ABSTRACT
Objective: To assess ICU patients with COPD, in terms of in-hospital characteristics, two-year mortality and two-year functional status of survivors. Methods: A prospective cohort study involving patients with acute exacerbation of COPD admitted to the ICUs of two hospitals in the city of Porto Alegre, Brazil, between July of 2005 and July of 2006. At two years after discharge, survivors were interviewed by telephone in order to determine Karnofsky scores and scores on a scale regarding activities of daily living (ADL). Results: The sample comprised 231 patients. In-hospital mortality was 37.7%, and two-year post-discharge mortality was 30.3%. Of the 74 survivors, 66 were interviewed (89%). The mean age at ICU admission was 74 ± 10 years, and the mean Acute Physiology and Chronic Health Evaluation II score was 18 ± 7. Two or more comorbidities were present in 87.8% of the patients. Of the 66 interviewees, 57 (86.3%) lived at home, 58 (87.8%) were self-sufficient, 12 (18.1%) required oxygen therapy, and 4 (6.1%) still required ventilatory support. There was a significant reduction in the quality of life and autonomy of the survivors, as evidenced by the Karnofsky scores (85 ± 9 vs. 79 ± 11, p = 0.03) and ADL scale scores (29 ± 5 vs. 25 ± 7; p = 0.01), respectively. Conclusions: In this patient sample, two-year mortality was quite high. Although there was a noticeable reduction in the functional status of the survivors, they remained self-sufficient.
Keywords:
Pulmonary disease, chronic obstructive/mortality; Quality of life; Intensive care units.
RESUMO
Objetivo: Determinar a taxa de mortalidade de pacientes com DPOC e avaliar o estado funcional dos sobreviventes dois anos após a alta da UTI. Métodos: Estudo de coorte prospectiva realizada nas UTIs de dois hospitais na cidade de Porto Alegre (RS) com pacientes com exacerbação aguda de DPOC e internados em UTI entre julho de 2005 e julho de 2006. Dois anos após a alta, os sobreviventes foram entrevistados via telefone. Os dados obtidos foram utilizados na determinação dos escores da escala de Karnofsky e de uma escala de atividades de vida diária (AVD). Resultados: Foram incluídos 231 pacientes. A mortalidade hospitalar foi de 37,7% e a mortalidade extra-hospitalar foi de 30,3%. Dos 74 sobreviventes, foram entrevistados 66 (89%). A média de idade dos pacientes no momento da internação na UTI era de 74 ± 10 anos e a do escore Acute Physiology and Chronic Health Evaluation II era de 18 ± 7. Tinham duas ou mais comorbidades 87,8% dos pacientes. Dos 66 entrevistados, 57 (86,3%) viviam em suas casas, 58 (87,8%) eram capazes de realizar seu autocuidado, 12 (18,1%) utilizavam oxigenoterapia, e 4 (6,1%) necessitavam suporte ventilatório. Houve uma significante redução na qualidade de vida e na autonomia, segundo os escores da escala de Karnofsky (85 ± 9 vs. 79 ± 11; p = 0,03) e de AVD (29 ± 5 vs. 25 ± 7; p = 0,01), respectivamente. Conclusões: A mortalidade desta amostra de pacientes foi muito elevada nos primeiros dois anos. Embora houvesse evidente redução do estado funcional dos sobreviventes, os mesmos preservaram a capacidade de realizar seu autocuidado.
Palavras-chave:
Doença pulmonar obstrutiva crônica/mortalidade; Qualidade de vida; Unidades de terapia intensiva.
IntroductionIt has been estimated that COPD, currently the sixth leading cause of death worldwide, will have become the third leading cause of death by 2020.(1) The researchers who constitute the Global Initiative for Chronic Obstructive Lung Disease have been standardizing the preventive and treatment practices for COPD; this has greatly benefited patients because the natural history of COPD is chronic and is characterized by a progressive decline in pulmonary function, as well as by recurrent exacerbations and frequent hospitalizations.(2)
The development of acute respiratory failure, which often requires ventilatory support, worsens the prognosis of the disease,(2,3) as well as increasing health care costs.(4,5) In-hospital mortality among patients with acute exacerbation of COPD admitted to the ICU is 20-82%,(6,7) and the one-year mortality rate is 11-39%.(2,8,9) A retrospective study(10)
evaluating 101 patients who required invasive ventilatory support because they were suspected of having COPD exacerbation demonstrated that the two-year survival rate among patients in follow-up treatment was 55.4%.
