ABSTRACT
Objective: To evaluate respiratory muscle strength and six-minute walk test (6MWT) variables in patients with uncontrolled severe asthma (UCSA). Methods: This was a cross-sectional study involving UCSA patients followed at a university hospital. The patients underwent 6MWT, spirometry, and measurements of respiratory muscle strength, as well as completing the Asthma Control Test (ACT). The Mann-Whitney test was used in order to analyze 6MWT variables, whereas the Kruskal-Wallis test was used to determine whether there was an association between the use of oral corticosteroids and respiratory muscle strength. Results: We included 25 patients. Mean FEV1 was 58.8 21.8% of predicted, and mean ACT score was 14.0 3.9 points. No significant difference was found between the median six-minute walk distance recorded for the UCSA patients and that predicted for healthy Brazilians (512 m and 534 m, respectively; p = 0.14). During the 6MWT, there was no significant drop in SpO2. Mean MIP and MEP were normal (72.9 15.2% and 67.6 22.2%, respectively). Comparing the patients treated with at least four courses of oral corticosteroids per year and those treated with three or fewer, we found no significant differences in MIP (p = 0.15) or MEP (p = 0.45). Conclusions: Our findings suggest that UCSA patients are similar to normal subjects in terms of 6MWT variables and respiratory muscle strength. The use of oral corticosteroids has no apparent impact on respiratory muscle strength.
RESUMO
Objetivo: Avaliar a força muscular respiratória e variáveis obtidas no teste de caminhada de seis minutos (TC6) em pacientes com asma grave não controlada (AGNC). Métodos: Estudo transversal, envolvendo pacientes com AGNC acompanhados em um hospital universitário. Os pacientes foram submetidos a TC6, espirometria e medidas da força muscular respiratória e responderam o Asthma Control Test (ACT, Teste de Controle da Asma). O teste de Mann-Whitney foi utilizado na análise das variáveis do TC6, e o teste de Kruskal-Wallis foi utilizado na verificação de uma possível associação do uso de corticoide oral com a força muscular respiratória. Resultados: Foram incluídos 25 pacientes, com médias de VEF1 de 58,8 21,8% do previsto e escore do ACT de 14,0 3,9 pontos. Não houve diferença significativa entre a mediana da distância percorrida no TC6 dos pacientes com AGNC e aquela prevista para brasileiros saudáveis (512 m e 534 m, respectivamente; p = 0,14). Durante o TC6, não houve queda significativa da SpO2. As médias de PImáx e PEmáx foram normais (72,9 15,2% e 67,6 22,2%, respectivamente). Não houve diferenças significativas nas medidas de PImáx (p = 0,15) e PEmáx (p = 0,45) entre os pacientes que usavam ao menos quatro ciclos de corticoide oral por ano e os que o usavam por três ou menos ciclos por ano. Conclusões: Nossos achados sugerem que os pacientes com AGNC são semelhantes a indivíduos normais em termos das variáveis do TC6 e da força muscular respiratória. Não se observou um impacto do uso de corticoide oral na força muscular respiratória.
Palavras-chave:
Asma; Tolerância ao exercício; Músculos respiratórios.
IntroduçãoA asma é uma doença inflamatória crônica das vias aéreas, caracterizada por hiper-reatividade brônquica, limitação variável do fluxo aéreo e sintomas, como dispneia, chiado e tosse, que melhoram espontaneamente ou com tratamento. Os objetivos básicos do manejo da asma são o controle total dos sintomas e das limitações das atividades diárias e a redução dos riscos futuros. (1,2) A maioria dos pacientes tem asma leve ou moderada, facilmente controladas com o uso de corticoides por via inalatória (CI) de forma isolada ou associados com long-acting 2 agonist (LABA, 2-agonista de longa duração).(3) Entretanto, entre os asmáticos graves, há um pequeno subgrupo de pacientes que permanecem sintomáticos apesar de boa adesão ao tratamento, uso correto dos dispositivos, manejo adequado de comorbidades e uso de altas dosagens de CI associados com LABA e/ou corticoide oral e/ou omalizumabe.(4,5) Esta condição particular é denominada asma grave não controlada (AGNC), a qual, segundo as diretrizes atuais de asma, deve ser tratada em serviços especializados.(4,5)
Pacientes com AGNC necessitam de altas doses de CI associados ou não a corticoides orais, os quais têm, entre seus efeitos adversos, a redução da síntese de proteínas e o aumento de sua degradação, efeitos esses que contribuem para a atrofia muscular.(6) Adicionalmente, o aumento da resistência das vias aéreas e da hiperinsuflação pulmonar também contribuem para a redução da eficiência de músculos inspiratórios, resultando em maior trabalho muscular e maior gasto energético para vencer a limitação ao fluxo aéreo.(7) Esses fatores ainda não foram bem estudados na AGNC.
