ABSTRACT
The objective of this study was to assess the efficacy of exercise training by means of a rehabilitative walking protocol. Twenty patients with COPD staged as III/IV according to the Global Initiative for Chronic Obstructive Lung Disease were included. Patients were evaluated at baseline and at the end of the exercise program regarding oxygen desaturation, sensation of dyspnea/fatigue, quality of life and six-minute walk distance. The comparison between the six-minute walk distance prior to and after training proved the efficacy of the protocol, which also resulted in a decrease in oxygen desaturation and in the sensation of dyspnea. This protocol can be easily put into practice.
Keywords:
Activities of daily living; Pulmonary disease, chronic obstructive; Rehabilitation; Exercise therapy; Exercise test.
RESUMO
O objetivo deste estudo foi avaliar a eficácia do treinamento de exercício com protocolo de marcha. Foram incluídos 20 doentes com DPOC em estádios III/IV segundo Global Initiative for Chronic Obstructive Lung Disease. Os pacientes foram avaliados no início e ao final do programa de exercício quanto à dessaturação de oxigênio, sensação de dispneia/fadiga, qualidade de vida e distância percorrida no teste da caminhada de seis minutos. O efeito de treinamento evidenciou-se na comparação das distâncias percorridas antes e após o treinamento, com diminuição da dessaturação para maiores distâncias e na sensação de dispneia. Esse programa de treinamento é facilmente exequível.
Palavras-chave:
Atividades cotidianas; Doença pulmonar obstrutiva crônica; Reabilitação; Terapia por exercício; Teste de esforço.
It is currently acknowledged that COPD patients present a decrease in exercise tolerance and dyspnea, and this phenomenon is essentially due to airway obstruction, to peripheral muscle dysfunction and presumably to a combination of various other factors (deconditioning, wasting, hypoxemia, hypercapnia, oxidative stress and apoptosis).(1-6) The Body mass index, airway Obstruction, Dyspnea, and Exercise capacity (BODE) index takes into consideration the following: body mass index; airway obstruction-as determined by measuring FEV1; the perception of dyspnea-as determined by the Modified Medical Research Council (MMRC) dyspnea scale; and exercise capacity-as determined with the six-minute walk test.(7) This index characterizes the multisystemic disease, considering not only the FEV1, which has currently shown not to be strongly correlated with the daily amount of physical activity or the degree of dyspnea. The BODE index has proven to be a reliable indicator of survival in COPD patients.(7)
Exercise training (ET) promotes better tolerance to exercise and improvement of the quality of life of these patients.(8) Currently, ET is recognized as an essential trend in pulmonary rehabilitation,(9) and a program of pulmonary rehabilitation has short- and long-term benefits, as has been demonstrated.(10) However, there is no consensus regarding the most appropriate training strategy for those patients; nor is there agreement regarding the appropriate duration, intensity and frequency of the individual training sessions.(9,11) The most frequently used modalities are walking and cycling.
The objective of this prospective analysis was to assess the efficacy of ET, using a rehabilitative walking protocol, in relation to the impact on quality of life and exercise capacity in COPD patients.
We included in the protocol 20 patients with clinically stable COPD (stages III/IV of the Global Initiative for Chronic Obstructive Lung Disease), all of whom were former smokers. The mean value of the BODE index of this group of patients prior to ET was 4 (range, 2-6).
The protocol consisted of walking training three times per week, during a period of 20 min, over two months (total of 20 sessions). The methodology was based on the determination of the highest maximum HR attained in the two initial six-minute walk tests, 80% of this HR value being established as the standard for training.
The ET was carried out in a 30-m long open-air covered walkway, supervised by a nurse specialized in pulmonary rehabilitation, with continuous electronic monitoring of HR and SpO2. The six-minute walk distances were recorded after each ET session, whereas SpO2 and HR were recorded before and after each ET session.
The patients were evaluated at baseline (T0) and at the end of the ET program (T1) using the following parameters: oxygen desaturation; sensation of dyspnea-as evaluated with the MMRC and Borg scales; sensation of fatigue of the lower limbs-as determined with the Borg scale; quality of life-as evaluated with the St. George's Respiratory Questionnaire (SGRQ); six-minute walk distance; plethysmography results at T0; spirometry values at T1; and arterial blood gas exchange.
All patients were submitted to one set of two six-minute walk tests before the ET program and another set of two six-minute walk tests after the ET program. These tests were conducted in accordance with the current recommendations,(12) in a 30-m covered walkway.
