ABSTRACT
Objective: To determine the diagnostic accuracy of positron emission tomography/computed tomography (PET/CT) using fluorine-
18‑deoxyglucose ([18F]-FDG) for the evaluation of a solitary pulmonary nodule (SPN). Methods: Prospective analysis of 53 consecutive
patients submitted to PET/CT between March 2005 and May 2007 for the evaluation of an SPN. Of those, 32 met the criteria for inclusion
in the present study. The lesions were evaluated for location, size, radiotracer uptake and maximum standardized uptake value (SUV). The
FDG-PET/CT results were correlated with other predictors of malignancy (age, gender, smoking status, nodule size and nodule location). The
definitive diagnosis was established through histopathology or through clinical/radiological follow-up for at least one year. Results: Fourteen
malignant SPNs were found. Through analysis of the receiver operating characteristic curve, we established an SUV of 2.5 as the most
appropriate cut-off point, since it correctly identified 13 of the 14 malignant SPNs. The results below that point revealed one false positive
for neoplasia out of a total of 14. The semiquantitative method presented a sensitivity of 92.9%, specificity of 72.2%, positive predictive
value of 72.2%, negative predictive value of 92.9% and accuracy of 81.2%. The multivariate analysis showed a statistically significant
association with SPN malignancy only for nodule location in the upper lobes (p = 0.048) and SUV (p = 0.007). Conclusions: The results
obtained suggest that the SUV of [18F]-FDG is a useful predictor of neoplasia in SPN, with a high negative predictive value, which allows
malignancy to be safely ruled out, showing its relevance in the diagnostic approach to pulmonary nodules.
Keywords:
Positron-emission tomography; Coin lesion, pulmonary; Lung neoplasms.
RESUMO
Objetivo: Determinar a acurácia diagnóstica da positron emission tomography (tomografia por emissão de pósitrons)/tomografia computadorizada
(PET/TC) com deoxiglicose marcada com flúor-18, conhecida como fluorodeoxiglicose (FDG[18F]), na avaliação de nódulo pulmonar
solitário (NPS). Métodos: Análise prospectiva de 53 pacientes consecutivos que realizaram PET/TC para avaliação de NPS, entre março de
2005 e maio de 2007. Destes 32 preencheram os critérios de inclusão. As lesões foram avaliadas quanto a sua localização e tamanho, grau de
captação do radiofármaco e o standardized uptake value (SUV, valor padronizado de captação) máximo das lesões. Os achados dos estudos
de FDG-PET/TC foram correlacionados com outros preditores de malignidade (idade, sexo, tabagismo, tamanho e localização do nódulo).
O diagnóstico definitivo foi estabelecido por confirmação histopatológica ou acompanhamento clínico-radiológico por um período mínimo
de um ano. Resultados: Encontrados 14 NPS malignos. Após análise da curva ROC, o SUV de 2,5 foi considerado o melhor ponto de corte
que identificou corretamente 13 dos 14 NPS malignos. Os resultados abaixo deste ponto de corte mostraram um exame falso positivo para
neoplasia num total de 14. O método semiquantitativo apresentou sensibilidade de 92,9%, especificidade de 72,2%, valor preditivo positivo
de 72,2%, valor preditivo negativo de 92,9% e acurácia de 81,2%. Na análise multivariada, apenas a localização do nódulo nos lobos superiores
(p = 0,048) e o SUV (p = 0,007) demonstraram significância estatística para malignidade no NPS. Conclusões: Os dados do estudo
mostram que o SUV da FDG[18F] é um bom preditor de neoplasia em nódulos pulmonares e com alto valor preditivo negativo, o que oferece
grande segurança em afastar presença de malignidade, indicando sua importância na abordagem diagnóstica do nódulo pulmonar.
Palavras-chave:
Tomografia por emissão de pósitrons; Nódulo pulmonar solitário; Neoplasias pulmonares.