O teste de caminhada de seis minutos (TC6) é um teste submáximo que provê uma avaliação da resposta global e integrada de todos os aspectos corporais envolvidos na realização do exercício (sistema pulmonar, sistema cardiovascular, circulação sistêmica e periférica, sangue, unidade neuromuscular e metabolismo muscular).(8,9) Já a força muscular respiratória pode ser estimada a partir das pressões geradas nas vias aéreas pela contração dos músculos respiratórios. As pressões respiratórias estáticas máximas são habitualmente medidas ao nível da boca na inspiração (PImáx) e na expiração (PEmáx).(10)
O papel do TC6 na avaliação e no acompanhamento de pacientes com DPOC, doença intersticial pulmonar, hipertensão arterial pulmonar e insuficiência cardíaca está bem estabelecido.(8) No entanto, em adultos, o impacto do comprometimento na asma grave foi avaliado apenas em um estudo de Canuto et al.,(11) que verificaram uma distância percorrida no TC6 (DTC6) significativamente menor nos pacientes com asma de difícil controle (ADC), em uso de corticoide oral, quando comparados com indivíduos saudáveis do grupo controle. Por outro lado, embora a redução da força muscular, principalmente da PImáx, tenha sido descrita em vários estudos com pacientes asmáticos, a mesma ainda não foi avaliada no grupo de pacientes com AGNC.(12)
O objetivo principal do presente estudo foi investigar o comportamento das variáveis do TC6, assim como PImáx e PEmáx, em pacientes com AGNC. De forma secundária, objetivamos investigar o impacto do uso de corticoide oral na força muscular respiratória e a correlação do nível de atividade física dos pacientes com a DTC6 e o nível de controle da asma.
MétodosTrata-se de estudo transversal que incluiu pacientes maiores de 18 anos com asma grave acompanhados no Ambulatório de Asma de Difícil Controle do Hospital das Clínicas da Universidade Federal de Minas Gerais (UFMG), em Belo Horizonte (MG), no período entre setembro e dezembro de 2012. O projeto foi aprovado pelo Comitê de Ética em Pesquisa da UFMG (parecer ETIC nº 156.403/2012). Todos os participantes assinaram o termo de consentimento livre e esclarecido.
O diagnóstico de asma grave baseou-se nos critérios da American Thoracic Society/European Respiratory Society (ATS/ERS),(13) assim definidos: como critérios maiores, uso de corticoide oral por no mínimo seis meses no ano e uso contínuo de CI em doses elevadas (≥ 1.600 µg de budesonida ou equivalente) associado a LABA; como critérios menores, VEF1 < 80%; variabilidade do PFE > 20%; uso diário de 2-agonista de curta duração; uso de mais de três cursos de corticoide oral no ano; história de episódio de asma quase fatal; uma ou mais consultas em serviços de urgência no ano anterior; e deterioração rápida da função pulmonar ao diminuir a dose do tratamento com corticoide.
Os pacientes incluídos tiveram acompanhamento ambulatorial por, no mínimo, seis meses, visando o controle de fatores ambientais e de comorbidades, a melhora da técnica de uso dos dispositivos inalatórios e o aumento da adesão ao tratamento. Além disso, foram incluídos apenas os pacientes nas etapas 4 e 5 de tratamento da asma (LABA/CI em dose elevada mais corticoide oral e/ou anti-IgE) segundo as diretrizes da Global Initiative for Asthma (GINA)(1) e da Sociedade Brasileira de Pneumologia e Tisiologia (SBPT),(2) e com dois critérios maiores ou um critério maior e dois menores dos critérios da ATS/ERS.(13) Foram excluídos os pacientes com cardiopatia grave; fumantes ativos; ex-fumantes com carga tabágica ≥ 10 maços-ano ou que cessaram tabagismo há menos de um ano; e pacientes que tiveram exacerbação necessitando de atendimento em pronto-socorro/internação, uso de prednisona ou equivalente acima de 20 mg e/ou de antibióticos nas últimas quatro semanas.