Although many instruments have been developed in order to evaluate mortality in patients with COPD, less attention has been given to the quality of life of survivors. The reintegration of COPD patients into society, their cognitive sequelae, their motor sequelae, their ability to maintain adequate social interaction, and their ability to resume their work activities, as well as the psychological changes that they experience, have yet to be properly studied.(11,12) The objective of the present study was to assess ICU patients with COPD, in terms of two-year mortality and the functional status of survivors two years out.
MethodsThe present study was a prospective cohort study involving all COPD patients admitted to two medical-surgical ICUs in the city of Porto Alegre, Brazil (the Central ICU of the Santa Casa Hospital Complex in Porto Alegre, a university hospital with 18 beds; and the Adult ICU of the Moinhos de Vento Hospital, a private hospital with 21 beds), between July of 2005 and July of 2006. During the study period, 1,219 patients were admitted (566 and 653, respectively). Of those, 231 were admitted because of COPD exacerbation and were therefore included in the present study. The study was approved by the research ethics committees of the two institutions.
The diagnosis of COPD was based on data from hospital admission records and on the clinical history taken by the attending physician. The clinical history included the following: smoking history; previous hospitalizations for COPD exacerbation; current cough and chronic dyspnea; constant or continuous use of bronchodilators or corticosteroids; and pulmonary function data obtained by spirometry.
During the ICU stay of each patient, we collected data related to the following: age; gender; Acute Physiology and Chronic Health Evaluation II (APACHE II) score; accompanying diseases; length of ICU stay; length of hospital stay; need for mechanical ventilation; need for dialysis; respiratory infection; septic shock; and outcome.
Two years after the patients had been discharged from the ICU, the researchers contacted the patients or closest family members by telephone in order to explain the objective of the present study, request the address to which the written informed consent form was to be mailed, and schedule a telephone interview. Together with the consent form, we mailed a return postage-paid envelope in order to facilitate the return of the consent form. Patients who refused to sign the consent form were excluded from the present study.
After the interviews had been scheduled and the consent forms had been returned, we collected the data by administering the research instrument in the form of an interview. The interviewers had previously been trained in using the structured questionnaire and administering it by telephone. The data collected by filling out the questionnaires allowed us to calculate the scores on two numeric scales: the Karnofsky scale; and a scale to assess activities of daily living (ADLs).(13-15)
Statistical analysisThe data are expressed as means ± SD, as medians (interquartile range), or as proportions. Categorical variables were analyzed by the chi-square test and Fisher's exact test. Continuous variables with normal distribution were analyzed by the Student's t-test for paired samples, whereas those with non-normal distribution were analyzed by the Mann-Whitney test. Values of p < 0.05 were considered significant. Patient mortality throughout the months was demonstrated by the Kaplan-Meier curve. The data were analyzed with the Statistical Package for the Social Sciences, version 16.0 (SPSS Inc., Chicago, IL, USA).
ResultsOf the 1,219 patients who were admitted to the ICUs during the 12-month study period, 231 were admitted for acute exacerbation of COPD. We interviewed 66 patients (28.6%). There were 165 patients who were not interviewed, because of the following (Figure 1): death in the ICU, in 63 patients (27.3%); in-hospital death after ICU discharge, in 24 (10.4%); death less than 6 months after ICU discharge, in 42 (18.2%); death within 6-12 months after ICU discharge, in 19 (8.2%); and death within 12-24 months after ICU discharge, in 9 (3.9%). In addition, 8 patients (3.4%) were excluded from the study: 5 because they declined to participate; and 3 because they were lost to follow-up.
