ABSTRACT
In this study, we analyzed the number of TB cases in an emergency room (ER) and the susceptibility profile of Mycobacterium tuberculosis strains. Patients were selected from among those treated at the Hospital das Clínicas, in the city of Belo Horizonte, Brazil. Between 2002 and 2005, 240 TB patients were identified. Of those, 117 patients (48.7%) were diagnosed in the ER, 72 (61.5%) presenting positive sputum smear microscopy. Drug susceptibility testing was carried out in 90 strains, of which 80 (89%) were sensitive, 9 (10%) were resistant, and 1 (1%) was multidrug resistant. The incidence of positive smear sputum microscopy and resistant TB strains was high, which calls for the immediate adoption of TB control measures in the ER.
Keywords:
Tuberculosis; Disease transmission, infectious; Drug resistance.
RESUMO
Neste trabalho, analisamos o número de casos de TB em um pronto-atendimento (PA) e o perfil de sensibilidade das cepas de Mycobacterium tuberculosis. Pacientes atendidos no Hospital das Clínicas, em Belo Horizonte (MG), foram selecionados. Entre 2002 e 2005, 240 pacientes com TB foram identificados. Destes, 117 (48,7%) foram diagnosticados no PA, 72 (61,5%) com baciloscopia positiva. Testes de sensibilidade foram realizados em 90 cepas, sendo 80 (89%) sensíveis, 9 (10%) resistentes e 1 (1%) multirresistente. A incidência de baciloscopia positiva e de TB resistente foi elevada, o que demanda uma adoção urgente de medidas de controle de TB no PA.
Palavras-chave:
Tuberculose; Transmissão de doença infecciosa; Resistência a medicamentos.
The identification of patients with respiratory symptoms in emergency rooms (ERs) is a strategy that has been adopted in hospitals in developed countries, as well as in referral hospitals for infectious diseases in Brazil, with the aim of identifying cases of TB.(1,2) The number of TB cases diagnosed in ERs in hospitals shows either the failure of primary health care clinics in the early detection of these cases in the community or patient preference for treatment in the ER. This occurs mainly due to the fact that Family Health Programs have not been implemented in metropolitan regions, as well as to limited patient access to these programs, patient preference for a specific treatment or late seeking of medical treatment and the existence of more severe clinical profiles associated with comorbidities (transplant recipient status, HIV/AIDS, chronic renal failure, insulin-dependent diabetes mellitus or alcoholism). Other major factors related to the delayed diagnosis and the increase in nosocomial transmission include the lack of training of the professionals in detecting patients with respiratory symptoms, as well as the lack of infrastructure for the respiratory isolation of patients suspected of having pulmonary TB in hospital facilities in developing countries.(3,4)
In the United States, due to the resurgence of TB in the 1980s and beginning of the 1990s, several outbreaks of nosocomial TB were described in patients and in health professionals. In subsequent years, the adoption of administrative and engineering measures in the control of infection with Mycobacterium tuberculosis was prioritized. These measures included the following: training of health professionals in conducting screening and early detection of patients with respiratory symptoms; and the subsequent isolation of such patients in negative pressure rooms. Such measures have been shown to be cost-effective in the control of nosocomial TB transmission.(5)
In a recent study of resistance to anti-TB drugs, involving 595 patients treated at six hospitals in the state of Rio de Janeiro between 2004 and 2006, the prevalence of multidrug-resistant TB (MDR-TB) was found to be high (3.9%) among the 433 patients with no history of previous treatment.(6) Such data indicate the urgent need for the implementation of strategies to avoid TB transmission in hospitals in Brazil. In 2005, one group of authors discussed the difficulty of implementing screening procedures in general hospital ERs in São Paulo, stating that it is necessary to consider other methods, such as syndromic surveillance for pulmonary diseases, or other forms of continuing education.(7)
The flow of admissions to the Hospital das Clínicas da Universidade Federal de Minas Gerais (HC-UFMG, Federal University of Minas Gerais Hospital das Clínicas) is principally through the ER. During the study period, an average of 3,400 patients per month and 240 patients per day were treated in the ER, which has 6 treatment rooms and 55 short-stay beds (being capable of accommodating up to 70 such beds). There was no respiratory isolation, no active investigation of respiratory symptoms, no standard instructions given to health care professionals on requesting sputum smear microscopy/culture for mycobacteria, no use of surgical masks by suspected TB patients, no use of special masks by health professionals and no requests for HIV serology in patients suspected of having pulmonary TB. Therefore, the aim of this study was to evaluate the number of cases of TB, confirmed by bacteriology, admitted to the ER of the HC-UFMG, the susceptibility of M. tuberculosis strains isolated from those patients, as well as the TB control measures employed.