IntroductionThe diagnostic approach to solitary pulmonary nodules (SPNs) continues to pose a great challenge to specialists in many areas, due to the absence of symptoms, the nonspecific morphological characteristics and the probability of malignancy.(1)
Primary neoplasia is found in approximately 35% of all SPNs.(2) However, most pulmonary nodules are inflammatory or granulomatous lesions.(3) The differentiation between the malignant and benign diseases requires the use of safe, reliable diagnostic methods.
When the clinical history, complementary imaging tests, cultures and serological tests are insufficient to confirm the diagnosis, surgical lung biopsy must be performed in order to accurately identify the etiology. However, the routine use of this technique will reveal many benign lesions, which could be clinically monitored.
Positron emission tomography (PET) using fluorine-18-deoxyglucose ([18F]-FDG) has been widely applied in lung cancer staging, especially in the detection of mediastinal metastases,(4) treatment planning, restaging following radiotherapy or chemotherapy and control of local recurrence of the disease.(5) This method has also been widely used for the evaluation of malignancy in SPNs and has been shown to be highly accurate.(6)
However, there have been few studies using PET/computed tomography (PET/CT) equipment to evaluate SPNs.
It is known that the glycolytic metabolism and, consequently, uptake of the [18F]-FDG are increased in inflammatory and granulomatous lesions,(7-10) especially in individuals with pulmonary tuberculosis, histoplasmosis or sarcoidosis.
Due to factors characteristic of Brazil, such as the high incidence of pulmonary tuberculosis(11) and endemic areas of histoplasmosis,(12) both diseases having the potential to give rise to SPNs, there is a need to establish a reliable predictor for the diagnosis of cancer in patients with pulmonary nodules.
The present study correlated the degree of uptake of [18F]-FDG in pulmonary nodules using a semiquantitative, visual analysis, together with the assessment of other predictive factors for lung cancer, such as age, gender, smoking status, size(13) and location of the nodule, to determine whether the standardized uptake value (SUV) of [18F]-FDG is a good predictor of cancer in SPNs and whether its diagnostic accuracy increases when used in conjunction with the factors mentioned above.
The principal objective of the present study was to evaluate the diagnostic performance of FDG-PET/CT in the characterization of SPNs.
MethodsThe study was conducted in the imaging sector of the Samaritano Hospital, a private hospital located in Rio de Janeiro, Brazil. This was a classical cohort study involving 53 consecutive patients submitted to FDG-PET/CT for the evaluation of SPNs between March of 2005 and April of 2007. The protocol was approved by the Samaritano Hospital Ethics
Committee (Process no. 0002018219705).
Among the patients initially evaluated, 21 were excluded for not meeting all of the inclusion criteria (being over 18 years of age; having no history of neoplasia; SPN having gone undiagnosed prior to the study outset; and confirmation of the diagnosis through histopathology) or for not remaining in clinical/radiological follow-up treatment for a minimum of one year after the FDG-PET/CT scan. Therefore, 32 patients were selected for inclusion in the study.
Demographic data such as age, gender, and smoking history were collected.
After the FDG-PET/CT results were known, the final decision regarding clinical follow-up or biopsy was made by the attending physician.
The patients fasted for 6 h prior to the FDG-PET/CT scan. The [18F]-FDG was administrated intravenously at a dose of approximately 448 MBq.
During the activation phase, in an appropriate room, the patients remained supine, covered with a blanket, without light or auditory stimuli, for 60 min (mean 73.2 ± 13.8 min), to avoid uptake of the radiotracer at physiological sites excited by these stimuli, which can result in artifacts that have false-positive interpretations. On this occasion, patients were instructed to drink 1 L of contrast material (barium diluted in water).
