ABSTRACT
Tuberculosis and cryptococcosis are infectious diseases that can result in the formation of single or multiple nodules in immunocompetent patients. Exposure to silica is known to raise the risk of infection with Mycobacterium tuberculosis. We report the case of an elderly man with no history of opportunistic infections and no clinical evidence of immunodeficiency but with a six-month history of dry cough and nocturnal wheezing. A chest X-ray revealed a mass measuring 5.0 × 3.5 cm in the right upper lobe. The diagnostic approach of the mass revealed tuberculosis. The histopathological analysis of the surrounding parenchyma reveled silicosis and cryptococcosis. Cryptococcosis was also found in masses identified in the mediastinal lymph nodes. The surgical approach was indicated because of the degree of pleuropulmonary involvement, the inconclusive results obtained with the invasive and noninvasive methods applied, and the possibility of malignancy. This case illustrates the difficulty inherent to the assessment of infectious or inflammatory pulmonary pseudotumors, the differential diagnosis of which occasionally requires a radical surgical approach. Despite the presence of respiratory symptoms for six months, the first chest X-ray was performed only at the end of that period. We discuss the possible pathogenic mechanisms that might have led to the combination of three types of granulomatous lesions in the same lobe, and we emphasize the need for greater awareness of atypical presentations of pulmonary tuberculosis.
RESUMO
A tuberculose e a criptococose são infecções que podem cursar com a formação de nódulos isolados ou múltiplos em pacientes imunocompetentes. A exposição à sílica reconhecidamente eleva o risco de doença pelo Mycobacterium tuberculosis. Apresentamos o caso de um paciente idoso sem antecedentes de infecções oportunistas, sem evidência clínica atual de imunodeficiência, com história de tosse seca e sibilos, principalmente noturnos, com duração de seis meses, cuja radiografia de tórax evidenciava uma imagem tumoral medindo 5,0 × 3,5 cm em lobo superior do pulmão direito. A abordagem diagnóstica da massa evidenciou tratar-se de tuberculose, e a análise histopatológica do parênquima circunvizinho revelou a presença de criptococose e de silicose. Criptococose foi diagnosticada também em massas linfonodais mediastinais. A conduta cirúrgica foi imposta pelo grau de comprometimento pleuropulmonar localizado, pelo caráter inconclusivo das abordagens diagnósticas invasivas e não invasivas realizadas, assim como pela possibilidade de tratar-se de neoplasia. Este caso ilustra a dificuldade inerente ao diagnóstico diferencial de massas pulmonares de natureza infecciosa ou inflamatória simulando neoplasia, o que ocasionalmente impõe uma conduta cirúrgica radical. Apesar da presença de sintomas respiratórios por seis meses, a primeira radiografia do tórax só foi realizada tardiamente. São discutidos os possíveis mecanismos patogenéticos que possam ter levado a associação de três tipos de granulomatose no mesmo lobo pulmonar e é enfatizada a necessidade de uma maior divulgação das apresentações atípicas da tuberculose pulmonar.
Palavras-chave:
Tuberculose pulmonar; Radiografia pulmonar de massa; Silicose; Criptococose.