The study was conducted from January of 2002 to December of 2005 in the ER of the HC-UFMG. Patients were selected based on positive bacteriological results in the records of the Mycobacteriology Laboratory of the HC-UFMG. Sputum smear microscopy was conducted using the Ziehl-Neelsen/fluorescence techniques on Löwenstein-Jensen medium, and species were identified through biochemical methods.(8)
Strain susceptibility to rifampin, isoniazid, pyrazinamide, streptomycin, ethambutol and ethionamide was tested at the Ezequiel Dias Foundation referral center in the state of Minas Gerais, using the proportion method, on Löwenstein-Jensen medium.(8)
The M. tuberculosis strains resistant to rifampin and isoniazid were defined as MDR-TB, as described in the international literature.(9)
The study design was approved by the Ethics in Research Committee of the UFMG (Process no. 162/01).
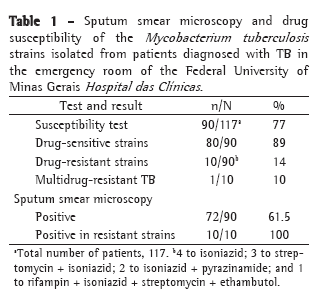
Among the 297 patients identified in the registry of the Mycobacteriology Laboratory, M. tuberculosis strains were isolated in 240 (81%), nontuberculous mycobacteria (NTM) strains were isolated in 46 (15.5%), and the minimum data required for the analysis were missing in 11 (3.5%). Of the 46 patients with NTM, 6 (13%) presented positive smear microscopy. Of the 240 patients with M. tuberculosis, 117 (48.7%) were treated in the ER and 123 (51.2%) were treated in the outpatient wards of the HC. Among the 117 M. tuberculosis strains isolated from the patients treated in the ER, drug susceptibility testing was conducted in 90 M. tuberculosis isolates (77%), of which 80 (89%) were sensitive to all of the drugs tested, 9 (10%) were resistant to certain drugs (4 to isoniazid; 3 to streptomycin and isoniazid; and 2 to isoniazid and pyrazinamide), and 1 (1.1%) was classified as MDR-TB (resistant to rifampin, isoniazid, streptomycin and ethambutol). Of the 117 patients treated in the ER, sputum smear microscopy was performed in 72 (61.5%), of whom 10 (14%) harbored drug-resistant strains (Table 1).
In the present study, we observed that most (80%) of the patients infected with mycobacteria harbored M. tuberculosis, as has been described by other authors.(1,3) Of the patients in whom a bacteriological diagnosis had been made, 48.7% had been treated in the ER, of which 61.5% were bacilliferous and 14% harbored drug-resistant strains. In the study period, administrative and engineering measures proposed by the National Ministry of Health at the end of 2004 had not yet been adopted.(2) In Brazil, analyses regarding the adoption of such measures of TB control in hospitals are rare, despite these being the point of entry for 30% to 40% of the cases of TB reported in large metropolitan centers.(10) The Rio de Janeiro State Pulmonology Health Council reported that the vast majority of deaths related to TB or TB/HIV occurred in hospitals in the city of Rio de Janeiro, in locales where there were no coordinated TB and TB/HIV control activities.(4) This scenario reflects the low priority that public health officials in developing countries give to the control of TB in hospitals.