The images were acquired using a PET/CT Biograph 2 (Siemens Medical Solutions, Erlangen, Germany). The topogram of the CT was previously acquired at 130 kV and 30 mA in order to determine the area of obtainment of the image (skull base to the proximal portion of the thigh). The CT was then acquired in the craniocaudal plane (130 kV; 100 mA; tube rotation time of 0.8 s/slice; width 5 mm/slice; collimation of 4 mm), in expiration, in order to minimize the respiratory artifacts of the PET/CT.(14)
The FDG-PET/CT was then acquired with the patient in the same position in which the CT was performed, using the detection system with a complete ring of lutetium oxyorthosilicate crystals. For the acquisition of the PET scan in three dimensions in the craniocaudal direction, the time of emission of each effective biological dose was 3 min, resulting in a total PET time of approximately 21 min (7 effective biological doses).
The CT data previously described(15) were used for the attenuation correction. After attenuation correction of the PET data, the images were reconstructed using an algorithm of four interactions and a 128 × 128 matrix, as also previously described.(16)
The semiquantitative analysis of the degree of uptake of the lesions characterized by the FDG-PET/CT scans was based on the SUV. The SUV represents the activity of the radiotracer in a topographic region of the body image or volume of interest normalized to the weight of the patient and to the quantity of radiotracer administered to the patient, hence the formula: SUV = radiotracer activity × weight of the patient/injected dose, which characterizes the relative concentration of the radiotracer in the lesion of interest.
In the present study, we used the maximum SUV of the lesions, that is, the SUV for the pixel with the greatest uptake in the lesion (maximum pixel SUV), determined semi-automatically, with the aid of the E-soft program, version 4.0 (Siemens Medical Solutions) through the demarcation of a volume of interest in the lesion studied.
The studies were interpreted by consensus among a radiologist and two nuclear medicine physicians on a workstation (E-soft, Siemens Medical Solutions).
The SPNs were analyzed in terms of size and location.
The uptake of the radiotracer in the lesions was evaluated subjectively by determining the degree of uptake in the lesions in relation to that observed for the mediastinum. Lesions presenting no measurable uptake of the radiotracer, as well as those presenting uptake intensity less than or equal to that of the mediastinum, were considered negative for neoplasia.
Lesions presenting uptake of the radiotracer that was more intense than that observed for the mediastinum were considered positive for neoplasia.
In addition to the subjective analysis of the degree of uptake of the lesions, a semiquantitative analysis was carried out by determining the maximum SUV of the lesion, using semi-automatic outlining of an area around the lesion for volume measurement, with a margin of 50%. Other
hypermetabolic foci with suspicion of viable neoplastic tissue were duly registered.
The results of the FDG-PET/CT scans were known before the definitive diagnosis had been made.
All patients who were not submitted to biopsy were monitored as outpatients for at least one year after the FDG-PET/CT scan, during which time they underwent chest CT scans in order to evaluate the SPNs.
The diagnosis of malignant lesion was established through histopathological evaluation. The diagnosis of benign lesion was established through biopsy or based on a reduction in the stability of the SPN during the clinical and radiological follow-up evaluations.
The continuous variables were expressed as mean ± standard deviation or median and the interquartile range, depending on the distribution of data, and were compared using the Student's t-test and Mann-Whitney test. The Kolmogorov-Smirnov test was used to determine the distribution of data. The categorical variables were expressed as percentages and compared using the chi-square test or Fisher's exact test.
Diagnostic performance and the best SUV cut-off point were determined by constructing and analyzing a receiver operating characteristic (ROC) curve. Sensitivity, specificity, negative predictive value and positive predictive value were calculated for this cut-off point.
A multivariate logistic regression model was generated, including all variables presenting a p value < 0.1 in the univariate analysis. Statistical significance was determined using an alpha error of <5% (p < 0.05).
The statistical analysis was carried out using the Statistical Package for the Social Sciences, version 12.0 (SPSS Inc, Chicago, IL, USA).
ResultsIn the subjective analysis, 14 patients with neoplasia and 5 with benign disease presented higher uptake in the pulmonary nodule than in the mediastinum.