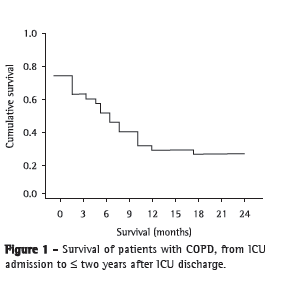
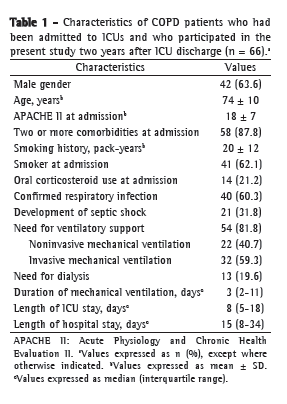
Of the 66 patients who were interviewed (89% of the two-year survivors), 66.4% were male, the mean age being 74 ± 10 years and the mean APACHE II score at ICU admission being 18 ± 7. Approximately 60% had presented with respiratory infection at ICU admission or developed respiratory infection during their stay in the ICU, and 31.8% had developed septic shock. Approximately 82% had required ventilatory support, and 19.6% had required dialysis (Table 1).
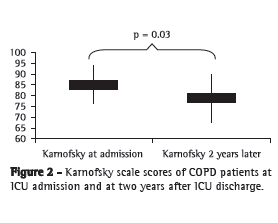
As can be seen in Table 2, 86.3% of the two-year survivors lived at home, 18.1% required home oxygen therapy; and 6% were dependent on ventilatory support. Figure 2 shows a reduction in the quality of life of survivors, as evidenced by the difference between the mean Karnofsky scale scores at ICU admission and those calculated at two years after ICU discharge (85 ± 9 vs. 79 ± 11; p = 0.03). Figure 3 shows a significant loss of autonomy among survivors, as evidenced by the difference between the mean ADL scale scores at ICU admission and those calculated at two years after ICU discharge (29 ± 5 vs. 25 ± 7; p = 0.01).

 Discussion
DiscussionIn the present study, ICU mortality was high among patients with COPD, as was mortality within the first months after hospital discharge. Although there was a noticeable reduction in the functional status of the survivors, they remained self-sufficient.
Approximately one third of patients with acute exacerbation of COPD die during their stay in the ICU,(2,3,9) and mortality remains high in the first year after hospital discharge.(2,3,9,16,17) In our study sample, mortality in the ICU was 27.3%, and the mortality rate in the first year after hospital discharge was 64.6%. At the time of the interview, two years after ICU discharge, 32% of our patients were alive. In three other studies,(9,12,17) two-year survival was 51%, 44%, and 41.9%, respectively. The prognosis for such patients has been related to multiple factors, including pulmonary function test results, blood gas analysis results, degree of pulmonary hypertension, age, nutritional status, need for ventilatory support, and APACHE II score at ICU admission.(6,9,16-19) The reintegration of such patients into society, in terms of their ability to maintain adequate social interaction or perform their activities satisfactorily, has yet to be thoroughly investigated.(12-15) There are few data regarding the need for hospital readmissions, the degree of dependence, the ability to remain self-sufficient, and the ability to resume work activities. The principal sequelae in individuals who survive critical disease are cognitive impairment,(20,21) neuromuscular weakness, polyneuropathy,(22) end-stage renal failure,(23) and ventilatory support dependence.(3,24) Patients with COPD constitute a group of patients who are particularly likely to develop such problems.
One group of authors(12) demonstrated that 75% of the patients with COPD who survived their ICU stay were self-sufficient six years after discharge. Our data show that 87.8% of the patients who survived remained self-sufficient two years after discharge. Most patients retain their ability to ambulate and perform tasks that require precise movements; in addition, they retain their cognitive abilities and are able to preserve intrafamily and interfamily relationships.(12) However, there is a reduction in exercise tolerance, as well as in the ability to perform work activities.(12,25) One study demonstrated, by means of the Glasgow Outcome Score, moderate worsening of the quality of life of survivors.(12)
Our data are in agreement with those from that study because we found a significant reduction in Karnofsky scale and ADL scale scores at two years after ICU discharge. It is noteworthy that, after hospital discharge, 18% of the patients in the present study required home oxygen therapy and 6% required ventilatory support, via tracheostomy or noninvasive ventilation, after hospital discharge. One group of authors(26) reported that the quality of life of 73% of patients with COPD improved or remained the same 6 months after ICU discharge, without the need for additional drugs.