Since the 1950s, with the advantage of outpatient treatment over hospitalization for the treatment of the disease, the closing of sanatoriums where these patients were treated was prioritized. Only recently, with the outbreaks of MDR-TB and extensively drug-resistant TB that have occurred in hospitals in Eastern Europe and South Africa, there is a consensus that TB control in hospitals should be given high priority, in developed and developing countries alike.(11)
Various studies have reported TB transmission in health care clinics, principally in hospitals receiving cases of high complexity and treating HIV-infected patients.(6,12-15) A survey conducted in public and private hospitals in seven large cities in Asia and Northern Africa showed that these hospitals, with the exception of those in Bangkok, did not conduct outpatient treatment in accordance with the recommendations of the local TB programs. The treatment offered was not always free to patients, the large number of hospitals never reported TB cases, there were no standardized regimens, and the evolution, as well as the outcomes, of the cases were unknown.(3)
One of the limitations of our study lies in the fact that the number of patients with respiratory symptoms and the proportion of bacilliferous patients treated in the ER during the study period are unknown. In an analysis conducted in 2006 at the HC-UFMG, it was observed that, of the patients having been under observation in the ER, 33.2% had remained for less than 24 h; 53.5% had remained from 1 to 5 days; and 13.5% had remained for more than 5 days. During that same period, patients with respiratory symptoms were not identified nor submitted to respiratory isolation, health professionals and other patients confined to the same environment, the latter often immunocompromised and with a higher risk of acquiring infection with M. tuberculosis, therefore being extensively exposed to patients with active pulmonary TB.(1,16) As previously reported by other authors, when the health team is unaware of TB cases in the hospital and health officials are unaware of the prevalence of drug-sensitive and drug-resistant TB in the hospitals they oversee, it is difficult to implement the necessary changes for the early identification of the disease and the use of measures for individual protection, which greatly increases the risk of infection with M. tuberculosis.(17,18)
After the data of the present study were disclosed, the medical staff of the HC-UFMG began to take administrative measures for the control of TB, such as the syndromic identification of TB, new ways of reporting data, as well as new forms of training and sensitization of professionals, as suggested by other authors.(9,16,18,19) From July of 2007 onward, after a training session had been given to health professionals and laboratory technicians, sputum smear microscopy results for ER patients and hospitalized patients began to be released in 4 h, as proposed by the World Health Organization and adhered to by most authors.(9-19)
Another relevant finding of our study was the high occurrence of drug-resistant TB (15.3%), similar to that described in other studies that analyzed the resistance profile of patients seen in hospitals and prisons.(6,9,12,14,15,17) This calls for making methods for the rapid diagnosis of drug-sensitive and drug-resistant TB available, as soon as possible, in large metropolitan centers and tertiary-care hospitals that treat patients under suspicion of TB, with or without other comorbidities. The majority of general hospitals do not have culture media for mycobacteria and even fewer perform anti-TB drug susceptibility testing. In such facilities, priority is given to the testing of strains for their susceptibility to drugs used against pyogenic germs, under the control of the cross infection committees, which typically fail to conduct TB surveillance.
AcknowledgmentsWe would like to thank the staff members of the HC-UFMG Mycobacteriology Laboratory (Roberto Silva, Delma Pereira, Adão Damasceno and Terezinha Nogueira de Souza) for their contribution.
References 1. White VL, Moore-Gillon J. Resource implications of patients with multidrug resistant tuberculosis. Thorax. 2000;55(11):962-3.
2. Sociedade Brasileira de Pneumologia e Tisiologia. II Diretrizes Brasileiras para Tuberculose. J Bras Pneumol. 2004;30(Suppl 1):S21-S56.
3. Chiang CY, Trébucq A, Billo N, Khortwong P, Elmoghazy E, Begum V, et al. A survey of TB services in hospitals in seven large cities in Asia and North Africa. Int J Tuberc Lung Dis. 2007;11(7):739-46.
4. Brito RC, Carvalho RM, Siqueira-Batista R, Bethlem EP, Beivlaqua AA, Kritski AL, et al. Recomendações da Assessoria de Pneumologia Sanitária do Estado do Rio de Janeiro para controle de tuberculose em hospitais gerais. Pulmão RJ. 2003;12(3):169-73.
5. Leonard MK, Egan KB, Kourbatova E, White N, Parrott P, Del Rio C, et al. Increased efficiency in evaluating patients with suspected tuberculosis by use of a dedicated airborne infection isolation unit. Am J Infect Control. 2006;34(2):69-72.
6. Brito RC. Resistência aos fármacos antituberculose em cepas de Mycobacterium Tuberculosis isoladas de pacientes atendidos em seis hospitais da região metropolitana do Estado do Rio de Janeiro, Brasil [thesis]. Rio de Janeiro: Universidade Federal do Rio de Janeiro; 2008.
7. Resende MR, Sinkoc VM, Garcia MT, Moraes EO, Kritski AL, Papaiordanou PM. Indicators related to delays in diagnosis and in implementation of measures to control airborne infection among patients with pulmonary tuberculosis in a tertiary-care hospital. J Bras Pneumol. 2005;31(3): 225-30.