IntroductionAlthough the World Health Organization estimates that the overall tuberculosis incidence rate has been declining since 2004,(1) the high prevalence of the disease worldwide, especially in tropical countries, is still responsible for a high number of deaths and the segregation of individuals with debilitating sequelae.(2) The classic symptoms of pulmonary tuberculosis consist of dry or productive cough, asthenia, anorexia, fever, and weight loss, which, when associated with certain radiological patterns,(3,4) lead to a rapid diagnosis. However, certain, unusual, clinical and radiological presentations or presentations associated with other, chronic, lung diseases can make the etiologic diagnosis time-consuming and challenging.(2,5) Among occupational diseases, silicosis is known to be a contributing factor to pulmonary tuberculosis and other fungal infections.(6) Because of its opportunistic nature, tuberculosis is common in immunocompromised patients.(7) The development of tuberculosis depends on the known interaction between the host immune status and the aggressiveness of the infectious agent, which is expressed by virulence, concentration of agents, and ability to induce hypersensitivity.(8) In this context, it is necessary to consider the modifying effect of the disease, which changes the life status of current populations, who benefit from better nutrition, housing, and health conditions. Such changes include increased susceptibility to infections in people living with HIV and increased resistance to infections in those not living with HIV. Our objective was to report the case of an elderly male patient who was oligosymptomatic and apparently immunocompetent. The patient was a former construction worker. He underwent lobectomy because of a tumor mass in the right upper lobe. Pathological examination revealed tuberculosis. In addition, silica infiltration and cryptococcosis were found in the surrounding lung parenchyma, the latter being also found in the mediastinal lymph nodes. The literature lacks information regarding tuberculous pseudotumor.
Case reportWe report the case of a 73-year-old White male patient who was a retired construction worker, having worked as a mason's assistant most of his economically active life. The patient was a former smoker (smoking history, 10 pack-years). Over a 6-month period, he had daily episodes of dry cough, dyspnea, and wheezing that improved, albeit partially, with the use of intravenous xanthine and an inhaled 2 agonist, having often sought emergency room treatment. The patient was referred to our hospital after the identification of a lung tumor on a chest X-ray. He reported no fever, chest pain, or bloodstained sputum. In addition, he reported weight loss (3 kg) during that period.
The patient had systemic arterial hypertension and reflux esophagitis, both of which were controlled. He reported no diabetes, dyslipidemia, chronic respiratory diseases, or contact with tuberculosis patients.
The patient reported no alcoholism. In addition, he reported that he had raised animals when he was young and that he had been exposed to smoke from wood-burning stoves until the age of 25 years.
Physical examination revealed good general health. The patient had pallor of the skin and mucosa, and his body mass index was 29.7 kg/m2. He was well hydrated and was breathing normally, having no jaundice or cyanosis. In addition, he had no digital clubbing or lymph node enlargement. Respiratory findings included increased anteroposterior chest diameter, normal breath sounds, and diffuse wheezing. Arterial oxygen saturation was 90% on room air. Cardiovascular and abdominal examination was normal. No leg edema, varicose veins, or ulcers were observed.
Spirometry revealed mild obstructive lung disease unresponsive to bronchodilators. The Mantoux tuberculin skin test (TST) was performed, and the induration was 15 mm. Counterimmunoelectrophoresis for antifungal serum antibodies was negative for cryptococcosis, aspergillosis, histoplasmosis, and paracoccidioidomycosis.
A CT scan of the chest (Figure 1) showed a hypodense tumor mass located in the right upper lobe and measuring 5.0 × 3.5 cm. The major axis of the mass was directed toward the pulmonary hilum.
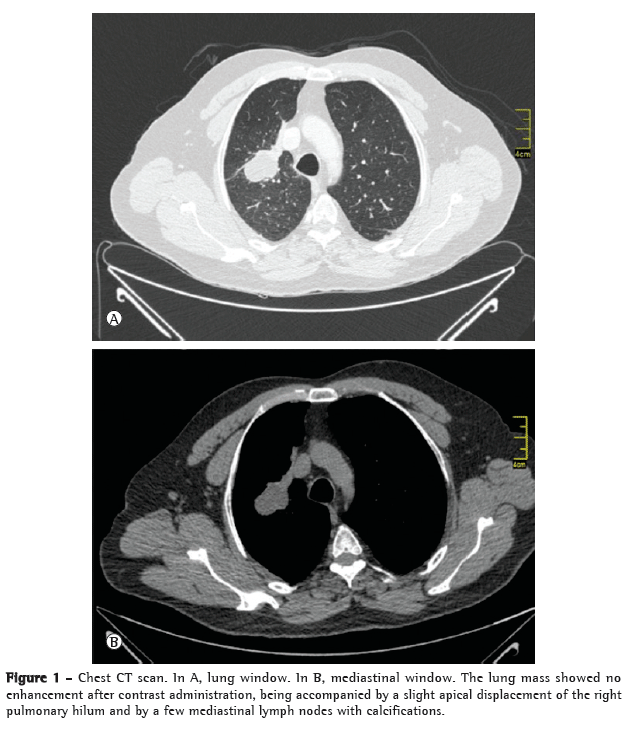
Wegener's granulomatosis was ruled out by negative antineutrophil cytoplasmic antibody test results associated with an absence of specific upper airway and nervous system symptoms.