All respiratory function tests were conducted in the Laboratory of Respiratory Pathophysiology of the Vila Nova de Gaia/Espinho Hospital, located in the city of Porto, Portugal.
The statistical analysis of the data was performed using the Statistical Package for the Social Sciences, version 11.5 (SPSS Inc., Chicago, IL, USA). For all of the associations and correlations considered, the level of statistical significance was set at p < 0.05.
All the patients included were male, with mean age of 68 years (range, 51-80 years). They presented a mean body mass index of 25 kg/m² (range, 18-35 kg/m²). All patients presented pulmonary inflation. The mean value of FEV1 was 0.984 L (39% of predicted), with a minimum value of 0.34 L (15% of predicted). Six patients (37.5%) presented heart disease, including valve failure (in 5), pulmonary hypertension (in 2) and left heart failure (in 1; left ventricular ejection fraction < 35%). None of the patients used home oxygen therapy or home noninvasive ventilation.
Sixteen patients (80.0%) finished the ET program, as follows:
3 were excluded due to exacerbation of the COPD in the context of respiratory infection and 1 due to cerebrovascular accident; this patient had severe arteriosclerotic disease. There were no other occurrences during the ET program.
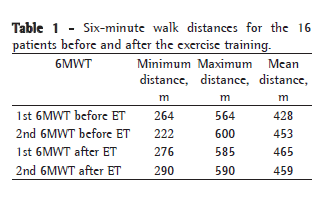
All six-minute walk distances are discriminated in Table 1.
The difference between the mean pre-ET and post-ET six-minute walk distances on the two six-minute walk tests (best of the two) was 10 m (458 m vs. 468 m; p = 0.301), as shown in Table 1.
The mean six-minute walk distance in the three sessions in the first week of ET was 1,435 m (range, 752-1,886 m), compared with 1,520 m (range, 800-1,920 m) in the last week of ET, a statistically significant difference of 85 m (p = 0.013).
The mean pre-ET and post-ET values obtained for the sensation of dyspnea with the Borg scale after the two six-minute walk tests (best of the two) were, respectively, 2.5 and 1.4 (p = 0.049). Regarding fatigue in the lower limbs according to the Borg scale, no statistically significant difference was observed between the pre-ET and post-ET values on the best six-minute walk test (1.1 and 1.5, respectively; p = 0.308).
The mean pre-ET and post-ET times to recovery after the performance of the six-minute walk tests were 75 s and 72.5 s, respectively.
The mean pre-ET and post-ET scores on the MMRC scale were,
respectively, 2.6 and 2.3, with a statistically significant difference of 0.3 (p = 0.025). In the evaluation of the self-perception of health, 5 patients (31.3%) reported obvious improvement (from moderate health status to good or very good health status). The mean scores obtained for the symptoms and activity domains of the SGRQ presented no statistical significance between T0 and T1 (symptom: 40.1 vs. 34.6; p = 0.352; activity: 58.0 vs. 54.0; p = 0.211). However, in the comparison of the mean scores, a clinically significant difference of four points was observed for these domains.
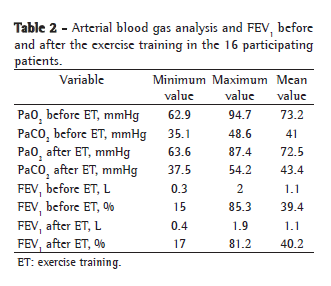
No significant differences were observed between T0 and T1 in terms of the results of the arterial blood gas analysis-PaO2 (p = 0.875) and PaCO2 (p = 0.99)-or in the FEV1 in L and % of predicted (p = 0.756: Table 2).
The mean HR after the two best six-minute walk tests presented a slight reduction between T0 and T1 (from 109 bpm to 107 bpm), as did the weekly mean HR during the ET sessions, which fell from 103 bpm in the first week to 101 bpm in the final week.
The mean value of the BODE index at T1 was 3.6 (a reduction of 0.4 in relation to T0).
A tendency toward a decrease in the oxygen desaturation for longer six-minute walk distances over several weeks of training was also observed.
In the interpretation of these results, it is necessary to take into consideration the size of the sample (only 16 patients completed the study). No significant (> 10-m) differences were observed in the post-ET six-minute walk distance. Sinces the mean value of the initial six-minute walk test was already high (> 450 m), the reduction in HR after the ET program, even if slight, can translate to better final performance.