8. Brasil. Ministério da Saúde. Fundação Nacional de Saúde; Centro de Referência Prof. Hélio Fraga. Manual de bacteriologia da tuberculose. 2a ed. Rio de Janeiro; 1994.
9. Jensen PA, Lambert LA, Iademarco MF, Ridzon R; CDC. Guidelines for preventing the transmission of mycobacterium tuberculosis in health-care setting, 2005. MMWR Recomm Rep. 2005;54(RR-17):1-141.
10. Lucca ME. Análise epidemiológica da tuberculose e co-infecção HIV/TB em Ribeirão Preto-SP, de 1998-2006 [dissertation]. São Paulo: Universidade de São Paulo; 2008.
11. Stop TB Partnership (World Health Organization). The global MDR-TB & XDR-TB response plan, 2007-2008. Geneva: World Health Organization, Stop TB Partnership; 2007.
12. Basu S, Andrews JR, Poolman EM, Gandhi NR, Shah NS, Moll A, et al. Prevention of nosocomial transmission of extensively drug-resistant tuberculosis in rural South African district hospitals: an epidemiological modelling study. Lancet. 2007;370(9597):1500-7.
13. Gonçalves ML. Transmissão nosocomial da tuberculose: diminuindo o risco. Bol Pneumol Sanit. 2001;9(2):21-26.
14. Lourenço MC, Silva MG, Fonseca LS. Tuberculose multi-resistente entre pacientes do sanatório penal masculino do Estado do Rio de Janeiro. Brazil J Microbiol. 2000;31(1):17-9.
15. Ruddy M, Balabanova Y, Graham C, Fedorin I, Malomanova N, Elisarova E, et al. Rates of drug resistance and risk factor analysis in civilian and prison patients with tuberculosis in Samara Region, Russia. Thorax. 2005;60(2):130-5.
16. Tokars JI, McKinley GF, Otten J, Woodley C, Sordillo EM, Caldwell J, et al. Use and Efficacy of Tuberculosis Infection Control Practices at Hospitals With Previous Outbreaks of Multidrug-Resistant Tuberculosis. Infect Control Hosp Epidemiol. 2001;22(7):449-55.
17. Guidelines for preventing the transmission of Mycobacterium tuberculosis in health-care facilities, 1994. Centers for Disease Control and Prevention. MMWR Recomm Rep. 1994;43(RR-13):1-132.
18. Cuhadaroglu C, Erelel M, Tabak L, Kilicaslan Z. Increased risk of tuberculosis in health care workers: a retrospective survey at a teaching hospital in Istanbul, Turkey. BMC Infect Dis. 2002;2:14.
19. Uthaivoravit W, Yanai H, Tappero JW, Limpakarnjanarat K, Srismith R, Mastro TD, et al. Impact of enhanced notification of tuberculosis laboratory results to minimise treatment delay, Chiang Rai Hospital, Northern Thailand. Int J Tuberc Lung Dis. 2003;7(1):46-51.
About the authors
Silvana Spíndola de Miranda
Associate Professor I. Department of Clinical Medicine, Federal University of Minas Gerais, Belo Horizonte, Brazil.
Ana Rita de Paiva Toledo
Medical Student. Federal University of Minas Gerais, Belo Horizonte, Brazil.
Simone Rodrigues Ribeiro
Pharmacist. Federal University of Minas Gerais, Belo Horizonte, Brazil.
Izabela Magalhães Campos
Medical Student. Federal University of Minas Gerais, Belo Horizonte, Brazil.
Petra Maria de Oliveira Duarte Sthur
Medical Student. Federal University of Minas Gerais, Belo Horizonte, Brazil.
Afrânio Lineu Kritski
Adjunct Professor of Clinical Medicine. Federal University of Rio de Janeiro, Rio de Janeiro, Brazil.
Study carried out at the Federal University of Minas Gerais Hospital das Clínicas, Belo Horizonte, Brazil.
Correspondence to: Silvana Spíndola de Miranda. Faculdade de Medicina, Departamento de Cínica Médica, Avenida Alfredo Balena, 190, 2º andar, Santa Efigênia, CEP 30130-100, Belo Horizonte, MG, Brasil.
Tel 55 31 3248-9599. E-mail: spindola@medicina.ufmg.br
Financial Support: None.
Submitted: 10 December 2007. Accepted, after review: 16 June 2008.