Fiberoptic bronchoscopy was performed on two occasions, having shown extrinsic obstruction of the right upper lobe bronchus and its segmental bronchi. In addition, the bronchial mucosa appeared to be infiltrated. However, analysis of the biopsy samples was inconclusive, a surgical approach being therefore adopted.
The surgical specimen consisted of a cavitary mass in the right upper lobe (the contents of which were thick) and enlarged mediastinal lymph nodes.
Pathological examination of the mass revealed a dense chronic inflammatory infiltrate that was granulomatous and exudative, as well as extensive areas of caseous necrosis, fibrosis, and giant cell reaction (Figure 2); none of the various sections examined met histopathological criteria for malignancy. The presence of intracytoplasmic crystalloid structures in the adjacent lung parenchyma (as revealed by HE staining) constituted evidence of silicosis (Figure 3). The mediastinal lymph nodes showed a marked chronic inflammatory infiltrate that was granulomatous and exudative, as well as extensive areas of necrosis, lymph node architecture being extensively effaced.
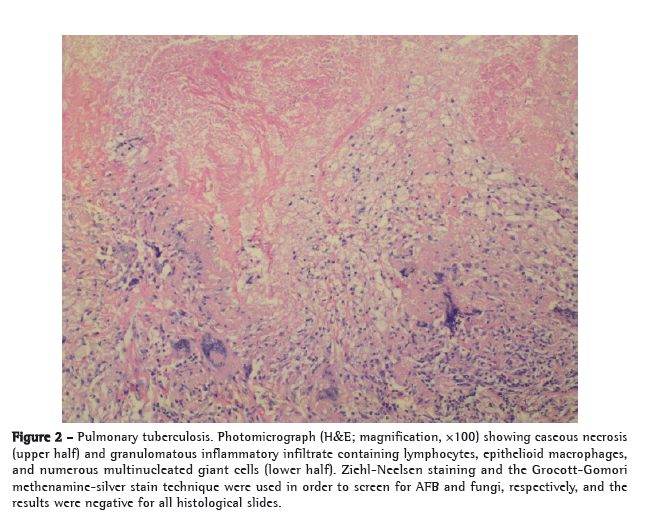
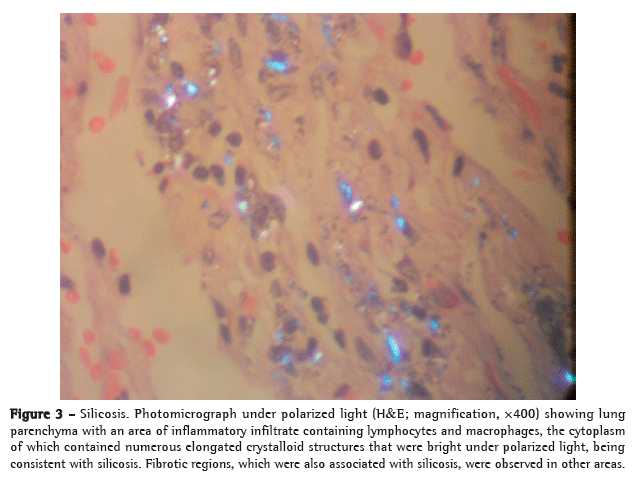
Serial histological sections were examined under oil immersion (total magnification, ×1,000). Ziehl-Neelsen staining and the Grocott-Gomori methenamine-silver stain technique were used in order to screen for AFB and fungi, respectively, and the results were negative for all histological slides. However, culture was positive for Mycobacterium tuberculosis.
