catholic University of Rio Grande do Sul - School of Medicine, Porto Alegre, Brazil.