The terms "health status", "social functioning", and "quality of life" have been used interchangeably in clinical studies and defined as health-related quality of life.(27) In order to assess the clinical conditions, psychological conditions, and autonomy of patients who are critically ill and receive treatment in the ICU, patient status has been graded by health status scales, functional independence scales, and scales regarding the ability to perform simple ADLs.(27) Each scale has characteristics that allow a more appropriate evaluation of the different subgroups of patients, taking into consideration aspects such as pathology, age, and comorbidities. The scales that are most commonly used in order to evaluate functional capacity in the elderly are the Katz scale and the Lawton scale.(27) Neurological patients benefit from the use of the Glasgow Outcome Score, the Barthel index, and the Rankin scale.(27) In order to assess quality of life, the Medical Outcomes Study 36-item Short-form Survey and its shortened version, comprising 12 items, can be used, as can other instruments, such as the EuroQol Group questionnaire.(14,15,27) The ADL scale(27) grades the ability of elderly individuals to perform ADLs such as taking their medication, using the telephone, and preparing food. The Karnofsky scale(15,27) assesses self-care, work capacity, the ability to ambulate, and the need for assistance in performing those tasks. In order to assess the functional capacity, autonomy, and quality of life of our patients, we chose to use the Karnofsky and ADL scales because they are easy to administer and to complete, as well as having been previously validated for use via telephone in similar studies involving critically ill patients.(28)
The objective of the present prospective cohort study was to evaluate the prognosis of patients admitted to ICUs and the quality of life of survivors at two years after ICU discharge. The strength of the present study lies in its design, which is appropriate for data collection in prognostic studies (cohort). In addition, the study was conducted at two different facilities, and there is a lack of similar data in Brazil. One of the limitations of the present study is the small sample size, which is due to the high mortality rate in the first year after ICU discharge, which in turn prevented us from furthering the analysis of aspects such as infectious exacerbations versus noninfectious exacerbations, invasive ventilatory support versus noninvasive ventilatory support, and presence of comorbidities versus absence of comorbidities.
The small sample size is also attributable to difficulties related to the lack of diagnostic criteria, as well as to the diagnostic confusion with asthma, especially in the subgroup of elderly individuals; to the lack of information regarding the severity of COPD, including pulmonary function test results and the need for home oxygen therapy prior to ICU admission; and to the fact that we did not use questionnaires specific to the evaluation of COPD patients.(29,30) Another limitation is the lack of specific assessment of exercise capacity, which has been reported to be greatly impaired in such patients.(12,25)
In conclusion, ICU mortality among the COPD patients evaluated in the present study was high, as was mortality in the first months after hospital discharge. In addition, the survivors remained self-sufficient two years after ICU discharge, although their functional capacity was significantly reduced, as demonstrated by the Karnofsky scale and ADL scale scores.
References1. Global Initiative for Chronic Obstructive Lung Disease [homepage on the Internet]. Bethesda: Global Initiative for Chronic Obstructive Lung Disease. [cited 2010 Feb 03]. Global Strategy for Diagnosis, Management and Prevention of COPD. Updated 2008. Available from: http://www.goldcopd.org/Guidelineitem.asp?l1=2l2=1intId=989
2. Ai-Ping C, Lee KH, Lim TK. In-hospital and 5-year mortality of patients treated in the ICU for acute exacerbation of COPD: a retrospective study. Chest. 2005; 128(2):518-24.
3. Quinnell TG, Pilsworth S, Shneerson JM, Smith IE. Prolonged invasive ventilation following acute ventilatory failure in COPD: weaning results, survival, and the role of noninvasive ventilation. Chest. 2006;129(1):133-9.
4. Miravitlles M, Murio C, Guerrero T, Gisbert R; DAFNE Study Group. Decisiones sobre Antibioticoterapia y Farmacoeconomía en la EPOC. Pharmacoeconomic evaluation of acute exacerbations of chronic bronchitis and COPD. Chest. 2002;121(5):1449-55.
5. Chen YH, Yao WZ, Cai BQ, Wang H, Deng XM, Gao HL, et al. Economic analysis in admitted patients with acute exacerbation of chronic obstructive pulmonary disease. Chin Med J (Engl). 2008;121(7):587-91.