O TC6 foi realizado em um corredor de 25,6 m utilizando um oxímetro portátil (Nonin Medical, Inc., Plymouth, MN, EUA), seguindo as recomendações da ATS.(14) Todos os pacientes fizeram dois TC6, com um intervalo mínimo de 30 min entre eles. Foram avaliados os seguintes parâmetros: SpO2 medida por oximetria de pulso, FC, FR, e percepção da intensidade de dispneia e de fadiga nos membros inferiores pela escala de Borg ao início e ao final dos testes. Foram verificados também o valor percentual da FC em relação à FC máxima prevista para adultos (%FCmáx), a FC de recuperação no primeiro minuto após o término do teste (FCR1) e a DTC6. Foram considerados significativos valores de dessaturação ≥ 4%,(8,14) %FCmáx > 85% do previsto(8,14) e FCR1 > 12 bpm.(15-17) Considerou-se válido o TC6 com o maior valor para DTC6; os valores absolutos e percentuais do previsto para a DTC6 foram calculados através da equação de referência para TC6 da população brasileira.(18)
A espirometria foi realizada utilizando um espirômetro da marca Koko (PDS Instrumentation Inc., Louisville, CO, EUA). A execução e a interpretação dos testes ocorreram segundo as diretrizes da SBPT.(10) Os valores encontrados no teste pós-broncodilatador foram relatados como valores absolutos e percentuais em relação aos valores previstos de acordo com Pereira et al.(19)
A força dos músculos respiratórios foi avaliada através de um manovacuômetro digital (Warren E Collins Inc., Braintree, MA, EUA) seguindo as diretrizes nacionais da SBPT,(10) com leitura e armazenamento dos sinais através de ductos individuais. Um orifício de 2 mm no circuito impedia falsas medidas por contração involuntária das bochechas. A PImáx foi mensurada ao nível do VR, e a PEmáx foi mensurada ao nível da CPT. Os resultados foram expressos em cmH2O.(20)
O nível de controle da asma foi avaliado através do Asthma Control Test (ACT, teste de controle da asma), no qual 25 pontos representam remissão clínica dos sintomas ou controle total da asma; de 20 a 24 pontos, controle adequado da doença; e abaixo de 20 pontos, asma não controlada; foi utilizada a versão validada para uso no Brasil.(21-23)
O nível de atividade física foi medido de acordo com International Physical Activity Questionnaire (IPAQ, Questionário Internacional de Atividade Física), versão curta, validado para uso no Brasil.(24,25) O instrumento contém sete questões relacionadas à frequência, em dias por semana, e à duração, em minutos por dia, das atividades físicas vigorosas, moderadas e de caminhada. O escore classifica os indivíduos em muito ativo, ativo, irregularmente ativo e sedentário. Agrupamos as classificações em dois grupos: muito ativo ou ativo e irregularmente ativo ou sedentário.(24,25)
Todos os pacientes do estudo realizaram TCAR de tórax para o diagnóstico diferencial de outras doenças associadas, como DPOC, bronquiectasias e aspergilose broncopulmonar alérgica.
A análise dos dados foi realizada no Statistical Package for the Social Sciences, versão 18 (SPSS Inc., Chicago, IL, EUA) e Minitab, versão 16 (Minitab Inc., State College, MA, EUA). O teste de Shapiro-Wilk foi utilizado para avaliar a distribuição dos dados. As variáveis categóricas foram apresentadas em frequência e proporção, e as variáveis contínuas foram expressas como média e desvio-padrão (distribuição paramétrica) ou como mediana e variação (distribuição não paramétrica). Para avaliar a diferença entre a DTC6 nos pacientes com AGNC e o valor previsto da DTC6 em indivíduos normais, assim como para verificar a associação da prática de atividade física (IPAQ) com as variáveis DTC6, escore do ACT, %FCmáx e FCR1, foi utilizado o teste de Mann-Whitney. A possível associação entre o uso de corticoide oral com PImáx e PEmáx foi avaliada através do teste de correlação de Spearman e teste de Kruskal-Wallis. Foram considerados estatisticamente significativos os valores de p < 0,05. Com base na maior DTC6 encontrada na literatura, considerando-se um desvio-padrão de 90,44 m, nível de significância de 0,05, usando-se o teste t de Student bicaudal para uma amostra única, o tamanho da amostra foi estimado em 26 pacientes para se verificar uma diferença de 50 m na DTC6 em relação à literatura.(26)
ResultadosA amostra inicial consistiu de 29 pacientes. Três indivíduos foram excluídos por se tratarem de pacientes com provável síndrome de sobreposição asma/DPOC, e outro foi excluído devido a exacerbação da asma durante o mês da coleta dos dados.