The lung mass was tested in an automated culture system, and there was M. tuberculosis growth. In this technique, the tubes containing the biopsy material (classically macerated and decontaminated) are monitored in an automated culture system (BACTEC Mycobacteria Growth Indicator Tube (MGIT) 960; Becton Dickinson, Sparks, MD, USA) for up to 42 days of incubation, and any microorganism growing in a given tube emits fluorescence detectable by the system sensors, which indicate the tube as positive. Ziehl-Neelsen staining was used in order to screen the positive material for AFB, and the material was cultured on Löwenstein-Jensen medium for approximately 10 days. Mycobacterial colonies were analyzed by polymerase chain reaction, which identified M. tuberculosis by insertion sequence IS6110. Culture of the lung tissue surrounding the mass was negative; the lymph node samples were lost.
Lung tissue and mediastinal lymph node samples were cultured on Sabouraud agar, Cryptococcus neoformans having been isolated after 72 h of incubation. For metabolic recovery of the yeast and identification of Cryptococcus sp., a subculture of that isolate was performed, also on Sabouraud agar. The genus and species were confirmed by the VITEK 2 Compact and 21343 YST Test Kit VTK 2 automated system (bioMérieux, Marcy I'Étoile, France). The turbidity of the final suspension of saline solution containing the isolated colonies was analyzed with a DensiCHEK Plus device (bioMérieux), the results being within the 1.80-2.20 range, as established by the manufacturer. A fragment of the lung mass was cultured, and the results were negative.
The patient received pharmacological treatment, being treated with a regimen of rifampin, hydrazide, pyrazinamide, and ethambutol for 2 months, followed by rifampin and hydrazide for 4 months, in accordance with current recommendations for the treatment of tuberculosis.(7) In addition, he received itraconazole for 6 months.
At 5 months of pharmacological treatment for tuberculosis, the patient presented with a symmetric and painful increase in the mammary glands, which remained increased after the end of the treatment. We attribute this to a rare side effect of hydrazide, which has been reported by other authors.(9)
DiscussionIn the case reported here, the primary lesion was identified by histology and culture as tuberculous granuloma. In the context of pulmonary tuberculosis, parenchymal pseudotumoral tuberculosis is considered rare in adults.(10) Although host immunocompetence contributes to pulmonary cryptococcosis presenting as nodules, such nodules are typically subpleural and smaller in size, as described in guidelines published in 2008.(11) A low level of symptoms is not uncommon, being found in cases of tuberculosis(10) and in approximately 25% of all cases of cryptococcosis(11) in immunocompetent patients. Nevertheless, in the present case, the finding of cryptococcosis widely present in the mediastinal lymph nodes and sparsely present in the lung parenchyma prompted a reassessment of the immune status of the patient. His immunocompetence was evidenced by a negative HIV test (ELISA) result, normal serum immunoglobulin levels, a negative antinuclear factor test result, a negative rheumatoid factor test result, a high proportion of nitroblue tetrazolium-positive cells (spontaneous, 55 %; stimulated, 71%), and normal levels of CD4 and CD8 lymphocytes. The concomitant presence of those two processes in a single lung lobe, which was also affected by silica infiltration and right apical mediastinal and pleural involvement, mimicked the radiological appearance of a lung neoplasm. Although the conflict involving the differential diagnosis of lung masses in view of the possibility of malignancy is well known, the present case is unusual because of the capricious combination of common and severe diseases, as well as because of the difficulty in identifying the etiologic agents. This difficulty is due to the intrinsic characteristic of these infectious lesions; they have a low concentration of agents, which stands in contrast with the host immune response. Pulmonary pseudotumoral tuberculosis in adults has been