Regarding the semiquantitative analysis, among the 32, the [18F]-FDG SUV increased to ≥ 2.5 in 18 of the 32 patients evaluated, All 18 of those patients were then submitted to biopsy, in which the histopathology confirmed neoplasia in 13 (40.6% of the sample as a whole). The diagnoses were adenocarcinoma in 10 cases (31.3%), bronchioloalveolar carcinoma in one (3.1%), adenocarcinoma with areas of bronchioloalveolar carcinoma in one (3.1%) and non-Hodgkin's lymphoma in one (3.1%). In the other 5 patients with elevated SUV, the biopsy findings revealed histoplasmosis in 2 (6.2%), tuberculosis in one (3.1%), locally invasive aspergillosis in one (3.1%) and a nonspecific inflammatory process in one (3.1%). Of the 14 patients with low or no [18F]-FDG uptake, 2 were submitted to biopsy. In one (3.1% of the sample as a whole), the histopathological result was bronchioloalveolar carcinoma, whereas the other patient was diagnosed with tuberculosis, as shown in Table 1.
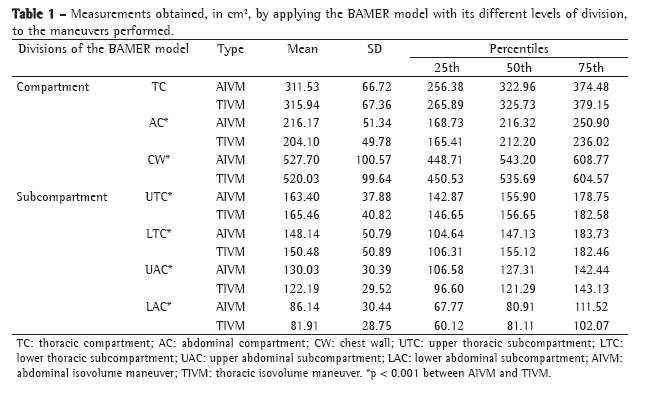
Among the 12 patients (38%) who were not submitted to biopsy, the SPN disappeared in 2 and remained unchanged in 10 (31.25%) at the end of the one-year follow-up period.
Of the 32 FDG-PET/CT scans performed, only one was false negative for neoplasia, in which the diagnosis was bronchioloalveolar carcinoma.
Of the 21 patients excluded, 10 (47.6%) were excluded for not completing one year of follow-up treatment, and 11 (52.4%) were excluded for having a history of neoplastic disease.
The diagnosis of adenocarcinoma was confirmed through histopathology in the 6 patients diagnosed with metastatic disease by FDG-PET/CT.
A diagnosis of cancer was not found to correlate with age, gender, smoking history or nodule size, although it was found to correlate with an [18F]-FDG SUV ≥ 2.5 and with nodule location in the upper lobes (Table 2).
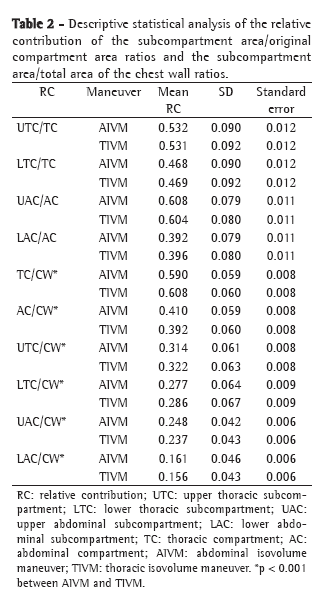
The average SPN diameter was 15.5 ± 6 mm (range, 5-25 mm), and nodule diameter did not correlate significantly with malignancy (p = 0.6).
Table 3 shows the demographic data, [18F]-FDG SUV, nodule size, nodule location, nodule uptake, mediastinal uptake, histopathological results and clinical follow-up.

The median SUVs in the patients with and without lung cancer were 5.55 (interquartile range, 3.45; 7.55) and 0.65 (interquartile range, 0; 3.5), respectively (p < 0.001).