6. Steer J, Gibson GJ, Bourke SC. Predicting outcomes following hospitalization for acute exacerbations of COPD. QJM. 2010;103(11):817-29.
7. Jezler S, Holanda MA, José A, Franca S. Mechanical ventilation in decompensated chronic obstructive pulmonary disease (COPD) [Article in Portuguese]. J Bras Pneumol. 2007;33 Suppl 2S:S111-8.
8. Groenewegen KH, Schols AM, Wouters EF. Mortality and mortality-related factors after hospitalization for acute exacerbation of COPD. Chest. 2003;124(2):459-67.
9. Connors AF Jr, Dawson NV, Thomas C, Harrell FE Jr, Desbiens N, Fulkerson WJ, et al. Outcomes following acute exacerbation of severe chronic obstructive lung disease. The SUPPORT investigators (Study to Understand Prognoses and Preferences for Outcomes and Risks of Treatments). Am J Respir Crit Care Med. 1996;154(4 Pt 1):959-67. Erratum in: Am J Respir Crit Care Med 1997;155(1):386.
10. Raurich JM, Pérez J, Ibáñez J, Roig S, Batle S. In-hospital and 2-year survival of patients treated with mechanical ventilation for acute exacerbation of COPD. Arch Bronconeumol. 2004;40(7):295-300.
11. Euteneuer S, Windisch W, Suchi S, Köhler D, Jones PW, Schönhofer B. Health-related quality of life in patients with chronic respiratory failure after long-term mechanical ventilation. Respir Med. 2006;100(3):477-86.
12. Rivera-Fernández R, Navarrete-Navarro P, Fernández-Mondejar E, Rodriguez-Elvira M, Guerrero-López F, Vázquez-Mata G, et al. Six-year mortality and quality of life in critically ill patients with chronic obstructive pulmonary disease. Crit Care Med. 2006;34(9):2317-24.
13. Hofhuis JG, Spronk PE, van Stel HF, Schrijvers GJ, Rommes JH, Bakker J. The impact of critical illness on perceived health-related quality of life during ICU treatment, hospital stay, and after hospital discharge: a long-term follow-up study. Chest. 2008;133(2):377-85.
14. Fildissis G, Zidianakis V, Tsigou E, Koulenti D, Katostaras T, Economou A, et al. Quality of life outcome of critical care survivors eighteen months after discharge from intensive care. Croat Med J. 2007;48(6):814-21.
15. Conlon N, O'Brien B, Herbison GP, Marsh B. Long-term functional outcome and performance status after intensive care unit re-admission: a prospective survey. Br J Anaesth. 2008;100(2):219-23.
16. Seneff MG, Wagner DP, Wagner RP, Zimmerman JE, Knaus WA. Hospital and 1-year survival of patients admitted to intensive care units with acute exacerbation of chronic obstructive pulmonary disease. JAMA. 1995;274(23):1852-7.
17. Breen D, Churches T, Hawker F, Torzillo PJ. Acute respiratory failure secondary to chronic obstructive pulmonary disease treated in the intensive care unit: a long term follow up study. Thorax. 2002;57(1):29-33.
18. Nevins ML, Epstein SK. Predictors of outcome for patients with COPD requiring invasive mechanical ventilation. Chest. 2001;119(6):1840-9.
19. Afessa B, Morales IJ, Scanlon PD, Peters SG. Prognostic factors, clinical course, and hospital outcome of patients with chronic obstructive pulmonary disease admitted to an intensive care unit for acute respiratory failure. Crit Care Med. 2002;30(7):1610-5.
20. Hopkins RO, Jackson JC. Long-term neurocognitive function after critical illness. Chest. 2006;130(3):869-78.
21. Hough CL, Curtis JR. Long-term sequelae of critical illness: memories and health-related quality of life. Crit Care. 2005;9(2):145-6.
22. Latronico N, Shehu I, Seghelini E. Neuromuscular sequelae of critical illness. Curr Opin Crit Care. 2005;11(4):381-90.
23. Uchino S, Kellum JA, Bellomo R, Doig GS, Morimatsu H, Morgera S, et al. Acute renal failure in critically ill patients: a multinational, multicenter study. JAMA. 2005;294(7):813-8.