defined by the presence of one or more masses in the parenchyma, such masses being caused by M. tuberculosis and arising as a primary or post-primary process. The pathological material, consisting of coalescing pulmonary infiltrates and caseous necrosis resulting from the presence of M. tuberculosis in the airways, can achieve large tumor size and only later reach the bronchial lumen,(10) generating cavities and causing elimination of sputum potentially containing bacilli. The combination of an atypical radiological presentation of pulmonary tuberculosis with a lack of classic symptoms and expected symptoms of an infectious disease producing pulmonary necrosis might be related to advanced age.(12) However, in a recent series of eight cases of pulmonary pseudotumoral tuberculosis,(10) the mean age was 36.0 ± 13.6 years; all patients reported a history of dry cough and had a Mantoux TST induration of 15-25 mm (as did our patient), whereas only two reported a history of fever and hemoptysis, another two having reported constitutional symptoms. It has been argued that atypical tuberculous lesions possibly represent delayed presentation of primary infection.(13) This should be taken into consideration in view of improvements in the health and living conditions of certain populations, as well as of programs to prevent and combat the disease. However, in the present case, the positive TST result-which represents effective specific immunity-and the apical location of the lesion are suggestive of secondary tuberculosis, which therefore results from the reactivation of quiescent foci resulting from the primary infection or from exogenous reinfection. In Brazil, lung lesions of less than 3 cm in diameter are likely to be diagnosed as tuberculoma, whereas tuberculous lesions the size of lung masses have rarely been reported and are limited to examples of radiological images.(3-5,14) This possibly contributed to our decision to focus on lung cancer in the present case, given that it is quite common in elderly patients with no comorbidities.
In our patient, the histopathological finding of silicosis was surprising because of the type of exposure, which is not among the most common risks(15) and which did not allow radiological recognition. This, however, does not rule out a strong correlation with tuberculosis. Although the mechanisms involved have yet to be fully elucidated, the relationship between chronic exposure to silica (even in the absence of silicosis) and an increased risk of developing tuberculosis is a harsh reality that is well documented in the literature.(16-18) The risk of developing tuberculosis has a direct relationship with the burden of exposure and, possibly, the duration of exposure (even if individuals are no longer exposed).(19)
The guidelines for the diagnosis of lung masses require that physicians be able to discriminate between malignant and benign lesions in order to avoid delays in the treatment of a malignant process or inadvertent interference with a benign process.(5,20) Therefore, physicians should rely on all available diagnostic methods, including invasive methods.(5) An analysis of the chain of increasingly complex interventions required for diagnosing an uncommon presentation of pulmonary tuberculosis under aggravating conditions shows the need for wider dissemination of information on atypical forms of pulmonary tuberculosis and their respective outcomes.
References1. Tuberculosis global facts 2010/2011. Cent Eur J Public Health. 2010;18(4):197. PMid:21361102
2. Hijjar MA, Procópio MJ, de Freitas LM, Guedes R, Bethlem EP. Epidemiologia da tuberculose: importância no mundo, no Brasil e no Rio de Janeiro. Pulmão RJ. 2005;14(4):310-4.
3. Bombarda S, Fiqueiredo CM, Funari MBG, Soares Jr J, Seiscento M, Terra-Filho M. Imagem em tuberculose pulmonar. J Pneumol. 2001;27(6):329-40. http://dx.doi.org/10.1590/S0102-35862001000600007
4. Capone D, Jansen JM, Lopes AJ, Sant'Anna CC, Soares MOT, Pinto RS, et al. Diagnóstico por imagem da tuberculose pulmonar. Pulmão RJ. 2006;15(3):166-74.
5. Lopes AJ, Jansen U, Capone D, Neves DD, Jansen JM. Diagnóstico de falsos tumores do pulmão. Pulmão RJ. 2005;14(1):33-42.