The area under the ROC curve (Figure 1) to determine the best SUV cut-off point for a diagnosis of cancer was 0.877 (95% CI: 0.75-0.99).
Analyzing the curve, we identified 2.5 as the best cut-off point. For this cut-off point, the values for sensitivity, specificity, positive predictive value, negative predictive value and accuracy were 92.9, 72.2, 72.2, 92.9 and 81.2%, respectively.
In the multivariate logistic regression, which was adjusted for nodule size, nodule location, age, gender and smoking history, an SUV ≥ 2.5 and nodule location in the upper lobes were the only predictors of malignancy, with ORs, respectively, of 77.05 (95% CI: 3.2-1813) and 11.22 (95% CI: 1.02-122).
DiscussionThe present study evaluated the diagnostic accuracy of FDG-PET/CT in cases of SPN, as well as attempting to identify factors, as yet unreported in the literature, that are predictive of malignancy in SPNs.
The results show that determining the [18F]-FDG SUV, even in isolation, is a reliable means of ruling out SPN malignancy, presenting a negative predictive value of 92.9%.
The only case that FDG-PET/CT failed to identify correctly as neoplasia was a case of bronchioloalveolar carcinoma, which is known to present low uptake of [18F]-FDG(5) due to its biological characteristics, with great possibility of false negative results.(17)
The diagnostic accuracy was similar to that described in the literature,(18) with a slightly lower specificity, although with a high negative predictive
value for pulmonary neoplasia.
In a recent study, FDG-PET/CT showed excellent diagnostic performance in the differentiating between benign and malignant SPNs, with a specificity of 97% and a sensitivity of 85%. The authors of that study concluded that the combination of the anatomical and metabolic images preserves the sensitivity of the CT and the specificity of the PET, resulting in a significant improvement in accuracy.(19)
In our study, 6 patients were identified with metastatic disease, showing the usefulness of the FDG-PET/CT in the staging and identification of occult metastases. Therefore, it is possible to reduce costs by avoiding surgical treatment when it will provide no benefits to the patient.(20)
The use of invasive diagnostic methods, such as fine-needle puncture, presents risks such as pneumothorax, bleeding and dissemination of the tumor along the trajectory of the needle. Surgical lung biopsy has a mortality rate of approximately 0.6%,(21) which can be lower in centers where the staff has more experience.(22) Therefore, FDG-PET/CT proves to be a safe method and provides physicians with reliable data to eliminate the need for a surgical biopsy, allowing them to limit management of an SPN to clinical monitoring.
In the present study, we found no statistically significant correlations between malignancy and factors previously described as predictors of malignancy, such as smoking status, gender, age and nodule size.
Regarding smoking, only 21.8% of the patients were current smokers, and half of the former smokers had been abstinent for more than 10 years, which might have influenced the result, since the cessation of smoking for a period such as the mentioned above reduces the risk of lung cancer by approximately 50%.(23,24) Another factor that must be considered is that the principal histological types related to smoking are squamous cell carcinoma and small cell carcinoma,(23) which were not diagnosed in our study.
In relation to gender, we found no predominance of cancer in men, which is in agreement with data obtained in recent epidemiological investigations demonstrating that the incidence of the disease has increased significantly among women while decreasing among men, with a tendency toward equalization.(25)
Regarding the size of the nodules, we believe that the small size of the sample might have influenced this result.
We point out two significant limitations of the study. The first was that the population was highly selected, and the PET/CT was therefore performed only in patients with pulmonary nodules in which there was heightened suspicion of malignancy. Therefore, the large number of neoplasms confirmed might have influenced the final result. The second limitation was the small sample size, which made the statistical analysis and the visual evaluation between the SPN and the mediastinum impossible, due to the large number of FDG-PET/CT scans in which there was no uptake of [18F]-FDG, as well as to the absence of cases in which in which such uptake was greater in the mediastinum than in the nodule.
