ABSTRACT
Malignant neurogenic mediastinal tumors in adults are uncommon and extremely aggressive. We report the case of a 61-year-old male patient with the simultaneous occurrence of malignant mediastinal schwannoma and bronchioloalveolar carcinoma. Although bronchioloalveolar carcinoma is present in 4-7% of the resected synchronous thoracic tumors, this association has never been reported in the literature. However, it is a common finding in patients presenting apparently inflammatory infiltrates and ground-glass opacities, as in the case presented here.
Keywords:
Mediastinal neoplasms; Nerve sheath neoplasms; Neurilemmoma; Neoplasms, multiple primary; Adenocarcinoma, bronchiolo-alveolar.
RESUMO
Tumores neurogênicos malignos do mediastino em adultos são raros e extremamente agressivos. Este artigo relata o caso de um paciente de 61 anos com a ocorrência simultânea de schwannoma maligno de mediastino e carcinoma bronquíolo-alveolar. Apesar do carcinoma bronquíolo-alveolar estar presente em 4-7% dos tumores torácicos sincrônicos ressecados, essa associação nunca foi apresentada na literatura. É, no entanto, um achado frequente em pacientes com infiltrados aparentemente inflamatórios e com opacidades em vidro fosco, como apresentado neste caso.
Palavras-chave:
Neoplasias do mediastino; Neoplasias da bainha neural; Neurilemoma; Neoplasias primárias múltiplas; Adenocarcinoma bronquíolo-alveolar.
IntroduçãoTumores neurogênicos são os mais comuns do mediastino, correspondendo a 20-35% de todas as neoplasias mediastinais.(1,2)
Constituem aproximadamente 75% das lesões do mediastino posterior e, em sua maioria, são benignos e assintomáticos. Quando os sintomas estão presentes, devem levantar a suspeita para uma lesão maligna.(3)
Tumores neurogênicos do mediastino podem originar-se de qualquer estrutura neural contida dentro do tórax, e são classificados de acordo com a sua origem: os derivados das bainhas dos nervos periféricos, os originários do sistema nervoso simpático e aqueles oriundos do sistema nervoso parassimpático. Tumores de origem simpática são classificados em neuroblastomas, ganglioneuroblastomas ou ganglioneuromas.
Tumores de linhagem parassimpática são incomuns e incluem paragangliomas funcionantes (feocromocitomas) e quemodectomas não-secretores.(1)
Dos tumores neurogênicos do mediastino, 40-65% têm sua origem na bainha dos nervos periféricos. Schwannomas (neurilemomas) e neurofibromas, ambas as lesões benignas, constituem mais de 95% dos tumores neste grupo. Os tumores malignos de bainha de nervo periférico (schwannomas malignos) são extremamente agressivos e correspondem aos 2-4% restantes.(2).
Relato de casoUm paciente de 61 anos procurou o setor de emergência de nossa instituição com queixa de dor subescapular há dois meses. Relatava que no início o quadro álgico era tolerável com analgésicos comuns; porém, tornou-se cada vez mais intenso. Não havia nenhum sintoma além da dor, e o paciente negava tosse, rouquidão, febre, calafrios, sudorese noturna, perda ponderal, hemoptise, dispneia e exposição à TB.
Tabagista de 30 anos-maço e etilista social. Negava história familiar de neoplasias.
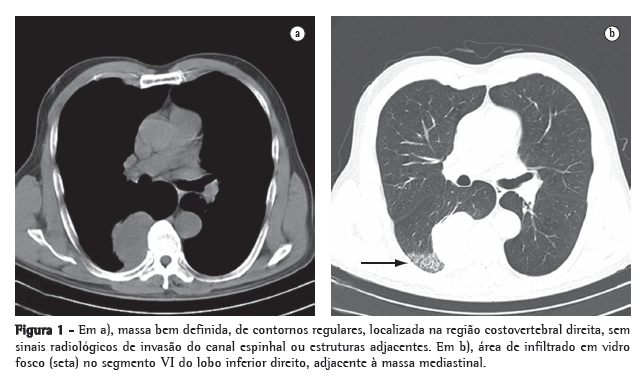
Ao exame físico apresentava-se em bom estado geral e nutricional, e seus sinais vitais eram normais. Sem adenomegalias. A ausculta pulmonar mostrava estertores finos inspiratórios em ambas as bases pulmonares. A ausculta cardíaca era normal. O exame do abdome e dos membros inferiores não revelou alterações. Os resultados do hemograma e testes bioquímicos estavam dentro dos padrões de normalidade. A tomografia computadorizada do tórax (Figura 1a) revelou massa bem definida, de contornos regulares, localizada na região costovertebral direita, medindo 6 × 4,3 cm. Adjacente a massa, observava-se infiltrado pulmonar, aparentemente inflamatório e não-específico.