24. Scheinhorn DJ, Artinian BM, Catlin JL. Weaning from prolonged mechanical ventilation. The experience at a regional weaning center. Chest. 1994;105(2):534-9.
25. Iribarren-Diarasarri S, Aizpuru-Barandiarana F, Loma-Osorio A, Castedo-González J, Poveda-Hernández Y, Muñoz-Martínez T, et al. Factores pronósticos de mortalidad en pacientes con enfermedad pulmonar obstructiva crónica tras su ingreso en una Unidad de Medicina Intensiva. El papel de la calidad de vida. Med Intensiva. 2005;29(4):204-11.
26. Wildman MJ, Sanderson CF, Groves J, Reeves BC, Ayres JG, Harrison D, et al. Survival and quality of life for patients with COPD or asthma admitted to intensive care in a UK multicentre cohort: the COPD and Asthma Outcome Study (CAOS). Thorax. 2009;64(2):128-32.
27. Dowdy DW, Eid MP, Sedrakyan A, Mendez-Tellez PA, Pronovost PJ, Herridge MS, et al. Quality of life in adult survivors of critical illness: a systematic review of the literature. Intensive Care Med. 2005;31(5):611-20.
28. Cabral CR, Teixeira C, Oliveira RP, Hass JS, Azzolin KO. Avaliação da mortalidade e qualidade de vida dois anos após a alta do CTI: dados preliminares de uma coorte prospectiva. Rev Bras Ter Intensiva. 2009;21(1):18-24.
29. Pereira ED, Pinto R, Alcantara M, Medeiros M, Mota RM. Influence of respiratory function parameters on the quality of life of COPD patients. J Bras Pneumol. 2009;35(8):730-6.
30. Dourado VZ, Antunes LC, Tanni SE, Godoy I. Factors associated with the minimal clinically important difference for health-related quality of life after physical conditioning in patients with COPD. J Bras Pneumol. 2009;35(9):846-53.
* Study carried out at the Moinhos de Vento Hospital and the Santa Casa Hospital Complex in Porto Alegre, Porto Alegre, Brazil.
Correspondence to: Cassiano Teixeira. Rua Riveira, 355/403, CEP 90670-160, Porto Alegre, RS, Brasil.
Tel/Fax: 55 51 3312-2608.
E-mail: cassiano.rush@terra.com.br
Financial support: None.
Submitted: 5 December 2010. Accepted, after review: 28 February 2011.
About the authorsCassiano Teixeira
Intensivist. Adult ICU, Moinhos de Vento Hospital; Central ICU, Santa Casa Hospital Complex in Porto Alegre. Adjunct Professor, Universidade Federal de Ciências da Saúde de Porto Alegre - UFCSPA, Federal University of Health Sciences of Porto Alegre - Porto Alegre, Brazil.
Cláudia da Rocha Cabral
Nurse. Central ICU, Santa Casa Hospital Complex in Porto Alegre, Porto Alegre, Brazil.
Jaqueline Sangiogo Hass
Nurse. ICU, Porto Alegre Hospital de Clínicas, Porto Alegre, Brazil.
Roselaine Pinheiro de Oliveira
Intensivist. Adult ICU, Moinhos de Vento Hospital; Central ICU, Santa Casa Hospital Complex in Porto Alegre, Porto Alegre, Brazil.
Mara Ambrosina de Oliveira Vargas
Coordinator. Graduate Nursing Program in Intensive Care, Universidade do Vale do Rio dos Sinos - UNISINOS, Vale do Rio dos Sinos University - São Leopoldo, Brazil.
Ana Paula da Rocha Freitas
Resident in Internal Medicine. Santa Casa Hospital Complex in Porto Alegre, Porto Alegre, Brazil.
Alessandra Hofstadler Deiques Fleig
Resident in Internal Medicine. Santa Casa Hospital Complex in Porto Alegre, Porto Alegre, Brazil.
Erika Cristine Treptow
Resident in Internal Medicine. Santa Casa Hospital Complex in Porto Alegre, Porto Alegre, Brazil.
Márcia Inês Boff Rizzotto
Resident in Internal Medicine. Santa Casa Hospital Complex in Porto Alegre, Porto Alegre, Brazil.