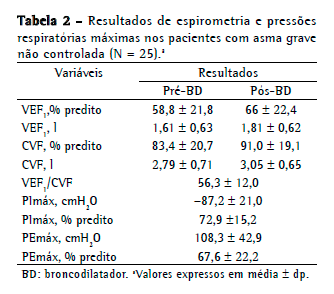
Participaram 25 pacientes asmáticos (18 do sexo feminino e 7 do sexo masculino), com média de idade de 49 anos e média de índice de massa corpórea de 28,9 7,9 kg/m2 (Tabela 1). Todos os pacientes apresentaram escores do ACT < 15 pontos, 14 pacientes (56%) eram irregularmente ativos/sedentários, e 20 (80%) tinham limitações para exercícios no período intercrise. Dez pacientes (40%) tinham história de exacerbação com internação em terapia intensiva, e 7 (28%), com necessidade de ventilação mecânica.

Todos os pacientes estavam em uso de LABA e dose alta de CI (≥ 1.600 µg de budesonida ou equivalente), 6 (24%) usavam pelo menos 10 mg/dia de prednisona há mais de um ano, e 3 (12%) utilizavam omalizumabe.
As principais alterações tomográficas foram bronquiectasias mínimas/moderadas com predomínio central, em 3 pacientes; pequenas áreas de enfisema centrolobular, em 11; fibroatelectasia discreta do lobo superior direito, em 1; e aprisionamento aéreo, em 1.
Houve predomínio de distúrbio ventilatório obstrutivo com média de VEF1 de 58,8 21,8% do previsto, e 17 pacientes (68%) tiveram prova broncodilatadora positiva. As médias da PImáx e PEmáx foram normais; entretanto, 7 (28%) e 11 (44%) dos pacientes apresentaram PImáx e PEmáx reduzidas (< 65% do previsto), respectivamente (Tabela 2). Dos 7 pacientes que tinham PImáx reduzidas, somente 2 apresentaram sinais espirométricos de hiperinsuflação pulmonar.
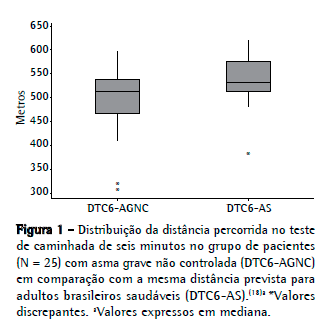
Não houve diferença significativa (p = 0,14) entre os valores medianos da DTC6 - 512 m (variação: 307,2-597,3 m) - e da DTC6 prevista para indivíduos normais - 534 m (variação: 382,6-621,3 m) - (Figura 1).
Nenhum paciente utilizou oxigênio suplementar e não houve queda da SpO2 média durante o TC6; porém, 5 pacientes apresentaram dessaturação durante o mesmo. Dentre esses, 2 apresentaram broncoespasmo, que foi revertido com a utilização de 2-agonista de curta duração, 2 tinham comorbidades (aspergilose broncopulmonar alérgica e sequela de tuberculose pulmonar), e 1 apresentara enfisema e aprisionamento aéreo na TC de tórax. Ao final do TC6, a intensidade da percepção da fadiga de membros inferiores foi leve e a de dispneia foi de leve a moderada. Os pacientes apresentaram uma queda significativa da FCR1 (Tabela 3).

Ao compararmos o subgrupo de pacientes em uso continuo de corticoide oral ou com quatro ou mais ciclos por ano (n = 15) com o subgrupo de pacientes com três ou menos ciclos por ano (n = 10) a fim de investigar a associação entre a frequência de uso de corticoide oral e a força muscular respiratória, não encontramos diferenças estatisticamente significativas entre os valores medianos de PImáx - 74,5% (variação: 59,0-104,0%) e 72,5% (variação: 43,0-104,0%; p = 0,15), respectivamente - e PEmáx - 67,5% (variação: 29,0-121,0%) e 63,5% (variação: 34,0-121,0%; p = 0,45), respectivamente.