(Figura 1b)
Foi realizada toracotomia póstero-lateral direita. Observou-se grande massa não-encapsulada, lobulada e densamente aderida à região costovertebral, estendendo-se de T7 a T8 e infiltrando os corpos vertebrais destas vértebras, assim como as cabeças das sétima e oitava costelas. Havia também invasão macroscópica do lobo pulmonar inferior. Foi realizada exérese em bloco do tumor, juntamente com ressecção em cunha do parênquima pulmonar acometido. Não foi possível a ressecção completa da lesão e havia doença residual evidente na região costocondral e no corpo da sétima vértebra.
A análise histopatológica revelou neoplasia de células fusiformes, com extensa necrose, moderado índice mitótico e atipia intensa, compatível com sarcoma de alto grau, provavelmente um tumor maligno de bainha de nervo periférico (Figura 2a). O ensaio imunohistoquímico foi positivo para proteína S-100, confirmando o diagnóstico de schwannoma maligno. Surpreendentemente, no parênquima pulmonar ressecado, foi diagnosticado também carcinoma bronquíolo-alveolar (Figura 2b). A lesão media 2,5 cm em seu maior eixo e comprometia as margens de ressecção. As duas neoplasias estavam separadas por tecido pulmonar sadio, ratificando a origem distinta das lesões.

O paciente recebeu radioterapia adjuvante; porém, nos meses subsequentes, desenvolveu sinais de compressão medular e paralisia flácida e faleceu quatro meses após a operação.
DiscussãoSchwannomas malignos do mediastino constituem aproximadamente 2% dos tumores neurogênicos do mediastino em adultos.(1,2)
Apresentam-se sob a forma de massa à radiografia de tórax e são em sua maioria assintomáticos. Quando produzem sintomas, geralmente se sobressai o quadro álgico.(2) Localizam-se quase que exclusivamente no mediastino posterior e são geralmente grandes, medindo de 6 a 13 cm, com diâmetro médio de 9 cm.(4) Ao exame macroscópico, sua superfície é não-encapsulada, esbranquiçada ou às vezes amarelada e com áreas de hemorragia, necrose ou ambos.(5) São reativos na imunohistoquímica para a proteína S-100 em 50-90% dos casos.(5) Apesar dos mecanismos ainda não terem sido estabelecidos, há crescente evidência de que as proteínas da família S-100 têm grande influência na carcinogênese e gênese de metástases tumorais, interagindo com uma série de outras proteínas e genes, como p53, COX-2 e BRCA1.(6)
Os tumores neurogênicos malignos do mediastino são extremamente agressivos e associados à baixa sobrevida em 5 anos. Invasão local, metástases hematogênicas e pulmonares ocorrem com frequência.(2)
Recorrência local é habitual.(3) Os achados em tomografia computadorizada sugestivos de malignidade são os seguintes: (1) áreas de baixa densidade; (2) compressão de estruturas adjacentes; (3)
anormalidades pleurais, como efusão pleural ou nódulos pleurais; e (4) nódulos pulmonares metastáticos.(4) A erosão de estruturas ósseas e dor não são achados incomuns e também sugerem malignidade.(5) A ressecção cirúrgica radical com margens amplas é o tratamento de escolha. Quando a ressecção completa não for factível, a excisão simples sem margens amplas ou a excisão subtotal seguida de radioterapia em altas doses são alternativas possíveis.(3) Radioterapia e quimioterapia adjuvantes não parecem aumentar a sobrevida, mas tem utilidade no tratamento da doença metastática.(3) A cura cirúrgica é raramente possível.(1)
A ocorrência simultânea de schwannoma maligno de mediastino e carcinoma bronquíolo-alveolar é inédita. Neoplasias torácicas múltiplas constituem aproximadamente 4% de todas as ressecções por câncer de pulmão, e grande parte dos casos ocorre entre a sexta e a sétima década de vida.(7) A gênese dos tumores sincrônicos pode ser atribuída a fatores oncogênicos intrínsecos ao indivíduo ou estar relacionada a um fenômeno fortuito.(7) De acordo com dois autores,(8) tumores torácicos sincrônicos devem ser diagnosticados simultaneamente com a lesão índice, ser interpostos por parênquima pulmonar sadio e não compartilhar drenagem linfática. Características histopatológicas, morfologia, localização, invasão vascular e análise imunohistoquímica também devem ser levadas em consideração na diferenciação dos tumores.(9) A histologia diferente em neoplasias claramente distintas é patognomônico da natureza primária das lesões. No entanto, isto ocorre em apenas 10-15% dos casos.(7,10)
Áreas de opacidade em vidro fosco em tomografia de tórax são achados inespecíficos e podem representar diversas condições, como edema pulmonar, proteinose alveolar, alveolites, pneumonites intersticiais e neoplasias.(11) O diagnóstico de neoplasia em infiltrado pulmonar em vidro fosco, como neste caso, não é raro. Alguns autores(11) avaliaram 20 casos de infiltrados em vidro fosco submetidos à ressecção cirúrgica. Destes, 50% foram diagnosticados como carcinoma bronquíolo-alveolar, 10% como adenocarcinomas e 25% como hiperplasia adenomatosa atípica, lesão considerada precursora de carcinoma bronquíolo-alveolar.