It is of note that the small sample size was due to the strictness of the inclusion criteria, which precluded the inclusion of patients with neoplasia at any site, either in activity or with criteria for cure, thus avoiding a predisposition to consider the SPN as malignant. In addition, recently diagnosed patients who had undergone PET/CT scans for staging were excluded, as were those with pulmonary masses.
The results obtained in this preliminary study allow us to conclude that the [18F]-FDG SUV is a good predictor of neoplasia in pulmonary nodules and can be used in the diagnostic investigation whenever available.
References 1. Pretreatment evaluation of non-small-cell lung cancer. The American Thoracic Society and the European Respiratory Society. Am J Respir Crit Care Med. 1997;156(1):320-32.
2. Tan BB, Flaherty KR, Kazerooni EA, Iannettoni MD; American College of Chest Physicians. The solitary pulmonary nodule. Chest. 2003;123(1 Suppl):89S-96S.
3. Ost D, Fein AM, Feinsilver SH. Clinical practice. The solitary pulmonary nodule. N Engl J Med. 2003;348(25):2535-42.
4. Gould MK, Kuschner WG, Rydzak CE, Maclean CC, Demas AN, Shigemitsu H, et al. Test performance of positron emission tomography and computed tomography for mediastinal staging in patients with non-small-cell lung cancer: a meta-analysis. Ann Intern Med. 2003;139(11):879-92.
5. Mavi A, Lakhani P, Zhuang H, Gupta NC, Alavi A. Fluorodeoxyglucose-PET in characterizing solitary pulmonary nodules, assessing pleural diseases, and the initial staging, restaging, therapy planning, and monitoring response of lung cancer. Radiol Clin North Am. 2005;43(1):1-21, ix.
6. Rohren EM, Lowe VJ. Update in PET imaging of nonsmall cell lung cancer. Semin Nucl Med. 2004;34(2):134-53.
7. Hara T, Kosaka N, Suzuki T, Kudo K, Niino H. Uptake rates of 18F-fluorodeoxyglucose and 11C-choline in lung cancer and pulmonary tuberculosis: a positron emission tomography study. Chest. 2003;124(3):893-901.
8. Zhuang H, Yu JQ, Alavi A. Applications of fluorodeoxyglucose-PET imaging in the detection of infection and inflammation and other benign disorders. Radiol Clin North Am. 2005;43(1):121-34.
9. El-Haddad G, Alavi A, Mavi A, Bural G, Zhuang H. Normal variants in [18F]-fluorodeoxyglucose PET imaging. Radiol Clin North Am. 2004;42(6):1063-81, viii.
10. Bombarda S, Júnior JS, Filho MT. Estudo do metabolismo da glicose na tuberculose pulmonar ativa utilizando a tomografia por emissão de pósitrons (18F-FDG PET). J Pneumol. 2002;28(5):270-6.
11. Ministério da Saúde. Fundação Nacional de Saúde. Controle da Tuberculose: Uma Proposta de Integração Ensino-Serviço. 5th ed. Rio de Janeiro: FUNASA/CRPHF/SBPT; 2002. 237p.
12. Martins EM, Marchiori E, Damato SD, Pozes AS, Silva AC, Dalston M. Histoplasmose Pulmonar Aguda: Relato de uma Microepidemia. Radiol Bras 2003;36(3):147-51.
13. Rivera MP, Stover DE. Gender and lung cancer. Clin Chest Med. 2004;25(2):391-400.
14. Gilman MD, Fischman AJ, Krishnasetty V, Halpern EF, Aquino SL. Optimal CT breathing protocol for combined thoracic PET/CT. AJR Am J Roentgenol. 2006;187(5):1357-60.
15. Kinahan PE, Hasegawa BH, Beyer T. X-ray-based attenuation correction for positron emission tomography/computed tomography scanners. Semin Nucl Med. 2003;33(3):166-79.