Os 11 pacientes mais ativos fisicamente e os 14 menos ativos apresentaram resultados semelhantes em relação a ACT, DTC6, FCR1 e %FCmáx no TC6 (Tabela 4).
 Discussão
DiscussãoHistoricamente, os pacientes que não atingem o controle da asma, apesar do tratamento nas etapas 4 ou 5 segundo o GINA, são classificados como portadores de ADC.(1) Entretanto, há mais de duas décadas persistem muitas discussões sobre a terminologia mais apropriada devido aos diferentes critérios de definição utilizados para asma grave, ADC, asma refratária ou resistente ao tratamento e, mais recentemente, AGNC.
Em 2000, uma publicação da ATS sugeriu critérios de definição de ADC, que ajudaram a reduzir parte dessas controvérsias.(13) No entanto, somente após a publicação da força tarefa da ATS/ERS em 2013, ratificada e citada na diretriz GINA de 2014, é que essa classificação tornou-se mais clara.(4,5)
De acordo com aquelas publicações, o termo "asma difícil de tratar" deve ser reservado para os pacientes que melhoram o controle da asma após medidas de higiene ambiental, melhora da técnica de uso dos dispositivos, melhora da adesão ao tratamento ou manejo adequado de comorbidades. Por outro lado, as mesmas publicações definiram "asma grave" como o grupo de pacientes que, apesar das medidas citadas anteriormente, necessitaram de medicamentos nas etapas 4 e 5 segundo GINA nos últimos 12 meses ou de corticoides sistêmicos por, no mínimo, 6 meses nos últimos 12 meses para manter o controle da asma ou que permaneceram sem um controle adequado apesar do tratamento.(4,5) Cabe destacar ainda que os pacientes definidos como AGNC seriam aqueles que mantiveram pelo menos um dos critérios além do baixo controle de sintomas(4,5): ACT < 20 pontos ou resultados equivalentes em outro escore validado para a verificação do controle da asma; duas ou mais exacerbações, necessitando de corticoide sistêmico no último ano; exacerbação grave com necessidade de internação no último ano; e persistência de limitação do fluxo aéreo apesar do tratamento nas etapas 4 ou 5 segundo GINA. (4,5) Portanto, torna-se cada vez mais importante a caracterização de pacientes com AGNC, bem como a identificação de desfechos que auxiliem na avaliação do impacto de intervenções nesses pacientes. Nesse contexto, inclui-se a capacidade de exercício e a força muscular respiratória.
No nosso estudo, os pacientes com AGNC percorreram uma DTC6 semelhante àquela prevista para a população brasileira.(18) Além disso, eles apresentaram comportamento normal da SpO2 média ao final do teste, redução adequada da FC um minuto após o término do TC6 e força muscular respiratória normal.
Como se sabe, o TC6 fornece indicadores da capacidade funcional, por meio da DTC6, da integridade da troca gasosa intrapulmonar pela SpO2, do estresse cardiovascular pela FC, da automação cardíaca pela FCR1 e do estresse sensorial pelos escores de dispneia.(8) Em nosso estudo, os pacientes percorreram, em média, 512 72 m no TC6, apesar de apresentarem padrão obstrutivo moderado, serem irregularmente ativos ou sedentários e apresentarem asma não controlada. Adicionalmente, não se observou dessaturação média significativa durante o teste (queda da SpO2 < 4% em relação aos valores basais).
Aproximadamente 71% dos participantes atingiram a %FCmáx, denotando uma troca gasosa eficiente e estresse cardiovascular satisfatório. A média de FCR1 (21,7 8,3 bpm) foi significativa, sugerindo automação cardíaca normal, o se que contrapõe com o achado de percepção da fadiga moderada e de dispneia (um pouco forte) ao final do teste. Após revisarmos a literatura, encontramos apenas um estudo em adultos sobre o comportamento de pacientes com asma grave durante o TC6.(11) Naquele estudo, a DTC6 nos pacientes com ADC foi significativamente menor em relação aos seus controles. (11) Entretanto, a média da DTC6 no grupo com ADC foi de 435 m,(11) aproximadamente 112 m inferior à DTC6 em nossa amostra. Cabe ressaltar que os pacientes daquele estudo eram mais velhos que os do presente estudo (52,3 8,3 anos vs. 49,8 14,4 anos), com maior grau de obstrução, indicado pelo VEF1 em % do previsto (44,0 15,9% vs. 58,8 21,8%) e faziam uso de mais medicamentos potentes, como corticoide oral (64% vs. 24%) e omalizumabe (47% vs. 12%).