Apesar de ser a neoplasia maligna mais comum do sistema nervoso periférico, o schwannoma maligno continua sendo um dos sarcomas menos estudados. A sobrevida em 5 anos é baixa e negativamente afetada pelo tamanho da lesão, ressecção incompleta e associação com doença de Von Recklinghausen.(3) A ressecção completa geralmente não é possível, e radioterapia e quimioterapia adjuvantes podem ter utilidade no tratamento da doença metastática. Pela raridade da lesão e a quase inexistência de sintomas, deve-se ter um alto grau de suspeição clínica para corretamente diagnosticar esta rara neoplasia. A associação de schwannoma maligno e carcinoma bronquíolo-alveolar provavelmente se deu por fenômeno fortuito e não influenciou o desfecho do caso, que foi consequência da natureza agressiva da lesão mediastinal. No entanto, a presença de neoplasia deve ser sempre suspeitada em infiltrados pulmonares em vidro fosco localizados que não desapareçam ou que aumentem. Convém nestes casos uma abordagem agressiva, com biópsia precoce e análise histopatológica.
Referências 1. Teixeira JP, Bibas RA. Surgical treatment of tumors of the mediastinum: the Brazilian experience. In: Martini N, Vogt-Moykopf I, editors. Thoracic surgery: Frontiers and uncommon neoplasms. International trends in general thoracic surgery. St. Louis: Mosby; 1989. p.211-225.
2. Wain JC. Neurogenic tumors of the mediastinum. Chest Surg Clin North Am. 1992;2:121-36.
3. Macchiarini P, Ostertag H. Uncommon primary mediastinal tumours. Lancet Oncol. 2004;5(2):107-18.
4. Moon WK, Im JG, Han MC. Malignant schwannomas of the thorax: CT findings. J Comput Assist Tomogr. 1993;17(2):274-6.
5. Shields TW. Benign and malignant neurogenic tumors of the mediastinum in adults. In: Shields TW, LoCicero III J, Ponn RB, editors. General Thoracic Surgery. Philadelphia: Lippincott Williams &Wilkins; 2000. p. 2313-2327.
6. Salama I, Malone PS, Mihaimeed F, Jones JL. A review of the S100 proteins in cancer. Eur J Surg Oncol. 2008;34(4):357-64.
7. Rostad H, Strand TE, Naalsund A, Norstein J. Resected synchronous primary malignant lung tumors: a population-based study. Ann Thorac Surg. 2008;85(1):204-9.
8. Martini N, Melamed MR. Multiple primary lung cancers. J Thorac Cardiovasc Surg. 1975;70(4):606-12.
9. Chang YL, Wu CT, Lee YC. Surgical treatment of synchronous multiple primary lung cancers: experience of 92 patients. J Thorac Cardiovasc Surg. 2007;134(3):630-7. Erratum in: J Thorac Cardiovasc Surg. 2008;136(2):542.
10. Trousse D, Barlesi F, Loundou A, Tasei AM, Doddoli C, Giudicelli R, et al. Synchronous multiple primary lung cancer: an increasing clinical occurrence requiring multidisciplinary management. J Thorac Cardiovasc Surg. 2007;133(5):1193-200.
11. Nakajima R, Yokose T, Kakinuma R, Nagai K, Nishiwaki Y, Ochiai A. Localized pure ground-glass opacity on high-resolution CT: histologic characteristics. J Comput Assist Tomogr. 2002;26(3):323-9.
Sobre os autores
Benoit Jacques Bibas
Residente em Cirurgia Geral. Hospital Central da Polícia Militar do Rio de Janeiro - HCPM - Rio de Janeiro (RJ) Brasil.
Marcos Madeira
Capitão Médico do Serviço de Cirurgia Torácica. Hospital Central da Polícia Militar do Rio de Janeiro - HCPM - Rio de Janeiro (RJ) Brasil.
Rodrigo Gavina
Capitão Médico do Serviço de Cirurgia Torácica. Hospital Central da Polícia Militar do Rio de Janeiro - HCPM - Rio de Janeiro (RJ) Brasil.
Leonardo Hoehl-Carneiro
Tenente Médico do Serviço de Anatomia Patológica. Hospital Central da Polícia Militar do Rio de Janeiro - HCPM - Rio de Janeiro (RJ) Brasil.
Sergio Sardinha
Tenente Coronel Médico do Serviço de Cirurgia Torácica. Hospital Central da Polícia Militar do Rio de Janeiro - HCPM - Rio de Janeiro (RJ) Brasil.
Trabalho realizado no Hospital Central da Polícia Militar do Rio de Janeiro - HCPM - Rio de Janeiro (RJ) Brasil.
Endereço para correspondência: Benoit Jacques Bibas. Av. Epitácio Pessoa, 3350, apto. 201, Lagoa, CEP 22471-001, Rio de Janeiro, RJ, Brasil.
Tel 55 21 2539-0994. E-mail: bjbibas@click21.com.br
Apoio financeiro: Nenhum.
Recebido para publicação em 29/12/2007. Aprovado, após revisão em 13/5/2008.