16. Hudson HM, Larkin RS. Accelerated image reconstruction using ordered subsets of projection data. IEEE Trans Med Imaging. 1994;13(4):601-9.
17. Ginsberg MS, Grewal RK, Heelan RT. Lung cancer. Radiol Clin North Am. 2007;45(1):21-43.
18. Fischer BM, Mortensen J, Højgaard L. Positron emission tomography in the diagnosis and staging of lung cancer: a systematic, quantitative review. Lancet Oncol. 2001;2(11):659-66.
19. Kim SK, Allen-Auerbach M, Goldin J, Fueger BJ, Dahlbom M, Brown M, et al. Accuracy of PET/CT in characterization of solitary pulmonary lesions. J Nucl Med. 2007;48(2):214-20.
20. Yi CA, Lee KS, Kim BT, Choi JY, Kwon OJ, Kim H, et al. Tissue characterization of solitary pulmonary nodule: comparative study between helical dynamic CT and integrated PET/CT. J Nucl Med. 2006;47(3):443-50.
21. van Rens MT, de la Rivière AB, Elbers HR, van Den Bosch JM. Prognostic assessment of 2,361 patients who underwent pulmonary resection for non-small cell lung cancer, stage I, II, and IIIA. Chest. 2000;117(2):374-9.
22. Bach PB, Cramer LD, Schrag D, Downey RJ, Gelfand SE, Begg CB. The influence of hospital volume on survival after resection for lung cancer. N Engl J Med. 2001;345(3):181-8.
23. Sachs S, Fiore JJ. An overview of lung cancer. Respir Care Clin N Am. 2003;9(1):1-25.
24. Thomas L, Doyle LA, Edelman MJ. Lung cancer in women: emerging differences in epidemiology, biology, and therapy. Chest. 2005;128(1):370-81.
25. Instituto Nacional de Câncer - INCA [homepage on the Internet]. Brasília: Ministério da Saúde. [cited 2007 Sep 12]. Atlas de Mortalidade por Câncer no Brasil 1979-1999. Available from: http://www.inca.gov.br/atlas.
___________________________________________________________________________________________________________________
Study conducted in the Radiology Department of the Universidade Federal do Rio de Janeiro - UFRJ, Federal University of Rio de Janeiro - and at the Luiz Felippe Mattoso Radiological Clinic - Rio de Janeiro, Brazil.
1. Assistant Professor of Pulmonology. Graduate School of Medicine of the Pontifícia Universidade Católica do Rio de Janeiro (PUC-Rio, Pontifical Catholic University of Rio de Janeiro) - Rio de Janeiro, Brazil.
2. Nuclear Physician. Samaritano Hospital/ Luiz Felippe Mattoso Radiological Clinic, Rio de Janeiro, Brazil.
3. Radiologist. Samaritano Hospital/ Luiz Felippe Mattoso Radiological Clinic, Rio de Janeiro, Brazil.
4. Nuclear Physician. Samaritano Hospital/ Luiz Felippe Mattoso Radiological Clinic, Rio de Janeiro, Brazil.
5. Physician. Samaritano Hospital, Rio de Janeiro, Brazil.
6. Full Professor of Pulmonology. Graduate School of Medicine of the Pontifícia Universidade Católica do Rio de Janeiro (PUC-Rio, Pontifical Catholic University of Rio de Janeiro) - Rio de Janeiro, Brazil.
7. Full Professor of Nuclear Medicine. Universidade Federal do Rio de Janeiro - UFRJ, Federal University of Rio de Janeiro - Rio de Janeiro, Brazil.
Correspondence to: Rafael de Castro Martins. Rua Macedo Sobrinho, 8 SL 203, Humaitá, CEP 22271-080, Rio de Janeiro, RJ, Brazil.
Tel 55 21 22667392. Fax 55 21 25275277. E-mail: rafaelcastromartins@gmail.com
Submitted: 7 June 2007. Accepted, after review: 22 October 2007.