6. Iossifova Y, Bailey R, Wood J, Kreiss K. Concurrent silicosis and pulmonary mycosis at death. Emerg Infect Dis. 2010;16(2):318-20. http://dx.doi.org/10.3201/eid1602.090824 PMid:20113570 PMCid:PMC2958007
7. Conde MB, Melo FA, Marques AM, Cardoso NC, Pinheiro VG, Dalcin Pde T, et al. III Brazilian Thoracic Association Guidelines on tuberculosis. J Bras Pneumol. 2009;35(10):1018-48. PMid:19918635
8. Rich AR. Factores responsables de las características de las lesiones tuberculosas y de los sintomas. In: Rich AR, Croxatto OG, editors. Patogenia de la tuberculosis. Buenos Aires: Alfa; 1945. p. 609-73.
9. Morrone N, Morrone Junior N, Braz AG, Maia JA. Gynecomastia: a rare adverse effect of isoniazid. J Bras Pneumol. 2008;34(11):978-81. PMid:19099106
10. Agarwal R, Srinivas R, Aggarwal AN. Parenchymal pseudotumoral tuberculosis: case series and systematic review of literature. Respir Med. 2008;102(3):382-9. http://dx.doi.org/10.1016/j.rmed.2007.10.017 PMid:18060757
11. Moretti ML, Resende MR, Lazéra MS, Colombo AL, Shikanai-Yasuda MA. Guidelines in cryptococcosis--2008 [Article in Portuguese]. Rev Soc Bras Med Trop. 2008;41(5):524-44. Erratum in: Rev Soc Bras Med Trop. 2008;41(6):695. PMid:19009203
12. Pérez-Guzmán C, Vargas MH, Torres-Cruz A, Villarreal-Velarde H. Does aging modify pulmonary tuberculosis?: A meta-analytical review. Chest. 1999;116(4):961-7. http://dx.doi.org/10.1378/chest.116.4.961 PMid:10531160
13. Choyke PL, Sostman HD, Curtis AM, Ravin CE, Chen JT, Godwin JD, et al. Adult-onset pulmonary tuberculosis. Radiology. 1983;148(2):357-62. PMid:6867325
14. Pereira BA, Macedo SG, Nogueira RA, Castiel LCP, Penna CR. Aspectos tomográficos da consolidação lobar na tuberculose pulmonar primária. Radiol Bras. 2009;42(2):109-13. http://dx.doi.org/10.1590/S0100-39842009000200009
15. Neto FK, Gronchi CC, Saad IF, da Cunha IA, Possebon J, Teixeira MM, et al. Sílica: manual do trabalhador. São Paulo: Fundacentro; 1995.
16. Leung CC, Yu IT, Chen W. Silicosis. Lancet. 2012;379(9830):2008-18. http://dx.doi.org/10.1016/S0140-6736(12)60235-9
17. Barboza CE, Winter DH, Seiscento M, Santos Ude P, Terra Filho M. Tuberculosis and silicosis: epidemiology, diagnosis and chemoprophylaxis. J Bras Pneumol. 2008;34(11):959-66. http://dx.doi.org/10.1590/S1806-37132008001100012 PMid:19099104
18. Rees D, Murray J. Silica, silicosis and tuberculosis. Int J Tuberc Lung Dis. 2007;11(5):474-84. PMid:17439668
19. Corbett EL, Churchyard GJ, Clayton T, Herselman P, Williams B, Hayes R, et al. Risk factors for pulmonary mycobacterial disease in South African gold miners. A case-control study. Am J Respir Crit Care Med. 1999;159(1):94-9. http://dx.doi.org/10.1164/ajrccm.159.1.9803048 PMid:9872824
20. da Silva GA, Manco JC, Terra Filho J, Glass H, Soares FA. Mass on chest X-ray. Postgrad Med J. 1997;73(862):515-7. http://dx.doi.org/10.1136/pgmj.73.862.515 PMid:9307749 PMCid:PMC2431376