Ao final do TC6, houve queda da SpO2 em 5 pacientes. Em 2 pacientes essa queda foi atribuída a broncoespasmo, revertido rapidamente com repouso e uso de 2-agonistas de curta duração. Os outros 3 pacientes tinham comorbidades (bronquiectasias devido a sequela de tuberculose, aspergilose broncopulmonar alérgica e enfisema pulmonar com aprisionamento aéreo, respectivamente). Esses resultados sugerem que, na ausência de broncoespasmo, a presença de dessaturação durante o TC6 em pacientes com AGNC deve alertar para a possibilidade de presença de comorbidades.
Para um grupo de autores,(27) a limitação ao exercício em pacientes com AGNC deve ser investigada quanto aos possíveis fatores, como a própria asma, hiperventilação alveolar, broncoconstrição induzida pelo exercício, descondicionamento físico, teste submáximo e isquemia cardíaca. Os autores observaram que, ao se identificarem os fatores limitantes, pode-se rever o tratamento, em especial o uso de altas doses de corticoide naqueles pacientes nos quais não foi encontrada limitação pulmonar.(27)
A medida da força muscular respiratória (PImáx e PEmáx) dos pacientes no presente estudo, em média, não foi diferente da observada em indivíduos normais. O aumento na capacidade residual funcional, causado pela hiperinsuflação pulmonar, retifica o diafragma e altera a mecânica respiratória, resultando em desvantagem mecânica, que pode ser inferida pela redução da força dos músculos respiratórios.(7,28) Entretanto, os asmáticos com distúrbio ventilatório obstrutivo leve ou moderado podem não apresentar hiperinsuflação pulmonar significativa que altere a posição do diafragma.(29,30) Como os pacientes da presente casuística apresentavam obstrução moderada das vias aéreas, é possível que esse fato justifique a similaridade de seus valores de PImáx e PEmáx com a de indivíduos normais.
Não encontramos diferenças significativas entre as médias de PImáx e PEmáx dos asmáticos com uso frequente de corticoide oral com aqueles com uso infrequente (três ou menos ciclos por ano). Entretanto, apenas 6 pacientes (24%) usavam corticoide oral continuamente. Um grupo de autores relatou redução da força muscular inspiratória em asmáticos dependentes de corticoides orais quando comparados com pacientes em uso de CI em altas doses e com graus semelhantes de hiperinsuflação pulmonar. (28) Deve-se ressaltar que 28% e 48% dos pacientes tiveram PImáx e PEmáx reduzidas, respectivamente. A força muscular respiratória pode estar reduzida principalmente em mulheres obesas em consequência de uma disfunção muscular respiratória. A atividade muscular ventilatória pode ser também comprometida pelo aumento da resistência elástica causada pelo excesso de tecido adiposo na caixa torácica e no abdome, o qual acarreta desvantagem mecânica aos músculos. (31,32) Em nosso estudo, 72% das pacientes eram do sexo feminino, com média de índice de massa corpórea de 28 kg/m2.
Embora os resultados do presente estudo devam ser avaliados com cautela, principalmente devido à falta de um grupo controle, à pequena casuística, ao delineamento transversal e por ter sido conduzido em um único centro, os mesmos são relevantes devido à escassez e às dificuldades de pesquisa da capacidade de exercício em pacientes com asma grave, assim como por representar uma amostra de um centro de referência de um hospital universitário e pelo alto poder estatístico observado (poder do teste de 81%).
Em conclusão, de acordo com a presente casuística, a DTC6 nos pacientes com AGNC foi semelhante aos valores previstos para a DTC6 em indivíduos normais no Brasil. A queda da SpO2 em 5 pacientes pode ser explicada pela presença de broncoespasmo e de comorbidades. A média das forças musculares respiratórias foi acima do limite inferior previsto, independente do uso de corticoide oral. São necessários novos estudos envolvendo um maior número de pacientes e com a inclusão de um grupo controle para um maior entendimento do comportamento da capacidade de esforço em pacientes com asma grave e para a definição do seu valor no manejo dessa doença.