This exercise training protocol with walking resulted in an improvement in quality of life and exercise capacity. In accordance with previous reports in the literature,(4,13) there was no significant alteration of the obstruction. Therefore, this improvement might be explained by the decrease in pulmonary inflation, although that parameter was not evaluated after the ET program.
Even in this context, the authors believe this to be an efficacious exercise training protocol in COPD. It is simple and easily put into practice, since walking is a physiological and natural activity in "real life". This protocol might correspond to good adherence on the part of the patients and, certainly, will be a stimulus to continuity of the "training" at home.
References 1. Saey D, Michaud A, Couillard A, Côté CH, Mador MJ, LeBlanc P, et al. Contractile fatigue, muscle morphometry, and blood lactate in chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2005;171(10):1109-15.
2. Man WD, Soliman MG, Nikoletou D, Harris ML, Rafferty GF, Mustfa N, et al. Non-volitional assessment of skeletal muscle strength in patients with chronic obstructive pulmonary disease. Thorax. 2003;58(8):665-9.
3. Wagner PD. Skeletal muscles in chronic obstructive pulmonary disease: deconditioning, or myopathy? Respirology. 2006;11(6):681-6.
4. Skeletal muscle dysfunction in chronic obstructive pulmonary disease. A statement of the American Thoracic Society and European Respiratory Society. Am J Respir Crit Care Med. 1999;159(4 Pt 2):S1-40.
5. Sin DD, Man SF. Skeletal muscle weakness, reduced exercise tolerance, and COPD: is systemic inflammation the missing link? Thorax. 2006;61(1):1-3.
6. Debigaré R, Marquis K, Côté CH, Tremblay RR, Michaud A, LeBlanc P, et al. Catabolic/anabolic balance and muscle wasting in patients with COPD. Chest. 2003;124(1):83-9.
7. Celli BR, Cote CG, Marin JM, Casanova C, Montes de Oca M, Mendez RA, et al. The body-mass index, airflow obstruction, dyspnea, and exercise capacity index in chronic obstructive pulmonary disease. N Engl J Med. 2004;350(10):1005-12.
8. Lacasse Y, Wong E, Guyatt GH, King D, Cook DJ, Goldstein RS. Meta-analysis of respiratory rehabilitation in chronic obstructive pulmonary disease. Lancet. 1996;348(9035):1115-9.
9. Pulmonary rehabilitation-1999. American Thoracic Society. Am J Respir Crit Care Med. 1999;159(5 Pt 1):1666-82.
10. Godoy RF, Teixeira PJ, Becker Júnior B, Michelli M, Godoy DV. Long-term repercussions of a pulmonary rehabilitation program on the indices of anxiety, depression, quality of life and physical performance in patients with COPD. J Bras Pneumol. 2009;35(2):129‑36.
11. O'Shea SD, Taylor NF, Paratz J. Peripheral muscle strength training in COPD: a systematic review. Chest. 2004;126(3):903-14.
12. ATS Committee on Proficiency Standards for Clinical Pulmonary Function Laboratories. ATS statement: guidelines for the six-minute walk test. Am J Respir Crit Care Med. 2002;166(1):111-7.
13. Moreira MA, Moraes MR, Tannus R. Teste da caminhada de seis minutos em pacientes com DPOC durante programa de reabilitação. J Pneumol. 2001;27(6):295‑300.
Study carried out in the Pulmonary Rehabilitation Unit of the Vila Nova de Gaia/Espinho Hospital, Porto, Portugal.
Correspondence to: Susana Alves Ferreira. Centro Hospitalar de Vila Nova de Gaia/Espinho EPE, Rua Conceição Fernandes s/n, Vilar de Andorinho, 4430-502, Vila Nova de Gaia, Portugal.
Tel 351 227 865 100. E-mail: susalvesferreira@gmail.com
Financial support: None
Submitted: 3 February 2009. Accepted, after review: 2 July 2009.
About the authorsSusana Alves Ferreira
Assistant Intern in the Department of Pulmonology. Vila Nova de Gaia/Espinho Hospital, Porto, Portugal.
Miguel Guimarães
Attending Physician in the Department of Pulmonology. Vila Nova de Gaia/Espinho Hospital, Porto, Portugal.
Natália Taveira
Attending Physician in the Department of Pulmonology. Vila Nova de Gaia/Espinho Hospital, Porto, Portugal.