Referências1. Global Initiative for Asthma - GINA. [homepage on the Internet]. Bethesda: Global Initiative for Asthma. [cited 2012 Sep 11]. Global Strategy for Asthma Management and Prevention. Available from: www.ginaasthma.org
2. Cruz AA, Fernandes AL, Pizzichini E, Fiterman J, Pereira LF, Pizzichini M, et al. Diretrizes da Sociedade Brasileira de Pneumologia e Tisiologia Para o Manejo da Asma - 2012. J Bras Pneumol. 2012;38(Suppl 1):S1-S46.
3. Barnes PJ, Woolcock AJ. Difficult asthma. Eur Respir J. 1998;12(5):1209-18 http://dx.doi.org/10.1183/09031936.98.12051209
4. Chung KF, Wenzel SE, Brozek JL, Bush MC, Sterk PJ, Adcock IM et al. International ERS/ATS guidelines on definition, evaluation and treatment of severe asthma. Eur Respir J. 2014;43(2):343-73. http://dx.doi.org/10.1183/09031936.00202013
5. Global Initiative for Asthma - GINA. [homepage on the Internet]. Bethesda: Global Initiative for Asthma. [cited 2014 Oct 1]. Global Strategy for Asthma Management and Prevention. Available from: www.ginaasthma.org
6. Schakman O, Gilson H, Thissen JP. Mechanisms of glucocorticoid-induced myopathy. J Endocrinol. 2008;197(1):1-10. http://dx.doi.org/10.1677/JOE-07-0606
7. Weiner P, Suo J, Fernandez E, Cherniack RM. Hyperinflation is associated with reduced strength and efficiency of the respiratory muscles in asthmatic and normal subjects. Chest. 1990;97(3 Suppl):69S-70S. http://dx.doi.org/10.1378/chest.97.3_Supplement.69S-a
8. Morales-Blanhir JE, Palafox Vidal CD, Rosas Romero Mde J, García Castro MM, Londo-o Villegas A, Zamboni M. Six-minute walk test: a valuable tool for assessing pulmonary impairment. J Bras Pneumol. 2011;37(1):110-7. http://dx.doi.org/10.1590/S1806-37132011000100016
9. Enright PL, Sherrill DL. Reference equations for the six-minute walk in healthy adults. Am J Respir Crit Care Med. 1998;158(5 Pt 1):1384-7. http://dx.doi.org/10.1164/ajrccm.158.5.9710086
10. Pereira CAC, Neder JA; Sociedade Brasileira de Pneumologia e Tisiologia (SBPT). Diretrizes para Testes de Função Pulmonar. J Pneumol. 2002;28(Suppl 3):1-238.
11. Freitas Canuto F, Silva SM, Malosá Sampaio LM, Stirbulov R, Ferrari Corrêa JC. Neurophysiological and functional assessment of patients with difficult-to-control asthma. Rev Port Pneumol. 2012;18(4):160-5. http://dx.doi.org/10.1016/j.rppneu.2012.02.008
12. Cavalcante Marcelino AM, Justino da Silva H. Role of maximal inspiratory pressure in the evaluation of respiratory muscle strength in asthmatics - Systematic review [Article in Portuguese]. Rev Port Pneumol. 2010;16(3):463-70. http://dx.doi.org/10.1016/S0873-2159(15)30042-8
13. Proceedings of the ATS workshop on refractory asthma: current understanding, recommendations, and unanswered questions. American Thoracic Society. Am J Respir Crit Care Med. 2000;162(6):2341-51. http://dx.doi.org/10.1164/ajrccm.162.6.ats9-00
14. ATS Committee on Proficiency Standards for Clinical Pulmonary Function Laboratories. ATS statement: guidelines for the Six-Minute Walk Test. Am J Respir Crit Care Med. 2002;166(1):111-7. http://dx.doi.org/10.1164/ajrccm.166.1.at1102
15. Shetler K, Marcus R, Froelicher VF, Vora S, Kalisetti D, Prakash M, et al. Heart rate recovery: validation and methodologic issues. J Am Coll Cardiol. 2001;38(7):1980-7. http://dx.doi.org/10.1016/S0735-1097(01)01652-7
16. Cole CR, Blackstone EH, Pashkow FJ, Snader CE, Lauer MS. Heart-rate recovery immediately after exercise as a predictor of mortality. N Engl J Med. 1999;341(18):1351-7. http://dx.doi.org/10.1056/NEJM199910283411804
17. Jolly MA, Brennan DM, Cho L. Impact of exercise on heart rate recovery. Circulation. 2011;124(14):1520-6. http://dx.doi.org/10.1161/CIRCULATIONAHA.110.005009
18. Soares MR, Pereira CA. Six-minute walk test: reference values for healthy adults in Brazil. J Bras Pneumol. 2011;37(5):576-83.
19. Pereira CA, Sato T, Rodrigues SC. New reference values for forced spirometry in white adults in Brazil. J Bras Pneumol. 2007;33(4):397-406. http://dx.doi.org/10.1590/S1806-37132007000400008
20. Black LF, Hyatt RE. Maximal respiratory pressures: normal values and relationship to age and sex. Am Rev Respir Dis. 1969;99(5):696-702.
21. Nathan RA, Sorkness CA, Kosinski M, Schatz M, Li JT, Marcus P, et al. Development of the asthma control test: a survey for assessing asthma control. J Allergy Clin Immunol. 2004;113(1):59-65. http://dx.doi.org/10.1016/j.jaci.2003.09.008
22. Roxo JP, Ponte EV, Ramos DC, Pimentel L, D'Oliveira Júnior A, Cruz AA. Portuguese-language version of the Asthma Control Test. J Bras Pneumol.
2010;36(2):159-66. http://dx.doi.org/10.1590/S1806-37132010000200002
23. Melosini L, Dente FL, Bacci E, Bartoli ML, Cianchetti S, et al. Asthma control test (ACT): comparison with clinical, functional, and biological markers of asthma control. J Asthma. 2012;49(3):317-23. http://dx.doi.org/10.3109/02770903.2012.661008
24. Academia.edu [homepage on the Internet] [cited 2012 Jul 2]. Guidelines for data processing and analysis of the International Physical Activity Questionnaire (IPAQ) - Short and long forms contents. [Adobe Acrobat document, 15p.]. Available from: https://www.academia.edu/5346814/Guidelines_for_Data_Processing_and_Analysis_of_the_International_Physical_Activity_Questionnaire_IPAQ_Short_and_Long_Forms_Contents
25. Pardini R, Matsudo S, Araújo T, Andrade E, Matsudo V, Braggion G, et al. Validação do questionário internacional de nível de atividade física (IPAQ - versão 6): estudo piloto em adultos jovens brasileiros. Rev Bras Ciênc Mov. 2001;9(3):45-51.
26. Machin D, Campbell M, Fayers P, Pinol A. Confidence intervals. In: Machin D, Campbell M, editors. Sample size tables for clinical studies. 2nd ed. London: Blackwell Science; 1997; p.122.
27. McNicholl DM, Megarry J, McGarvey LP, Riley MS, Heaney LG. The utility of cardiopulmonary exercise testing in difficult asthma. Chest. 2011;139(5):1117-23. http://dx.doi.org/10.1378/chest.10-2321
28. Akkoca O, Mungan D, Karabiyikoglu G, Misirligil Z. Inhaled and systemic corticosteroid therapies: Do they contribute to inspiratory muscle weakness in asthma? Respiration. 1999;66(4):332-7. http://dx.doi.org/10.1159/000029403
29. Oliveira CM, Lanza Fde C, Solé D. Respiratory muscle strength in children and adolescents with asthma: similar to that of healthy subjects? J Bras Pneumol. 2012;38(3):308-14. http://dx.doi.org/10.1590/S1806-37132012000300005
30. Decramer M, Lacquet LM, Fagard R, Rogiers P. Corticosteroids contribute to muscle weakness in chronic airflow obstruction. Am J Respir Crit Care Med. 1994;150(1):11-6. http://dx.doi.org/10.1164/ajrccm.150.1.8025735
31. Levin OS, Polunina AG, Demyanova MA, Isaev FV. Steroid myopathy in patients with chronic respiratory diseases. J Neurol Sci. 2014;338(1-2):96-101. http://dx.doi.org/10.1016/j.jns.2013.12.023
32. Weiner P, Waizman J, Weiner M, Rabner M, Magadle R, Zamir D. Influence of excessive weight loss after gastroplasty for morbid obesity on respiratory muscle performance. Thorax. 1998;53(1):39-42. http://dx.doi.org/10.1136/thx.53.1.39






